名称更改为COVID-19,增强您对病毒感染的免疫反应
Name Change to COVID-19, Boosting Your Immune Response to Viral Infections
点击这里观看视频翻译。
Welcome to another MedCram coronavirus update! And we’ve got some news today. This is for the 12th of February 2020. So the new name that the WHO has given the virus is called SARS-CoV2, and the disease that it causes is being known as covid-19. So that’s the new nomenclature. This is the name of the virus, and this is the name of the disease, sort of like HIV and AIDS. This is the virus, this is the disease.
欢迎来到另一个MedCram冠状病毒更新!今天我们有一些新闻。这是2020年2月12日。因此,世卫组织赋予该病毒的新名称称为SARS-CoV2,其引起的疾病被称为covid-19。这就是新的术语。这是病毒的名称,这是疾病的名称,有点像艾滋病毒和艾滋病。这是病毒,这是疾病。
And let’s take a look at the update. Again, just the word about these numbers. We believe these numbers are probably under-reporting here. We don’t know how much they’re underreporting. It’s because only the most severe cases in China are actually being tested. If you look here of the total deaths and total recovered, that leaves another 40,000 people that are somewhere between death and totally recovered. So only time is going to be able to tell that.
让我们看一下更新。再说一遍,只是关于这些数字的字眼。我们认为这些数字可能在这里被低估了。我们不知道xxx多少。这是因为实际上只有xx最严重的病例正在接受测试。如果您在此处查看死亡总数和已恢复的总数,那么还有40,000人处于死亡和完全恢复之间。因此,只有时间才能证明这一点。
If we go to our friends over at Worldometers, you’ll see here a nice graph of where we are and total cases. We can see that it’s kind of been leveling off a little bit. If we go to the log rhythmic, you can see again a little bit more of a leveling off. It is unclear whether or not that is related to the number of test kits like we were talking about, or whether or not there’s an actual leveling off. It’s kind of interesting to see. Something that they’ve added, that we talked to them about, is this case outside of China, and we’ll get to that here.
如果我们在Worldometers拜访我们的朋友,您会在这里看到一个很好的图表,显示了我们的状况和总案件数。我们可以看到它有点趋于平稳。如果我们以对数律动,则可以再次看到稳定的水平。目前尚不清楚这是否与我们所谈论的测试套件的数量有关,或者是否与实际水平持平。看起来很有趣。我们与他们讨论过的是他们添加的一些东西,这是在中国境外的案例,我们将在这里进行讨论。
So we go down to the bottom of this page. Now they start looking at total cases excluding mainland China. And in terms of those cases, we are not seeing a leveling off but more of still this epidemic. So it looks as though things are still taking off outside of China. We are not seeing an asymptotic leveling off but rather still going up. When we look at cases per day, we can see here that just in the last couple of days we’ve had the most number of cases outside of China being diagnosed.
因此,我们进入此页面的底部。现在,他们开始研究不包括中国大陆在内的全部案例。就这些情况而言,我们没有看到稳定的趋势,但更多的是这种流行病。因此,似乎中国境外仍在起飞。我们没有看到渐近平稳的趋势,而是还在上升。当我们每天查看病例时,我们可以看到,在过去的几天中,我们在中国以外被诊断出的病例数量最多。
I want to talk a little bit about the viral infection itself and immunity. For that, we’re going to draw out a little bit of a schematic here how this happens. So the first thing that happens is, of course, you have this virus particle, which will draw as stars, and these stars are outside the body, so this could be an airway, this could be inside the GI tract, etc., etc. So this virus goes in and latches onto cells receptors, and it causes the cells to become infected with the virus, and of course, the virus takes over the machinery of the cells, and it causes it to make more of it and proteins, and so these cells will be coded with these proteins on the outside.
我想谈谈病毒感染本身和免疫力。为此,我们将在此处画出原理图的一点点。因此,首先发生的事情当然是您具有此病毒颗粒,该颗粒将像星星一样吸引,并且这些星星在体外,因此这可能是呼吸道,可能在胃肠道内,等等。因此,这种病毒进入并闩锁在细胞受体上,导致细胞感染该病毒,当然,该病毒接管了细胞的机械,并使其制造更多的蛋白质,因此这些细胞将在外面被这些蛋白质编码。
And of course, more particles are made. These cells explode and they release more and more of these virus particles. So what is going on at this point is you’ve got here on the blood side, you’ve got things called cells, which are blood cells, and one of those cells is called an antigen-presenting cell. And so these cells start to go in and extravasated from the blood into the tissue, and they’re able to recognize these cells that are abnormal because of these abnormal proteins on the surface. So, these antigen-presenting cells envelop and destroy these virally infected cells.
