确诊病例中增加及睡眠抵御新冠感染
Spike in Confirmed Cases & Fighting Infections with Sleep (Lecture 17)
Welcome to another MedCram coronavirus update. Just wanted to review SARS-COVID-2 is the name of the virus, and covid-19 is the name of the illness that the virus is causing. That’s an important distinction because up to this point, the criteria for a confirmed case has been looking at the RNA using PCR (polymerase chain reaction) technique in test kits specifically for this virus.
欢迎来到另一个MedCram冠状病毒更新。只是想查看一下SARS-COVID-2是病毒的名称,而covid-19是该病毒引起的疾病的名称。这是一个重要的区别,因为到目前为止,确诊病例的标准一直是在专门针对该病毒的测试试剂盒中使用PCR(聚合酶链反应)技术研究RNA。
What they’re noticing, of course, is that they don’t have enough kits to test everybody. As a result of that, and this has been a major push there in Wuhan, China, is to look at something that is not as specific, but as much easier, much more rapidly, able to make that assessment, and that’s looking at the illness, and parts of the illness, the characteristics of the illness, is an infiltrate on chest x-ray or CT scan.
当然,他们注意到的是他们没有足够的工具包来测试每个人。结果,这是中国武汉市的一个主要推动力,就是要着眼于没有那么具体但可以更容易,更迅速地进行评估的东西,并且着眼于疾病,疾病的一部分以及疾病的特征是通过胸部X线或CT扫描发现的。
So these lung scans have been central in making the determination of whether or not we’re dealing with the virus. So again, moving from something that’s very specific but takes a long time to make a diagnosis, couple of days to confirm it, versus something that’s very quick but not as specific. In other words, you may catch other things in there, but given the fact that there’s an epidemic, the chances of that happening are pretty low, and the key here is that it’s very fast.
因此,这些肺部扫描对于确定我们是否正在处理该病毒至关重要。再次重申,从非常具体但需要较长时间才能做出诊断的内容转变为几天才能确认诊断,而不是很快但又不那么具体的内容。换句话说,您可能会在其中捉到其他东西,但是考虑到存在流行病的事实,这种情况发生的可能性非常低,而这里的关键是它的速度非常快。
So it looks like today they made that switch, and as a result of that we’re seeing a lot bigger numbers. Let’s go to the numbers. 60,000 now total confirmed cases; 1369 total deaths; total recovered is 6,061, about four times the number of deaths has totally recovered, and I will show that in a little bit what that looks like.
因此,看起来今天他们做出了这种选择,因此,我们看到的数量要多得多。让我们去看看数字。现已确认的病例总数为60,000;总死亡1369人;恢复的总数为6,061,大约是完全恢复的死亡人数的四倍,我将稍微说明一下。
Here’s the WorldOmeter website. Huge jump in cases, and that’s because of the change in the definition. Not much probably has changed in terms of the reality on the ground, as we’ve been saying before this number is probably been underestimating, but it has been systematically underestimating. Now we’ve gone from apples to oranges, where this is probably closer to the true number because now we’re looking at lung scans.
