医院感染比例及原因,N-95口罩使用
Hospital Spread of Infection, WHO Allowed in China, & N-95 Masks (Lecture 14)
Welcome to another MedCram coronavirus update! So I wanted to go over the recent numbers. And total deaths is a 910. That means that it’s surpassed SARS. Total recovered is a good three and a half times now. The total number of deaths about a week ago, they were substantially below the total number of deaths. So we’re seeing an improvement here in the total number of recovered.
欢迎来到另一个MedCram冠状病毒更新!所以我想回顾一下最近的数字。总死亡人数是910。这意味着它已经超过了SARS。如今,回收的总量是三倍半。大约一周前,死亡总数大大低于死亡总数。因此,我们看到恢复的总数有所改善。
Now, these numbers are provided to us from the WHO, the CDC and a number of other agencies. Recently here, there’s been some news that China seems as though, but the WHO is now being allowed to go in, and that team is being headed up by Dr. Bruce. Aylward, according to the New York Times article. If we look here, or the others, that they have listed. Here is actually on the cruise ship just south of Tokyo. You can see that there.
现在,这些数字已从WHO,CDC和其他许多机构提供给我们。最近在这里,有一些消息似乎表明中国好像是中国,但是现在允许世卫组织进入,而布鲁斯博士正在领导该小组。据《纽约时报》报道,艾尔沃德。如果我们看这里,或者其他人,他们已经列出了。这实际上是在东京南部的游轮上。您可以在那里看到。
I wanted to talk about a recent article that was just published in JAMA, the Journal of the American Medical Association, on February 7th, and we will put a link in the description below that links to the article. I think it’s an excellent article, and basically it’s a description of a hundred thirty-eight patients that were admitted to University Hospital in Wuhan and describes exactly what happened to them.
我想谈谈2月7日刚刚发表在JAMA上的最新文章,即《美国医学会杂志》,我们将在下面的描述中添加一个链接到该文章。我认为这是一篇很棒的文章,基本上是对武汉大学医院收治的138名患者的描述,并准确描述了他们所发生的事情。
This is an article that looked at patients that were admitted from the first of January until the 28th of January. And at this hospital, there was a total of 138 patients. How do they diagnose these? All of these were positive for coronavirus, but they did not look at serum viral titers or serum viral load. They looked at sputum.
本文探讨了从1月1日至1月28日收治的患者。在这家医院,总共有138名患者。他们如何诊断这些?所有这些对于冠状病毒都是阳性的,但是他们没有看血清病毒滴度或血清病毒载量。他们看着痰。
So that’s one of the weaknesses of the study. The other thing I want to mention here is that these are a hundred thirty-eight patients that were sick enough to come to the hospital. That’s really important to understand because this is going to give you a limited look at what happens to patients who are sick enough to come to the hospital and seek medical attention.
因此,这是该研究的弱点之一。我想在这里提及的另一件事是,这些一百三十八名病人病得很重,可以去医院就诊。理解这一点非常重要,因为这将使您对生病到医院就医的患者的病情了解有限。
So what they noticed in the article is that first of all the patient has symptoms, then they typically developed shortness of breath, then they became admitted to the hospital, and then after they were admitted to the hospital, one of two things happened: either they were admitted to the Intensive Care Unit or they were admitted to the regular floor.
