预防和24天潜伏期
Prevention, & 24 Day Incubation (lecture 15)
Welcome to another MedCram coronavirus update! So let’s go to the numbers. Again, these are numbers that we take with a grain of salt. These are the numbers that we have. They are coming from the WHO who has been allowed into China as of yesterday, also from the CDC here. We know that these numbers are probably underestimated. We know that because only the most severe cases that made it to the hospital are getting tested. We know that these numbers are underestimated. We don’t know by how much. We may never know how much. Total deaths keep increasing by bigger numbers, 1,018. Total recovered is growing probably the fastest.
欢迎来到另一个MedCram冠状病毒更新!因此,让我们来看数字。再说一遍,这些不一定是准确的数字。这些是我们拥有的数字。他们来自昨天才获准进入中国的世界卫生组织,也来自这里的疾病预防控制中心。我们知道这些数字可能被低估了。我们知道,因为只有送往医院的最严重病例正在接受检查。我们知道这些数字被低估了。我们不知道多少。。。。。。总死亡人数继续增加,增加了1,018。回收的总量可能增长最快。
Okay, let’s go over to our other website that we look at, which is the Worldometer. At least according to these numbers, there is a suggestion that things are layering out.
好的,让我们转到我们关注的另一个网站,即Worldometer。至少根据这些数字,有人暗示事情正在逐步发展。
Let’s go back though to our death cases. That doesn’t seem to be at all petering out. In fact, if we look at the number of deaths here, February 10th deaths total was 108, and that seems to indicate what we’ve been talking about all along, and that is the number of cases usually represent something earlier in the course, and that takes time for the patient to get sick to the point of death, which takes a little bit longer. So hopefully, here in the next week or so, we might start to see death starting to layer out. We can only hope that that’s the case.
让我们回到死亡案例。这似乎根本没有消失。实际上,如果我们看一下这里的死亡人数,那么2月10日的死亡总数为108,这似乎表明了我们一直在谈论的话题,也就是说,在此过程中,案件的数量通常代表着早期,而且要花一些时间才能使病人生病直至死亡,这要花更长的时间。因此,有希望的是,在下一周左右的时间里,我们可能会开始看到死亡开始加剧。我们只能希望是这种情况。
We know that almost all of these deaths are happening in mainland China in the Wuhan area, of course, their system, as with any system, is overwhelmed, inundated, and things that would normally be happening are not happening as they should. They’re trying to alleviate that by building hospitals dedicated to taking care of these more milder symptoms, so they can take the stress off of the hospitals to take care of these more severe cases.
我们知道,几乎所有这些死亡都是在武汉地区的中国大陆发生的,当然,与任何其他系统一样,它们的系统不堪重负,被淹没,而通常会发生的事情并未如期发生。他们试图通过建立专门治疗这些较轻微症状的医院来缓解这种情况,以便他们减轻医院的负担,以应对这些更严重的情况。
So, of course, the big news over the last 24 hours has been about the incubation period. We’re going to get to what to make about the incubation period of 24 days. Before we get to that, the other big news is San Diego, California just got its first case, and interestingly it was from four people that were hospitalized because of symptoms at UC San Diego. And they had done some testing there at UC. San Diego, apparently they went to the CDC, and the CDC released them. But one of these people actually had further testing done, and it turned out to be positive, and which case that patient came right back to the hospital, and they had quarantined them, and everyone’s doing well. It’s just that we have a patient that’s turned positive. And so again, these are people that flew in last Wednesday from China and are being quarantined at the Miramar base, just north of San Diego.