这是WorldOmeter网站。在情况下跳跃很大,这是由于定义的更改。正如我们之前曾说过的那样,这一数字可能没有被低估了,但是就实地而言,实际变化并没有太大变化,但是系统地低估了这一数字。现在我们已经从苹果变成了橘子,这可能更接近真实数字,因为现在我们正在研究肺部扫描。
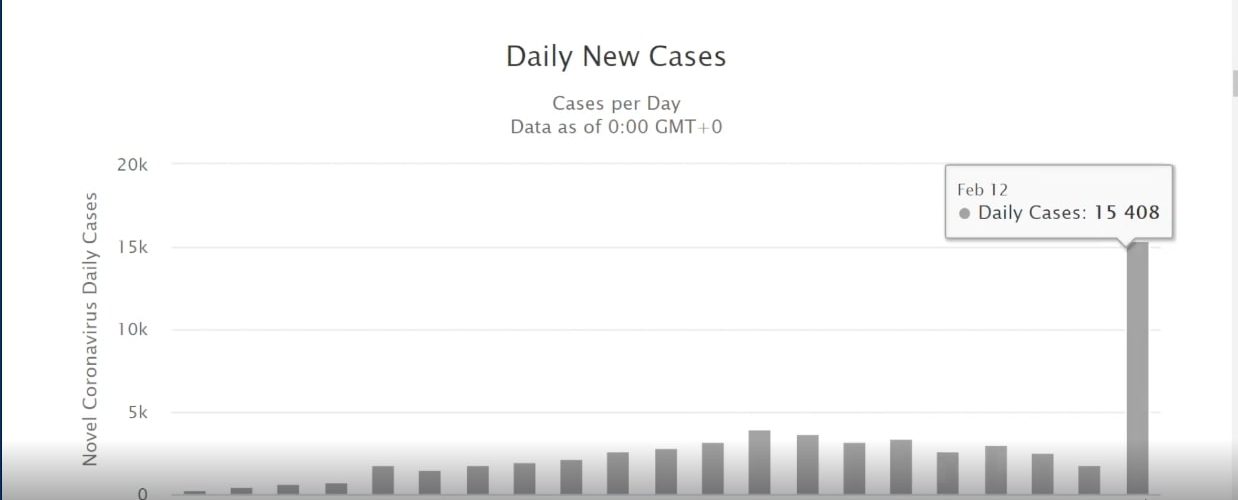
Still, there’s probably a lot of people that haven’t come into the hospital. There could be many people outside of this testing parameter that were not picking up. Let’s keep looking here. In terms of daily cases worldwide, huge jump in the total number of cases.
尽管如此,可能仍有很多人没有来医院。在此测试参数之外,可能有很多人没有接听。让我们继续看这里。从世界范围内的日常案件来看,案件总数急剧增加。
Now, another graph we’ve been looking at here recently is the total cases excluding mainland, China. So what are things looking like? Actually, because we’re not overwhelmed with the number of cases, right? Total cases only 517, we can be very careful, and we can do those RNA tests that are very specific. Again here, some of the smallest numbers to date as of February 12; we will keep watching those numbers as they go.
现在,我们最近在这里查看的另一个图表是不包括中国大陆在内的总案件数。那到底是什么样的?其实,因为我们没有太多的案例,对吗?总共只有517个案例,我们可以非常小心,我们可以进行非常特定的RNA测试。再次强调一下,截止2月12日为止的一些最小数字;我们将继续关注这些数字。
Okay. I want to follow up a little bit more on some of the things that we were talking about before, and that is what we can do in terms of our immunity, and I want to be clear about this. Some of the things that we’ve been talking about in terms of sleep in the last videos, if you haven’t watched these, is that we don’t have any randomized trials for specifically coronavirus. Everything we’re gonna be talking about has to do with what evidence do we have in terms of viruses in general or immunity. I want that to be clear.
好的。我想对我们之前谈论的一些事情进行更多的跟进,这就是我们在抗扰性方面可以做的事情,我想对此进行澄清。在上一个视频中,我们在睡眠方面一直在谈论的一些问题(如果您还没有看过的话)是,我们没有针对冠状病毒的任何随机试验。我们将要谈论的一切都与我们在一般病毒或免疫力方面拥有的证据有关。我想清楚一点。
What we’re looking at here is a methodological way of going through all of the risk factors and trying to reduce our risks in this kind of situation. Remember, in this situation, we don’t have medications or vaccines, and so what is it that we can do to reduce and minimize the risk of becoming infected, and if we are infected, of surviving an infection? So one of the easy things we talked about is sleep, and we made the point last time that by sleeping more, that actually improves the immune system. But we’ve got to realize that not everybody sleeps well, right? Some people have insomnia.
我们在这里看到的是一种方法方法,它可以分析所有风险因素并尝试降低这种情况下的风险。请记住,在这种情况下,我们没有药物或疫苗,那么,我们可以采取什么措施来减少和最小化被感染的风险,以及如果我们被感染,则能够存活下来?因此,我们谈论的最简单的事情之一就是睡眠,而我们上次提出的观点是,多睡,实际上可以改善免疫系统。但是我们必须意识到,不是每个人都睡得好吧?有些人失眠。
The other thing that people don’t realize is that if your body is not ready to go to sleep, and you try to go to sleep and go in bed, what’s going to happen is you’re not going to be able to sleep, and you’re going to get anxiety because you can’t sleep. Then you’re going to associate that with the bedroom. And when you walk into the bedroom, you get more anxious. I’m not going to leave all of you hanging here. There are things that we can do for people who can sleep, people who have insomnia.