当然,会产生更多的粒子。这些细胞爆炸,并释放出越来越多的病毒颗粒。因此,此时发生的事情是,您在血液里有称为细胞的东西,它们是血细胞,而其中的一种细胞称为抗原呈递细胞。因此,这些细胞开始进入并从血液中渗入组织,并且它们能够识别出由于表面上的这些异常蛋白质而异常的这些细胞。因此,这些抗原呈递细胞包裹并破坏了这些病毒感染的细胞。
So let’s show a little bit more of a close-up of how that happens. So we have this antigen-presenting cell, and inside the antigen-presenting cell is the cell that is infected with virus, and it’s got virus particles on it. And so what’s very important with this antigen-presenting cell does is it presents the antigen. So here is the antigen presented on the outside of that cell. This is the most important thing that the antigen-presenting cell can do because what it then does is it meets up with something called a TH1 response, or a CD4+ cell. And this cell here is the mastermind behind your cellular mediated immunity because this antigen here will latch on to this CD4 positive TH1 cell, and it will release Il-12, which is a chemical that comes from the antigen-presenting cell, that stimulates this cell to go and fight anything that looks like this on it, that antigen.
因此,让我们展示一下这种情况的特写。因此,我们有了这个抗原呈递细胞,并且在抗原呈递细胞内部是感染了病毒的细胞,上面有病毒颗粒。因此,这种呈递抗原的细胞非常重要的是呈递抗原。因此,这是存在于该细胞外部的抗原。这是抗原呈递细胞可以做的最重要的事情,因为它所要做的就是遇到一个叫做TH1反应或CD4+细胞的东西。这个细胞是细胞介导免疫力的策划者,因为这里的抗原将锁存在CD4阳性TH1细胞上,并释放出IL-12,这是一种来自抗原呈递细胞的化学物质,可刺激这种细胞去对抗任何看起来像它的抗原。
And so there’s major responses that can occur. Number one is that these TH1, CD4 cells will then stimulate another type of cell called the cd8 cells, and those are killer cells, and they go out, and all they do they will kill any cell that has those antigens on it. That’s a very important thing, and the way that that happens is it has little proteins on the surface that will recognize this and cause docking to occur. So you want that connection to be very, very tight.
因此,可能会发生重大反应。第一个是这些TH1 CD4细胞将刺激另一种称为cd8细胞的细胞,这些细胞是杀伤细胞,它们会消失,它们所做的一切将杀死所有带有这些抗原的细胞。这是非常重要的事情,并且发生的方式是表面上几乎没有蛋白质可以识别并导致对接。因此,您希望该连接非常紧密。
Another thing that this TH1 can do is it can stimulate, in the blood and tissue, B cells and these B cells will produce antibodies that look like this, and these antibodies will bind to these antigens and neutralize them. So this really is immunity. And this is the key that allows you to survive a viral infection.
TH1可以做的另一件事是,它可以刺激血液和组织中的B细胞,这些B细胞将产生看起来像这样的抗体,并且这些抗体将与这些抗原结合并中和它们。所以这确实是免疫力。这是使您能够抵抗病毒感染的关键。
Let me be very clear about this. This is probably one of the most important things that you can have going for you when you have a viral infection; this is what determines whether or not you get admitted to the floor, or whether or not you go to the Intensive Care Unit, because if this reaction does not occur correctly, and this immunity doesn’t get on top of the viruses quickly and limit them, kind of quarantining this, then you get wide viral infections all over the body, and the amount of infection causes more immunity which causes more inflammation, and that’s why people die.
让我对此非常清楚。这可能是病毒感染时最重要的事情之一。这是决定您是否可以住院或进入重症监护病房的原因,因为如果这种反应未正确发生,并且这种免疫力无法迅速超越病毒并受到限制将它们隔离,然后您会在全身传播广泛的病毒感染,并且感染的数量会导致更多的免疫力,从而导致更多的炎症,这就是人们死亡的原因。
And so, while the best way to prevent you from ending up having something bad happen from coronavirus is to avoid getting the virus in the first place. If you do get coronavirus, you want your immune system working perfectly. And wouldn’t it be nice if there was something that we could do to enhance this Il-12 response to enhance the ability of this binding to occur, to enhance the ability of cd8 killer cells to bind their targets and to destroy, to enhance the ability of TH1 CD4 cells to create and stimulate actually these B cells to make antibodies?