因此,他们在文章中注意到的是,首先,患者有症状,然后通常会出现呼吸急促,然后被送进医院,然后在入院后发生了两件事之一:他们被送往重症监护病房,或被送往常规病房。
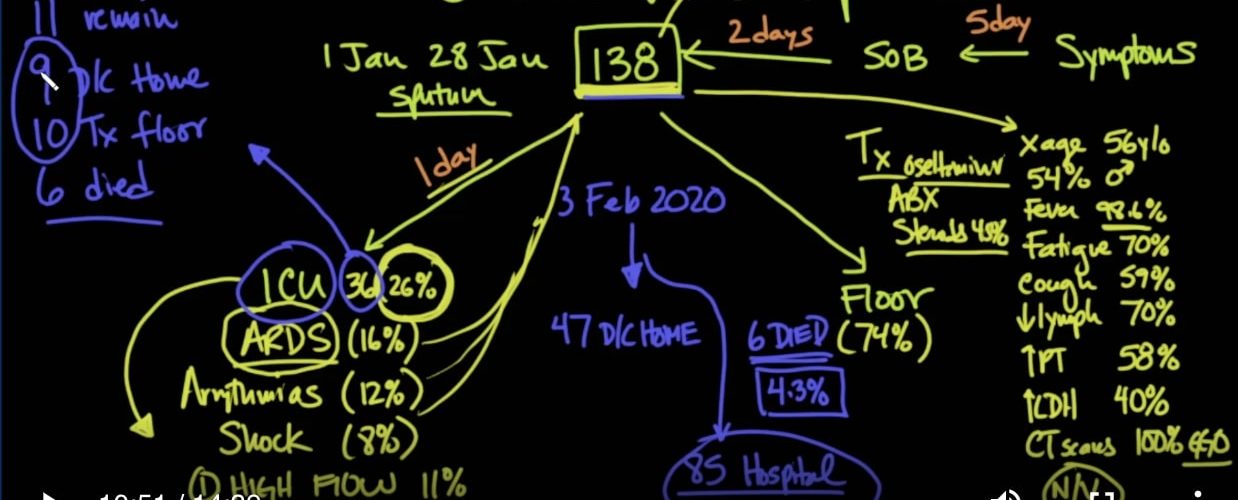
And then we’ll talk about where it goes from there. Now, in terms of timing, that’s important to get to as well. From the time of symptoms to the time of shortness of breath was about five days according to their survey, and then from shortness of breath to admission here at the 138 was two days on average, and then from admission to intensive care, if they were going to go to the Intensive Care, was one day.
然后,我们将讨论它的去向。现在,就时间而言,这也很重要。根据他们的调查,从症状发生到呼吸急促的时间大约为五天,然后从呼吸急促到住院时间平均为2天,然后从住院到重症监护是1天。
So let’s talk about what those symptoms were. First of all, the average age of patients admitted into the study was 56 years old, and unlike previous reports that showed a real high predilection to men, only 54 percent of these patients were male. When I say ONLY, look more like a 50-50 kind of mix as opposed to 60 or 70 that have been shown before.
因此,让我们谈谈这些症状是什么。首先,入选该研究的患者的平均年龄为56岁,与以前的报告显示男性的真实偏爱不同,这些患者中只有54%是男性。当我只说时,看起来更像是50-50种混合物,而不是之前显示的60或70种混合物。
So what were the symptoms? Fever was seen in 98.6 percent of the patients, kind of an ironic figure given that 98.6 degrees Fahrenheit is the average temperature for human being. Aa fever is defined by the way as a temperature of greater than 100.4 Fahrenheit or 38 degrees Centigrade. Fatigue was seen in about 70% of patients; cough was seen in 59 percent of patients; low lymphocytes, what we call lymphopenia, a common sign that you can see in viral infections, that that was seen in as high as 70% of patients. Prothrombin time, a PT, that sort of a measure of the blood’s ability to coagulate, and when you have a high PT, that means that your blood is a little bit more thin, and that was seen in about 58 percent of patients; and elevated lactate dehydrogenase, which is another lab value typically seen in viral infections, that was seen in about 40%.
那是什么症状呢?在98.6%的患者中发现了发烧,这具有讽刺意味,因为98.6华氏度是人类的平均温度。发烧定义为温度高于100.4华氏度或38摄氏度。大约70%的患者出现疲劳; 59%的患者出现咳嗽;低淋巴细胞,我们称为淋巴细胞减少症,这是您在病毒感染中可以看到的常见征兆,在70%的患者中都可以看到。凝血酶原时间(PT)是一种衡量血液凝结能力的指标,当您的PT高时,意味着您的血液会变得稀薄一些,约有58%的患者看到过;乳酸脱氢酶升高,这是病毒感染中常见的另一个实验室值,约为40%。
Now when they looked at CT scans, 100% of those patients have what they call ground glass opacities, that’s inflammation in the lungs and that’s consistent with what we would see in a viral pneumonia of any type. So in other words, what we’re seeing here is not very specific for coronavirus, but could in fact be seen in the flu, could be seen in other types of viruses that could do this.
现在,当他们进行CT扫描时,其中100%的患者称其为毛玻璃样混浊,即肺部发炎,这与我们在任何类型的病毒性肺炎中所见一致。因此,换句话说,我们在这里看到的不是针对冠状病毒的,但实际上可以在流感中看到,也可以在其他可以做到这一点的病毒中看到。
One of the things that they saw is that there was a substantial amount that had just nausea and vomiting, and that was kind of unusual. It wasn’t as high as 80 to 90%, but it was there.