人们没有意识到的另一件事是,如果您的身体还没有准备好入睡,而您却试图入睡并上床睡觉,那将会发生的事情是您将无法入睡,而且你会因为无法入睡而焦虑。然后,您要将其与卧室关联。当您走进卧室时,您会更加焦虑。我不会让你们所有人都挂在这里。我们可以为那些可以入睡的人,失眠的人做些事情。
There are many other things that can happen when you’re trying to sleep, including obstructive sleep apnea. There are people that can’t sleep because of medical problems, and I’ll try to address all of those. However, remember that each person is an individual, and we are not here to give out medical advice. So all of this needs to be reviewed with your personal physicians, but there are some guidelines, there are some things that you can do, that are going to help, and we’ll be happy to go over some of those things in general.
当您尝试入睡时,可能会发生许多其他事情,包括阻塞性睡眠呼吸暂停。有些人由于医疗问题而无法入睡,我将尽力解决所有这些问题。但是,请记住,每个人都是个人,我们并不是在这里提供医疗建议。因此,所有这些都需要您的私人医生进行审查,但是有一些指导方针,您可以做一些事情,将对您有所帮助,我们很乐意复习其中的一些内容。
So, I wanted to review another paper that was put out to study by Van Cauter. Basically what they did was they took some healthy men, and on average they were around 23 years of age, and there were some criteria that they had to have.
因此,我想复习Van Cauter提交研究的另一篇论文。基本上,他们所做的就是接受了一些健康的男人,平均年龄在23岁左右,而且必须具备一些条件。
Number 1: No influenza vaccine in the previous three years. And all of them had to have a specific sleep routine. In other words, they normally went to bed between 11:00 p.m. and 1:00 a.m. They typically woke up between 7:00 and 9:00 a.m. And their total sleep time was around 8 hours (+/-) 30 minutes.
1:在过去三年中没有流感疫苗。他们都必须有特定的睡眠程序。换句话说,他们通常在晚上11:00之间上床睡觉。他们通常在早上7:00至9:00醒来,并且他们的总睡眠时间约为8小时(+/-)30分钟。
There were about 25 of these men, and they split them up into two groups. The first group, which had 11, was the Intervention Group. These are the ones that were prevented from sleeping, and then there was another group of about 14 that were the control group.
这些人中大约有25人,他们将他们分为两组。第一组有11名,是干预组。这些是被阻止入睡的人,然后还有另一组,约14人为对照组。
They did something very interesting. Those 11 in the sleep deprivation group were only allowed to sleep for four hours, and they did this for six nights. Whereas the Control Group were allowed to sleep for the eight hours for those same six nights. Then, after those six nights of only four hours sleep per night, they were allowed to sleep for 12 hours to recover, and they did that for seven nights. Here, of course, they were allowed to sleep again for the eight hours for the same seven nights.
他们做了一些非常有趣的事情。睡眠剥夺组中的那11个人只被允许睡四个小时,而他们做了六个晚上。而对照组则被允许在同样的六个晚上睡八个小时。然后,在每晚仅睡四个小时的那六个晚上之后,他们被允许睡12小时以恢复,然后睡了七个晚上。当然,在这里,他们被允许在同样的七个晚上里再睡八个小时。
What they did was they took measurements of antibody titers, and they did it just before they were given an immunization. So I’m going to write here when they were given immunization was on the fourth night, so right here fourth night of minimal sleep, and this was an immunization against the flu vaccine.
他们所做的是他们测量了抗体的滴度,并且在进行免疫接种之前就做了。所以我要在第四个晚上给他们接种疫苗时在这里写,在这里是最小睡眠的第四个晚上,这是针对流感疫苗的免疫接种。
Okay, so flu vaccine given there, and flu vaccine given the same point over here. And what they measured was at this point right here what was the antibody titer to the flu vaccine, and they also measured again 10 days later, and then they measured again 21 to 30 days later.