因此,预防冠状病毒最终导致某些不良后果的最佳方法首先是避免感染该病毒。如果您确实感染了冠状病毒,则希望您的免疫系统运转正常。如果我们可以做些什么来增强这种Il-12反应,从而增强这种结合的发生能力,增强cd8杀伤细胞结合其靶标的能力,并破坏,增强这种能力,那不是很好吗? TH1 CD4细胞产生并实际上刺激这些B细胞产生抗体的能力。
Well, there actually is something that we can do that can enhance this. Number one. It’s not a drug. Number two. It’s absolutely free. There’s no money involved. Number three, you can do it anywhere. And I’m sure by this point, you’re probably saying what possibly could this be? And are you pulling my leg on this? This is probably one of the biggest things that you can do to protect yourself from this viral infection causing a problem, or any other viral infection, and there are absolutely no side effects to it, and the answer is sleep.
好吧,实际上我们可以做些事情来增强这一点。第一,这不是药品。第二,它是完全免费的。第三,您可以在任何地方进行操作。我确定到这一点,您可能是说这可能么?这不是扯淡吗?这可能是您可以采取的最大措施,以保护自己免受这种引起问题的病毒感染或任何其他病毒感染的侵害,并且绝对没有副作用,而答案就是睡眠。
That’s right. Sleep, and enough of it, greatly enhances the ability of the antigen-presenting cell binding to the TH1 and promoting Il-12; sleep also prevents the breaking up of this binding site with cd8 killer cells with the antigen. I will show you the research that’s done this. I have peer-reviewed papers in extensive research over the last 20 years that sleep has a tremendous effect on your immune response against viruses.
睡觉以及足够的睡眠可以大大增强抗原呈递细胞与TH1结合并促进II-12的能力;睡眠还可以防止这种结合位点与具有抗原的cd8杀伤细胞的分裂。我将向您展示完成此工作的研究。在过去的20年中,科学家进行了广泛研究并发表了大量的的同行评审论文,这证明了睡眠对您的病毒免疫反应具有巨大影响。
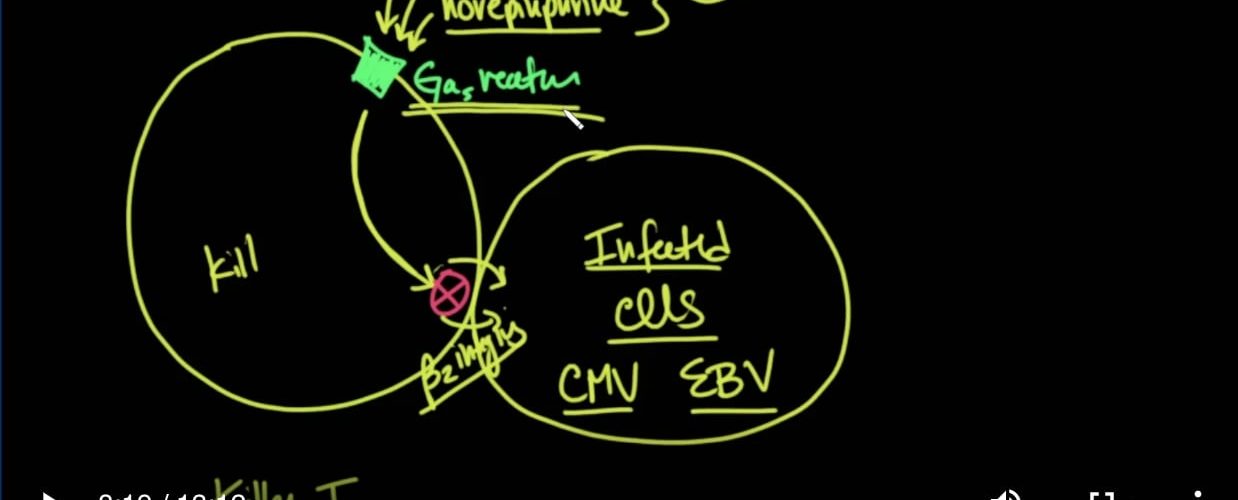
I will show you a paper here. Here we have on the left side a cytotoxic T cell. This is the cd8 cells. This is the cells that kill. And here we have an infected cell with either CMV or EBV in the paper. So what they showed was that there is a G-protein receptor here on the cell, and when it is activated by either isoproterenol, epinephrine, or norepinephrine. These are hormones typically that are elevated in wakefulness; that these wakefulness hormones would activate this receptor in the killer T cells, and it would cause an inhibition of these beta 2 integral proteins that allow binding to these infected cells and destruction.