因此,过去24小时的大新闻当然就是潜伏期。我们将探讨24天的潜伏期。在此之前,另一个大新闻是加利福尼亚圣地亚哥,这是第一个病例,有趣的是,有四个人因为加利福尼亚大学圣地亚哥分校的症状而住院。他们在加州大学做了一些测试。圣地亚哥,显然他们去了CDC,而CDC释放了他们。但是其中一个人实际上进行了进一步的检查,结果是肯定的,并且在这种情况下,患者被送回医院,并且已经对其进行了隔离,每个人的状况都很好。只是我们有一个病人变得积极。同样,这些人是上周三从中国飞来的,并在圣地亚哥北部的Miramar基地被隔离。
So let’s talk about this quarantine issue. Actually, the quarantine issue, which is related to the incubation period. So up to this point was felt that 14 days was enough to take care of any potential type infection. In fact, that’s where the recommendation came for just about anyone in the world now that is coming from China. They are quarantine them because the incubation period is about 14 days.
因此,让我们谈谈隔离问题。实际上,隔离问题与潜伏期有关。因此,到目前为止,人们认为14天就足够照顾任何潜在的类型感染。实际上,这就是针对现在来自中国的世界上任何人的推荐。它们被隔离,因为潜伏期约为14天。
Well, there was this new paper that was published pre peer-reviewed. What does that mean? That means that before a bunch of scientists that are in that field got to look at the paper, pick it apart, and say what about this? What about that? It got published on a server, and it’s out there. Let’s talk about it.
好吧,有一篇新的论文是在同行评审之前发表的。这意味着什么?这意味着在该领域的一群科学家必须先研究论文,将其拆开并说出什么来之前?那个怎么样?它已发布在服务器上,并且在那里。让我们来谈谈它。
So here is the article, the lead author whose name actually goes at the end is this gentleman Nanshan Zhong. This is a pulmonologist. And you know, I’ve got a soft spot in my heart for pulmonologist because I am one, and here’s the abstract for it. And then here’s the key part. It says the median incubation period was three days range of 0 to 24.0 days.
所以这是文章,最后一位真正叫名字的主要作者是这位先生南山钟。这是一名肺科医生。而且您知道,我对肺病科医生心里情有独钟,因为我是其中之一,这是摘要。然后是关键部分。它说中位潜伏期为三天,范围是0到24.0天。
And of course, they went into a lot of other things. So some things I want to point out here, which is really interesting, is if you were to see our update from yesterday, where we actually quoted the JAMA article. The JAMA article was a publication that looked at 138 patients that were seen in the hospital there in Wuhan.
当然,他们还做了很多其他事情。因此,我想在这里指出的一些事情真的很有趣,那就是您是否要看昨天的更新,我们实际上引用了JAMA文章。 《美国医学会杂志》(JAMA)的一篇文章研究了武汉市医院中的138名患者。
This one actually looks at 1099 patients. So you’re going to get a much bigger and number. That was at 1 hospital; this is 552 hospitals in 31 provinces through January 29, 2020. So here the median age as compared to the JAMA article was a little bit younger. That was in the 50s; this was 47 years of age. In this case, there was a bigger majority that were males. In the previous one, it was more split half and half. We saw about the same number of people with fever, people with cough. We also saw that diarrhea was uncommon, but it did happen.
这实际上是针对1099名患者。因此,您将获得更大的数量。那是在一家医院。到2020年1月29日,这是31个省的552家医院。因此,与JAMA文章相比,这里的中位年龄要年轻一些。那是在五十年代。这是47岁。在这种情况下,男性占大多数。在上一个中,它被分成了一半和一半。我们发现发烧和咳嗽的人数大致相同。我们还看到腹泻很少见,但确实发生了。
But there are ome other interesting things. We saw that lymphopenia, that means low white blood cells were observed. That seems to be a very common finding in any type of viral infection, but in the JAMA article, which was looking at a hundred thirty-eight patients in a single medical center. In that situation, there were 36 patients, or 26 percent, that were admitted to the Intensive Care Unit. Here, only 55 patients, or 5%, were admitted to the Intensive Care Unit.