好吧,所以在那儿接种流感疫苗,在那儿给予流感疫苗同一点。他们此时测量的是流感疫苗的抗体效价,他们也在10天后再次测量,然后在21至30天后再次测量。
So they wanted to see what the effect was of sleep deprivation on the body’s ability to make antibodies against, in this case, the flu vaccine, basically a challenge immunologically to the patient’s immune system. So even though the patients had never had a flu shot before, as we mentioned, in the previous three years, they did have antibodies against the flu because of course people have had the flu in the past. And so there was no Statistical Significant difference here between these two, so there was no difference, and over here on the sleep deprivation side, it was .07, and I’m rounding it off, and over here on the control side it was .09. So there was no Statistically Significant difference.
因此,他们想了解睡眠不足对身体产生抗流感疫苗抗体的能力有何影响,在这种情况下,这基本上是对患者免疫系统的免疫学挑战。因此,即使我们之前提到的患者在过去三年中从未接种过流感疫苗,但他们确实有抗流感的抗体,因为过去人们当然会患上流感。因此,这两者之间在统计上没有显着差异,因此也没有差异,在睡眠剥夺方面,这是.07,我正在四舍五入,在控制方面,这是.09。因此没有统计学上的显着差异。
Now, after the immunization, these people here were sleep-deprived; these people here were not sleep deprived. And so the question is what was the difference here at this point, even though remember now this is 10 days in; they had the ability of recovering some of their sleep even at 12 hours.
现在,在免疫接种之后,这些人在这里睡眠不足。这些人在这里没有被剥夺睡眠。所以问题是,尽管现在记住这是10天了,但此时的区别是什么?他们甚至有能力在12小时后恢复一些睡眠。
So four days into recovery sleep, how much would it be? Well, the tighter here in the sleep deprivation group was .50, whereas the tighter over here on this side was 1.15. It was over twice the amount now when they looked at it after about 21 to 30 days after they had gone both back to a regular sleep schedule. Again, there was no difference in terms of antibody titer.
那么恢复睡眠四天了,要多少钱?好吧,睡眠剥夺组的收紧范围是.50,而这一边的收紧范围是1.15。他们俩都回到正常的睡眠计划后约21到30天,看着它的数量已经是现在的两倍多。同样,抗体效价没有差异。
So they discovered was that sleep deprivation could reduce the body’s ability to fight off the flu as measured by antibodies, but that difference seemed to go away after a period of 21 to 30 days. But please remember that they also stopped the sleep deprivation that they were doing. So the question is what would happen if someone had chronic sleep deprivation.
因此,他们发现睡眠不足会降低身体抵抗流感的能力(通过抗体来衡量),但是这种差异在21到30天后似乎消失了。但是请记住,他们也停止了他们正在做的睡眠剥夺。所以问题是如果有人长期睡眠不足,会发生什么。
Okay, let’s look at another study. This one was by Cohen, et al. In this one, this is a bigger study, they took 153 patients, and they were age 21 to 55 years of age, and they asked them about the previous 14 days of sleep, and they looked at two things. They looked at sleep duration. How long were they sleeping for, and they looked at sleep efficiency.
好吧,让我们看看另一项研究。这是由Cohen等人撰写的。在这项研究中,这是一项规模更大的研究,他们研究了153名患者,年龄在21至55岁之间,他们询问了他们之前的14天睡眠时间,并研究了两件事。他们看着睡眠时间。他们睡了多长时间,他们看着睡眠效率。
And then they put in rhinovirus, one of the viruses that cause the common cold. They dropped in with nasal drops into their nostrils; these drops in to infect them. Okay, so we know exactly how much duration they sleep, their efficiency, and we’re taking 153 of them, and basically inducing a cold, they monitored them for five days, and they looked at the results of it. Two sets of results.
然后他们放入了鼻病毒,这是一种引起普通感冒的病毒。他们用滴鼻剂滴入鼻孔。这些水滴会感染它们。好吧,所以我们确切地知道了他们的睡眠时间长短,他们的效率,我们正在服用其中的153个,基本上是感冒了,他们监视了他们五天,并观察了结果。两组结果。
The first one had to do with duration. Remember we looked at the duration, and we looked at the efficiency. Let’s talk about duration first. They were able to divide them into two categories: those that had less than seven hours of sleep and those that had greater than or equal to 8 hours of sleep in total. Those that had less than seven hours of sleep were anywhere between 1.18 and 7.30 times the likelihood of having cold symptoms, and on average, that was 2.94. So in other words, based on the duration of sleep, if you had less than seven hours, you were on average 2.94 times more likely to develop a cold when exposed to the same exposure than those who slept for greater than eight hours.