他们看到的一件事是,许多患者恶心和呕吐,这是很不寻常的。它没有高达80%到90%,但是在那里。
In terms of treatment for these patients, almost all of them received oseltamivir, which is a flu medication; also, antibiotics were used on the majority, and in about 45 percent of patients steroids were used. They weren’t really able to tell whether or not any of this stuff had a benefit to the patient. Of course, this study was not designed to look at that.
就这些患者的治疗而言,几乎所有人都接受了奥司他韦(一种流感药物);同样,大多数人都使用了抗生素,大约45%的患者使用了类固醇。他们无法真正分辨出这些东西是否对患者有益。当然,本研究并非旨在研究该问题。
So let’s look at the 138 patients that came in. The first thing I’m going to mention to you, and we’re going to talk about this at the end, I think this is probably the biggest thrust and the biggest surprise out of this paper, was that 41 percent of these patients, or total of 57 patients, were patients that did not come to the hospital with the coronavirus, but in fact picked it up there. We call that a nosocomial infection.
因此,让我们看一下这138名患者。我首先要向您提及的是这件事,我们将在最后进行讨论,我认为这可能是最大的推动力和最大的惊喜。在本文中,这些患者中有41%或总共57位患者不是携带冠状病毒到医院就诊的患者,而是实际上是在那儿捡到的。我们称这是医院感染。
So yes, there were patients at the hospital that were there for a completely different reason, and they developed coronavirus at the hospital, and there were health care workers that went to work without coronavirus and picked it up taking care of patients at the hospital.
因此,是的,医院里的病人完全有不同的原因,他们在医院内感染了冠状病毒,还有一些医护人员上班时都没有冠状病毒,并在医院照顾病人。
What percent of the patients in the hospital that were treated for coronavirus had that? A substantial; amount 41%! We’ll talk about that at the end of this presentation. So of these 138 patients, regardless of whether or not they came to the hospital with it or not, or develop that there, what happened to them?
医院中接受过冠状病毒治疗的患者中有百分之多少?实质性的金额41%!在本演示文稿的结尾,我们将对此进行讨论。那么,在这138名患者中,无论他们是否随便一起去医院或在那里发展,他们都发生了什么?
So of the 138, and on average after about one day, there was a decision to have them moved to the Intensive Care Unit. About 36 patients, or 26 percent, of the 138 went to the Intensive Care Unit, and 74% were stable enough to be admitted to the regular floor.
因此,在138名患者中,平均大约一天后,决定将他们转移到重症监护室。 138名患者中约有36名患者(占26%)去了重症监护病房,而74%的患者病情稳定到可以接受常规就诊的水平。
So let’s focus our time a little bit on what happened to the patients in the Intensive Care Unit. So why did they have to go to the Intensive Care Unit? Well, there are many reasons why somebody could go to the Intensive Care Unit. For instance, they could go into ARDS; they could have serious arrhythmias, or they could go into shock.
因此,让我们把时间集中在重症监护病房的病人身上。那么,为什么他们必须去重症监护室呢?嗯,有人可以去重症监护病房有很多原因。例如,他们可以进入ARDS;他们可能患有严重的心律不齐,或者可能会休克。
Sometimes you can have more than one of these things, so don’t expect all of these things to add up. But if you look at of the 138, how many of them had ARDS? 16 percent of patients admitted to the hospital have to go to the Intensive Care units for ARDS reasons. Of the people who are admitted, 12% of the 138 had arrhythmias, and eight percent of people admitted to the hospital had to go to the Intensive Care Unit because of shock.
有时您可以拥有以上这些东西之一,所以不要期望所有这些东西加起来。但是,如果您查看这138个,则其中有多少人患有ARDS?由于ARDS原因,入院的患者中有16%必须去重症监护病房。在138名住院患者中,有12%患有心律不齐,而入院的患者中有8%由于休克不得不去重症监护室。
Now if you want more information on ARDS, please look at our ARDS video, How Coronavirus Kills, and that describes what ARDS is in detail. And what are the treatments that the Intensive Care Unit can use to treat these kinds of things?
现在,如果您想了解有关ARDS的更多信息,请观看我们的ARDS视频,《冠状病毒如何杀死》,其中详细介绍了ARDS。重症监护病房可以使用哪些治疗方法?
Now, of those that went to the Intensive Care Unit, what kind of oxygen supplementation do they need? There are three basic types of oxygen supplementation that you’ll see in the Intentional Care Unit. One is known as high-flow oxygen. The other is non-invasive positive pressure ventilation. This is kind of like CPAP, but it’s actually called BiPAP because the ventilator helps you when you take a breath in, so it gives you a higher pressure when you’re breathing in, and lower pressure when you’re breathing out. We call that non-invasive positive pressure ventilation, and then, of course, full-out ventilators.