但是,还有一些其他有趣的事情。我们看到了淋巴细胞减少症,这意味着观察到低白细胞。在任何类型的病毒感染中,这似乎都是很常见的发现,但在JAMA的文章中,该文章仅在一个医疗中心检查了138名患者。在这种情况下,重症监护病房收治了36名患者,占26%。在这里,只有55名患者(即5%)被送入了重症监护室。
Let me explain that. Again, the larger study that had more patients in it, and was more of a cross-section of the area, had a much lower admission rate to the Intensive Care Unit, only 5%. And whereas in our JAMA article, 4.3% died at least at the time of publication, the mortality rate here in this publication was only 1.36. So it seems as though the patients included in this study were not as severe.
让我解释一下。再次,较大的研究中有更多的患者,并且是该区域的横截面,重症监护病房的入院率要低得多,仅为5%。而且,尽管在我们的JAMA文章中,至少有4.3%的人在发布时死亡,但此处的死亡率仅为1.36。因此,似乎这项研究中包括的患者并不那么严重。
So, what do we say about this 24 days? Let’s talk about that. The first thing you need to look at is that the median incubation period was 3.0 days. So what would make that outlier exist? Well, they asked the WHO doctor at a press conference on the 10th that very same question, and the response was that sometimes what can happen is there is a reinfection later on, that makes the exposure look longer than it really is. In fact, they’ve seen this in Ebola where there’s a double exposure, and sometimes what can happen is there is a reinfection later on that makes the incubation period look longer than it really is.
那么,这24天我们要怎么说?让我们来谈谈。您需要查看的第一件事是中值潜伏期为3.0天。那么,什么使该异常值存在呢?好吧,他们在10日的一次新闻发布会上向世卫组织医生问了同样的问题,答复是有时可能发生的事是稍后再进行感染,这会使接触时间长于实际时间。实际上,他们在埃博拉病毒中曾见过两次接触,有时可能发生的是稍后再感染,使潜伏期看起来比实际更长。
So what we mean to say there’s an infection that occurs here on day Zero, and then there’s an incubation period here, or let’s say 10 days incubation period, and then there’s another repeated one, and this one may not cause symptoms, but this repeated one may cause symptoms, and that will be another incubation period, and then let’s say this one happens to be 14 days, and then symptoms occur.
因此,我们的意思是说在第零天在这里发生了感染,然后在这里有一个潜伏期,或者说是十天的潜伏期,然后又有一个重复的重复,这个重复可能不会引起症状,但是重复一次一个人可能会导致症状,那将是另一个潜伏期,然后假设这恰好是14天,然后才出现症状。
And so they can clearly identify this as one of the potential infection periods, and they look at this, of course, as the symptoms. What they don’t realize though is that there is another infection that occurred and that the total, when added up, yes, it comes out to 24 days. But that’s not the incubation period of this infection to this symptom. There is another one there.
因此,他们可以清楚地将其识别为潜在的感染期之一,并且可以将其视为症状。他们没有意识到的是,又发生了另一种感染,总的来说,是24天。但这不是这种症状的感染潜伏期。那里还有另一个。
It’s an interesting concept. This is an outlier. And so sometimes you will get outliers, right? There is always a bell-shaped distribution, with most things that as anyway, and so yes, is it possible that you’re going to get an outlier here at the 99th percentile or the first percentile? It’s possible. But it seems as though at least at this point, what we’re talking about in terms of a median, is three days on the incubation period. What we’ll do is we’ll put a link in to the video where the reporter asks the WHO physician about exactly what does this 24 day incubation period means.
这是一个有趣的概念。这是一个离群值。因此有时您会出现异常值,对吗?总会有一个钟形分布,无论如何,大多数情况还是如此,是的,您是否有可能在第99个百分点或第一个百分点得到异常值?这是可能的。但似乎至少在这一点上,我们所说的中位数,是潜伏期的三天。我们要做的是在视频中添加一个链接,记者在该视频中向WHO医生询问这24天潜伏期的确切含义。
Okay. So let’s talk a little bit more about what’s happening, and what it is that we can do. So we spent some time, if you look at our previous videos, talking about things that we can do to help us prevent getting the virus, and that’s what a lot of expenditures going into right now, quarantining, shutting down.