第一个与持续时间有关。记住我们看了持续时间,我们看了效率。让我们先讨论持续时间。他们能够将其分为两类:睡眠时间少于七个小时的睡眠者和睡眠时间总计大于或等于8个小时的睡眠者。那些睡眠时间少于七个小时的人,其患感冒症状的可能性在1.18到7.30倍之间,平均为2.94。因此,换句话说,基于睡眠时间,如果您少于七个小时,则与睡了八个小时以上的人相比,在相同的照射下患感冒的可能性平均高出2.94倍。
There was another category and that was efficiency. Now efficiency, sleep efficiency, is simply the amount of time that you are asleep divided by the amount of time that you are in bed. And they divide that into two categories: those that were asleep greater than 98% of the time versus those that were less than 92% of the time. And what they found was that those that slept less than 92% of the time were 5.5 times the likelihood of getting the cold, and that was a range of 2.08 to 14 .48, meaning that it’s not just how long you sleep, but with efficiency you sleep with as well.
还有另一类,那就是效率。现在,效率,即睡眠效率,就是您睡着的时间除以您躺在床上的时间。他们将其分为两类:睡眠时间大于98%的人与睡眠时间小于92%的人。他们发现,睡眠时间少于92%的人患感冒的可能性是5.5倍,范围是2.08到14 .48,这意味着不仅睡眠时间长,而且睡眠时间长您的睡眠效率也很高。
Now when you’re looking at statistics, they noted that it was just these things, duration and efficiency, that made the difference. When they look for confounders, things that did not predict, pre-challenge antibodies did not predict it, demographics, the season of the year, the BMI, the socioeconomic status, and their health or lifestyle, none of those things affected whether or not they got the cold, but the strong predictor was duration and the efficiency of sleep.
现在,当您查看统计数据时,他们指出,正是这些因素,持续时间和效率才有所不同。当他们寻找混杂因素时,没有预料到的事情,挑战前抗体没有预料到的事情,人口统计,一年的季节,BMI,社会经济状况以及他们的健康或生活方式,这些都不会影响他们得了感冒,但最有力的预测因素是持续时间和睡眠效率。
So I believe that even though these two studies are not specifically testing the 2019 coronavirus, I do believe that they do have some appropriate information for us in dealing with what is it that we can do right now in terms of protecting ourselves from the virus and realize that it’s not a 100%. You can still get the virus even though you sleep well, just like some of these people got the cold even though they did sleep, but it was less likely.
因此,我相信即使这两项研究并未专门测试2019年的冠状病毒,但我确实相信它们确实为我们提供了一些适当的信息,以应对我们目前在保护自身免受病毒和病毒侵害方面可以做的事情。意识到这不是100%。即使睡眠良好,您仍然可以感染该病毒,就像其中一些人即使睡觉也得了感冒一样,但是可能性很小。
So the purpose of these last couple of updates was to show you the importance of sleep. Now. The question is what can I do to make my sleep better? And I think that’s what we’re going to attack in the next couple of videos is what is it that you can do personally if you have such and such a problem. Let’s say, you have difficulty falling asleep. Let’s say you have difficulty staying asleep. What are the things that you can do that are fairly simple and effective in making your sleep better?
因此,这最后几次更新的目的是向您展示睡眠的重要性。现在。问题是我该怎么做才能使我的睡眠更好?我认为接下来的几段视频中,我们将要攻击的是如果遇到此类问题,您可以亲自进行处理。假设您难以入睡。假设您难以入睡。您可以做些哪些简单而有效的事情来改善您的睡眠?
Let’s talk about those and also update the news and the numbers as we go through this epidemic. Thanks for joining us!
让我们讨论一下这些问题,并在经历这种流行病时更新新闻和数字。感谢您加入我们!




Add comment