现在,在去了重症监护室的人中,他们需要什么样的氧气补充?在意向监护室中,您会看到三种基本的氧气补充类型。一种被称为高流量氧气。另一个是无创正压通气。这有点像CPAP,但实际上称为BiPAP,因为呼吸机在您吸气时会为您提供帮助,因此在吸气时它会给您带来更高的压力,而在呼气时给您带来更低的压力。我们将其称为无创正压通气,然后将其称为全通气呼吸机。
So of those people that went to the Intensive Care units, how many have to go on high-flow? 11%. How many have to go on non-invasive positive pressure ventilation basically wearing a tight mask? 42%. And how many actually have to go on the ventilator? Up to almost half the patients, 47%. And of those people, 4 patients have to go on ECMO. ECMO is basically where you bypass the heart and lung on a machine to oxygenate the patient until their lungs get on inflamed, or they recover from the infection.
那么,那些去了重症监护病房的人中,有多少人必须坚持高流量? 11%。基本上要戴好口罩的无创正压通气要进行多少次? 42%。到底有多少必须使用呼吸机?多达近一半的患者,占47%。在这些人中,有4名患者必须接受ECMO。基本上,ECMO是您在机器上绕过心脏和肺部给患者充氧的方法,直到患者的肺部发炎或从感染中恢复过来。
So overall, you can see that these patients, which were fully in the phase of the viral infection where patients were coming to the hospital, they were very sick. We can see here that of the 138, a quarter of these patients, more than a quarter, are going to the Intensive Care Unit, meaning that this cohort look to be a little bit sicker than previous descriptions.
因此,总的来说,您可以看到这些完全处于病毒感染阶段的病患,他们正在医院就诊,他们病得很重。从这里我们可以看到,在138名患者中,有四分之一(超过四分之一)要去重症监护病房,这意味着该队列看起来比以前的描述病了一些。
Again, I caution you to understand that this 26 percent is not 26 percent of all people who get coronavirus infection, but rather 26 percent of people who get coronavirus infection and then develop symptoms severe enough to have to have them into the hospital.
再次提醒您,我要理解的是,这26%的人并不是冠状病毒感染者的26%,而是26%的冠状病毒感染者并出现严重症状以致不得不将其送入医院。
So let’s talk about what’s happened to these patients. So the last update, as of February 3rd, 2020, let’s get an update, of all of these 138 patients, 47 patients have been discharged home. There have been six patients that have died, and the remaining 85 patients are still in the hospital. So, the six that have died out of the 138 leaves us with a mortality of about 4.3 percent. That’s the base of the mortality based on the hospitalization because we don’t yet know what’s going to happen to these 85 patients.
因此,让我们谈谈这些患者发生了什么。因此,让我们来更新一下截至2020年2月3日的所有138位患者,其中47位患者已出院。已有6名患者死亡,其余85名患者仍在医院。因此,在138人中死亡的6人使我们的死亡率约为4.3%。这是基于住院治疗的死亡率的基础,因为我们尚不知道这85名患者将会发生什么情况。
Let’s talk a little bit about what happened to these people in the ICU specifically. So there were 36 people that went into the Intensive Care Unit. What has happened to them since they were admitted to the hospital? Well, of those 36 patients, we know based on the report that 11 still remain in the Intensive Care Unit, that nine have been actually discharged home, that 10 have gotten well enough to be transferred to the floor, and that all of the six that died, all of them were in the Intensive Care Unit.
让我们谈谈ICU中这些人发生的事情。因此,有36人进入了重症监护室。自他们入院以来,他们发生了什么事?好吧,在这36名患者中,根据报告,我们知道,重症监护病房中仍有11名患者,有9名实际上已经出院,有10名患者状况良好,可以转移到地板上,而所有6名患者死了,他们都在重症监护室。
So you can see here that of the 36 that initially came in, nineteen of them have improved to the point where they are either gone home or on the regular floor, and 11 still remain, and we’re going to see where that goes.
因此,您可以在此处看到最初引入的36个服务,其中19个已经改善到可以回家或呆在常规地板上的程度,还有11个仍然存在,我们将拭目以待。
Okay, let’s talk about 57 patients of the 143, or 41% of them, develop the infection in the hospital. Of those 57, 17 of them were actual patients that were in the hospital for another reason, but a full 40 of these were healthcare workers.