我在这里给你看一篇论文。我们在左侧有一个细胞毒性T细胞。这是cd8细胞。这是杀死细胞。在本文中,我们有一个感染了CMV或EBV的细胞。因此,他们的研究结果显示,细胞上存在一个G蛋白受体,当它被异丙肾上腺素,肾上腺素或去甲肾上腺素激活时, (这些是通常会提高清醒性的激素)这些清醒激素会激活杀伤性T细胞中的该受体,并会抑制这些β2整合蛋白,从而使它们与这些感染细胞结合并破坏它们。
And so the opposite was true when the patients were sleeping because these hormones were at very low levels that prevented the inhibition of this Gas, G protein which caused better binding and more effective killing of these infected cells.
当患者入睡时情况正好相反,因为这些激素的含量非常低,阻止了这种Gas,G蛋白的抑制,从而导致了这些感染细胞更好的结合和更有效的杀死它们。
So do you know how much sleep in adults in the United States should be getting? According to the recommendations, and you can look this up at the CDC, they should be getting between seven and nine hours a night. Do you know how many people actually get at least 7 hours of sleep per night? About 60 percent. That means there’s about 30 to 40 percent of us that are getting less than seven hours a night. These are the people that are at the highest risk for the effects of sleep deprivation, and these are exactly the same conditions that a lot of our health care workers in the United States are under. These are physicians; these are nurses; these are respiratory therapists who are chronically sleep-deprived because of shifts, because of working at night, and these are the ones that are gonna be on the front line dealing with this virus.
那么,您知道美国成年人应该获得多少睡眠吗?您可以在CDC(美国疾控中心)上查询一下,他们应该每晚有7到9个小时。您知道每晚实际上有至少7个小时的睡眠的人数吗?大约百分之六十,这意味着我们中大约30%至40%的人每晚的睡眠时间少于7个小时。这些人最容易遭受睡眠剥夺的风险,而这些正是我们美国许多医护人员所面临的相同挑战。这些是医师;这些是护士;这些是呼吸治疗师,他们由于轮班或在夜间工作而长期睡眠不足,而这些人将成为第一线应对这种病毒的人。
Think about a lot of the physicians that are working in China right now, and all of this is to the detriment of their immune system. At the beginning of the night when you go to sleep, normally, let’s say around 10:00 p.m., the first thing that occurs is that you should be having more slow-wave sleep at the beginning of the night, and towards the end of the night more REM sleep.
想想现在在中国工作的许多医生,所有这些都损害了他们的免疫系统。通常,在晚上入睡的晚上(例如晚上10:00左右),发生的第一件事是,您应该在夜晚开始时和睡眠结束时进行更多的慢波睡眠。晚上更多的REM睡眠。
Well, they’re starting to see that slow-wave sleep is integral in the production of growth hormone, and growth hormone has tremendous effects on immunity. And this is especially involved, as the papers will show, that I’ll upload to the description, in the secretion of Il-2 12, which is what we recall is the thing that causes the antigen-presenting cell to stimulate the TH1 response with the CD4 cells. So that’s tied to slow-wave sleep. This is the sleep right here that occurs, generally speaking, between 10 p.m. and 1 a.m. in the morning. And this is the sleep that we cut off the most by going to bed late. And so we’re losing out on growth hormone, and our immunity stinks because of it.
好了,他们开始看到慢波睡眠是生长激素生产中不可或缺的部分,而生长激素对免疫力具有巨大影响。正如论文将显示的,这尤其涉及到,我将在Il-12的分泌物中上载到描述中,我们记得这是导致抗原呈递细胞刺激TH1反应的物质。 CD4细胞。因此,这与慢波睡眠有关。这就是通常在晚上10点左右-凌晨1点发生的睡眠。但我们经常失去这些睡眠,也就是说我们失去了生长激素,因此我们的免疫力出了问题。
I want you to think what’s happened to our ability to sleep over the last number of decades. So this is when we would normally go to sleep, around 9:00 to 10:00 p.m., and occasionally people would wake up in the middle of the night and be awake for a little bit and then they would get up again in the morning, around 5:00 to 6:00 a.m. This is the time that we used to have for sleeping. And how much time is that? So for about 9 to 5 would be about eight hours of sleep according to the CDC and most of the research. Plenty of time! But what’s happened? Because we’ve moved away from an agrarian society to more of urban society. We’ve had to push this back because we have to get up earlier because of traffic. And what’s happening is we’re living out in the suburbs. We’re living further out, and all the jobs are in the cities, and so there’s traffic, and so sleep has taken a big toll there, and we’re not able to get as much sleep.