好的。因此,让我们再谈一些正在发生的事情以及我们可以做什么。因此,我们花了一些时间(如果您观看我们以前的视频),谈论我们可以采取哪些措施来帮助我们预防病毒,这就是现在用于隔离,关闭和关闭系统的大量支出。
But we’ve also talked about what is the treatment that can occur if somebody actually comes down with the coronavirus and they have symptoms that are severe enough that end them up in the hospital. We’ve already talked a little about some of the medications, and we’ll talk more about some of these medications that are being used.
但是,我们还讨论了如果有人真的感染了冠状病毒并且他们的症状严重到足以使他们最终住院的话,该如何治疗。我们已经讨论了一些药物,并且还将讨论一些正在使用的药物。
Realize that medications that are used for diseases at least in the United States or in Europe have to go through rigorous placebo-controlled trials for them to be indicated for that. So in other words, if you have a blood pressure medication, or you have an antibiotic, it has to be tested for that particular indication for it to work.
意识到至少在美国或欧洲,用于疾病的药物必须经过严格的安慰剂对照试验才能明确表明。因此,换句话说,如果您使用降压药或抗生素,则必须对其进行特定适应症的测试以使其起作用。
Now, we can’t do this with a brand-new coronavirus. We will never have randomized placebo-controlled trials ready to go at the initiation of an outbreak. They are planning to have something maybe in April, and that’s really, really fast for some of these medications, but we don’t have anything that we know is going to work, and so as a result of that whenever we give something for treatments, unless a known situation like ARDS, because viral pneumonia can cause ARDS, that’s acute respiratory distress syndrome, there are some treatments that we know work.
现在,我们无法使用全新的冠状病毒做到这一点。在爆发爆发时,我们永远不会准备进行随机的安慰剂对照试验。他们计划在四月份开药,对于某些这类药物来说确实非常快,但是我们没有什么知道会起作用的,因此,每当我们给一些药物治疗时,除非有像ARDS这样的已知情况,否则由于病毒性肺炎会导致ARDS(即急性呼吸窘迫综合征),因此我们知道一些有效的治疗方法。
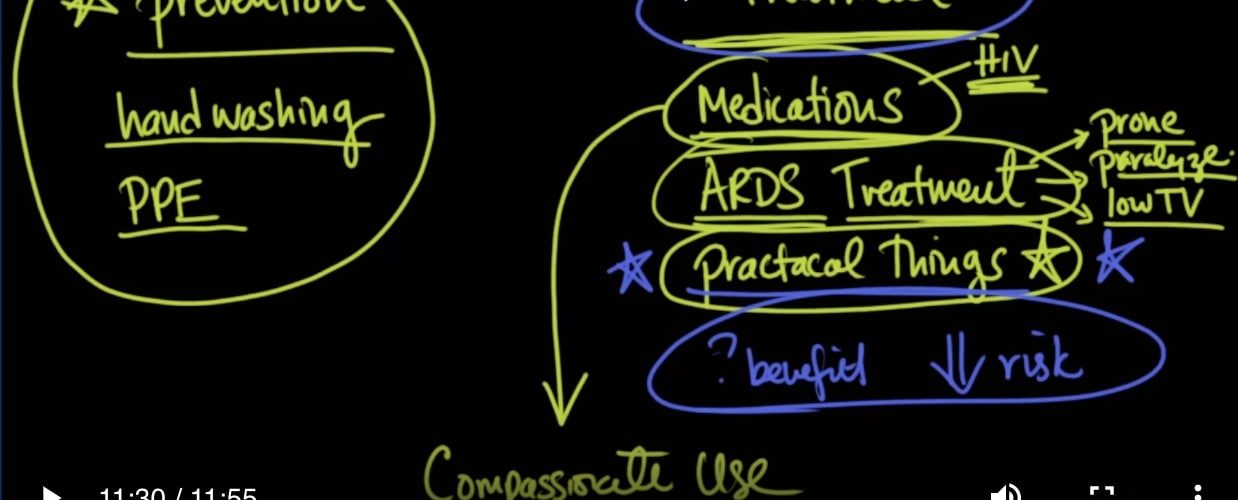
We’ve talked about this in our video, which I will give you a link to How Coronavirus Kills. There’s something that we can do called prone positioning, there’s something that we can do called paralysis, and there’s also something called low tidal volumes. So all of these are things that we can do to help improve because that’s been a randomized placebo-controlled trial for ARDS, but in terms of medications for this coronavirus, we don’t have practical things that we can do. We don’t have randomized placebo-controlled trials, which are the best evidence for these things.