好吧,我们来谈谈143位患者中有57位患者(占41%)在医院内感染的情况。在这57名中,有17名是由于其他原因住院的实际患者,但其中有40名是医护人员。
Let’s go back to these 17 patients that were there. They said that 7 of them were on the surgical ward, and that 5 of them were on the internal medicine ward, and that 5 of them were on the oncology ward. Now, of these 40 patients that were actually healthcare workers there at the hospital, 31 of them, or 78%, were working on the wards. 7 of them, or 18%, were in the emergency room, and 2, or 5%, were working in the Intensive Care Unit.
让我们回到那里的这17位患者。他们说,其中7人在外科病房中,其中5人在内科病房中,其中5人在肿瘤病房中。现在,在这40名实际上是医院医护人员的患者中,其中31名,即78%,正在病房工作。其中有7人,即18%,在急诊室,有2人,即5%,在重症监护室工作。
They talked about in the paper, about 1 patient who presented with nausea and vomiting, which we said was kind of a typical, and he was admitted to the surgical ward while he had coronavirus, and they believe based on history and based on deductive reasoning that about 10 people were infected because of his symptoms and his virus.
他们在论文中谈到,大约有1位患者出现恶心和呕吐,我们说这是很典型的,他患有冠状病毒时被送往外科病房,他们相信基于病史和演绎推理由于他的症状和病毒,大约有10人被感染。
So what this paper highlights, I think, is the transmissibility of this virus. And what we really need to highlight here is hand washing, and the key here is that you’ve got to wash for 20 seconds, and as we’ve said before that’s like singing Happy Birthday twice. Wash your hands with soap, and you need to do this before, of course, before you go into a patient’s room, before you put on gloves, before you are done a gallon, and you need to do it after. And why is that? Because you’re using your hands to take off your personal protective equipment that would have the virus on there and really avoid touching your face with your hands.
因此,我认为本文强调的是该病毒的可传播性。我们真正需要强调的是洗手,这里的关键是您必须洗20秒,就像我们之前所说的那样,就像唱两次生日快乐。用肥皂洗手,当然,这需要在进入患者房间之前,戴上手套之前,完成XX之前以及之后进行。为什么是这样?因为您正在用双手脱下可能会感染病毒的个人防护设备,所以真正避免用手触摸脸部。
Now, what about masks? Well, if you are suspicious that the person that you are about to examine has the coronavirus, and you are a healthcare worker, they’re recommending n95 masks. If you suspect that the patient is the one that has the virus, then they ought to be wearing a regular surgical mask in addition to n95 masks. So this is for the patient, and this is for you. As a healthcare worker, you should also be doing eyewear protection. And you can see what the workers over in China are now currently wearing. They got the message. They understand what it is that’s going on, and they’re going to make sure that that doesn’t happen again.
现在,口罩怎么样?好吧,如果您怀疑要检查的人患有冠状病毒,并且您是医护人员,则建议使用n95口罩。如果您怀疑患者是感染病毒的患者,那么除了n95口罩外,他们还应该戴常规的外科口罩。所以这是给病人的,也是给你的。作为医护人员,您还应该保护眼镜。您会看到中国工人现在穿着什么。他们收到了消息。他们了解发生了什么,并且将确保不会再次发生。
And what this article, I think, really shows is the delicate balance that you have to strike when you have patients with a virus coming into a setting where there are other patients that don’t have the virus. And I believe that is really the thrust as to why they are building these hospitals dedicated to the virus so that they don’t cross-infect other people, other health care workers, and that they can have the infrastructure in place to deal with the contamination that can occur in these places.
我认为,这篇文章真正显示的是,当有病毒患者进入其他患者没有该病毒的环境时,您必须达到微妙的平衡。我认为,这确实是他们为什么要建立这些专门针对该病毒的医院的推动力,以便它们不会交叉感染其他人,其他医护人员,并且他们可以拥有适当的基础设施来应对这种病毒。这些地方可能发生污染。
Please stay tuned for other videos that we’re going to really delve into what it is that you either as a healthcare individual, or as a citizen, can do to improve your chances of not getting the virus. Or number two: if you do get the virus, beating it. So stay tuned for those videos coming up.
请继续收看其他视频,我们将深入探讨您作为医疗保健个人或公民可以提高您没有感染病毒的机会的意义。或第二点:如果您确实感染了病毒,那就击败它。因此,请继续关注即将到来的视频。




Add comment