我希望您考虑一下过去几十年来我们的睡眠能力发生了什么。因此,这是我们通常在晚上9:00到10:00睡觉的时间,偶尔人们会在半夜醒来,清醒一会儿,然后早晨又会起床。 ,大约在凌晨5:00到6:00之间,这是我们过去睡觉的时间。那是多少时间?根据CDC和大多数研究,晚9:00至早5:00睡眠时间约为8个小时。充足的时间!但是发生了什么事?因为我们已经从农业社会转移到更多的城市社会。我们不得不将其推迟,因为由于交通原因,我们必须提早起床。而且正在发生的事情是我们住在郊区。我们生活在更远的地方,所有工作都在城市里,所以人流量大,因此睡眠在这里造成了巨大的损失,我们无法获得足够的睡眠。
But on the other side, there’s also been a push. And why is that? Because of electricity. And the other thing is electronics. So think about iPad, smartphones in general, 20 years ago, television, movies, internet, all of those sorts of things. And so the key here though is all of this is light that is stimulating the eyes, and when you stimulate the eyes with bright light, it pushes your circadian rhythm and delays it, and so what you’re losing out on is sleep there. And so what’s happened is we’ve gone from society where we were getting eight hours of sleep before, and now getting five to six hours of sleep. That is going to translate into decreased immunity.
但还有电和电子产品的推动。为什么是这样?因为用电。另一件事是电子产品。因此,请考虑一下iPad,20年前的智能手机,电视,电影,互联网以及所有类似的东西。因此,这里的关键是所有这些都是刺激眼睛的光线,当您用明亮的光线刺激眼睛时,它会推动您的昼夜节律并延迟它,因此您失去的就是在那里睡觉。因此,发生的事情是我们已经离开了以前已经能睡八个小时的社会,而现在仅有五到六个小时的睡眠。这将导致免疫力下降。
So the question is, how can we get this back? Because I believe this is one of the things that we can do in the face of this coronavirus, that we don’t have to ration, we don’t have to worry about “do we have enough of this to go around for everybody in an epidemic?” because this is something that’s available to everybody, is getting plenty of sleep to help with immunity.
所以问题是,我们怎样才能回到过去?因为我相信这是面对这种冠状病毒我们可以做的事情之一,我们不必定量分配资源,我们不必担心“我们是否有足够的钱来满足每个人流行病期间的需求?”因为这是每个人都拥有并可以使用的东西,所以要获得充足的睡眠以帮助提高免疫力。
In addition to me being a pulmonary and critical care specialist that takes care of the unfortunate effects of the virus with people with ARDS and on the ventilator, I also happen to be a sleep specialist, and I know that there are a lot of people out there that have problems with sleeping. Some have insomnia, some have sleep apnea, some have a number of these things. And for each person, it might be an individual thing, but there are some basic things that we can do to improve our sleep.
除了我是一名肺部和重症监护专家之外,我还负责治疗呼吸道疾病和呼吸窘迫综合征(ARDS)以及呼吸机对人的不利影响,我也恰好是一名睡眠专家,而且我知道有很多人有睡眠问题。有些人有失眠症,有些人有睡眠呼吸暂停,有些人类似的问题。对于每个人来说,这可能都是一回事,但是我们可以做一些基本的事情来改善睡眠。
And so for the next couple of updates, I am going to talk a lot about coronavirus, or as it’s called now SARS-cov-2, or COVID-19. But we’re also going to talk about practical things that we can all do as individuals to help bolster our immunity, and be prepared for anything that might come. Thanks for joining us!
因此,在接下来的几个更新中,我将谈论冠状病毒,或者现在称为SARS-cov-2或COVID-19。但是,我们还将讨论一些实际的事情,作为个人,我们所有人都可以做些事情,以帮助增强我们的免疫力,并为可能发生的一切做好准备。感谢您加入我们!




Add comment