我们已经在视频中谈到了这一点,我将向您提供有关冠状病毒如何杀死的链接。我们可以做的事情叫做俯卧位,我们可以做的事情叫做瘫痪,还有一些叫做低潮气量的事情。因此,所有这些都是我们可以帮助改善的事情,因为这是针对ARDS的随机安慰剂对照试验,但是就这种冠状病毒的药物而言,我们没有可以做的实际事情。我们没有随机的安慰剂对照试验,这是这些事情的最好证据。
So what do we do instead? We look at the biology of things, and we make certain choices, and we say, yes, even though we know that we don’t know for sure if this is going to work, we’re still going to try it anyway because there’s very little risk. So, for instance, for medications that have indications for other diseases, for instance, HIV, it may work in coronavirus. And so what we’ll do is we’ll do this, and it’s called compassionate use, and you have to apply for that to use it.
那么我们该怎么办呢?我们着眼于事物的生物学,做出某些选择,然后说,是的,即使我们知道我们不确定是否能奏效,但还是要尝试一下,因为风险很小。因此,例如,对于具有其他疾病迹象(例如HIV)的药物,它可能在冠状病毒中起作用。因此,我们要做的就是做到这一点,这称为同情使用,您必须申请使用它。
And so that’s what happened in this case in the gentleman in Thailand where they used medications that were typically indicated for HIV. They used it to see if the man would get better, and that’s the kind of things that we have now. Basically, anything that we say we’re going to throw at in terms of a medication against coronavirus, it’s going to be compassionate use.
这就是泰国绅士在这种情况下发生的情况,他们使用了通常用于HIV的药物。他们用它来看看这个人是否会变得更好,这就是我们现在所拥有的东西。基本上,我们说过要针对冠状病毒使用的任何药物,都将具有同情心。
We’re not going to have the best evidence to say it’s going to work. So what I would like to do over the next couple of videos, and we’ve talked about this before, is to look at some practical things that the biology tells us may work. But can I tell you for sure that it’s going to help you? No. So what are those things? The things that will fit into the category where there is ? benefit, but very low risk. These are the kinds of things that you can concentrate on to help you if you are ever in the situation where you have coronavirus.
我们将没有最好的证据说它会起作用。因此,我想在接下来的两个视频(我们之前已经讨论过)中做的是看一些生物学告诉我们的可能有用的东西。但是,我可以肯定地说这会对您有所帮助吗?不,那是那些东西?符合类别的事物在哪里?受益,但风险很低。如果您患有冠状病毒,可以通过这些方式来帮助您。
What is it that you can do beforehand, and at the point of, to limit the morbidity and mortality. And I’m telling you right now; you’re going to be surprised at some of the things. But I’m going to show you the evidence for it, and you may say NO, really? Could that really help me? Well, we’ll go over the evidence, and you make your final decision, and if the benefits outweigh the risks, then you should do it. Thanks for joining us!
您可以事先做些什么,以限制发病率和死亡率。我现在告诉你;您会对某些事情感到惊讶。但是我将向您显示证据,您可能会说不,真的吗?真的可以帮到我吗?好吧,我们将检查证据,由您做出最终决定,如果收益大于风险,则应该这样做。感谢您加入我们!




Add comment