美国医学院讲师清晰讲解随着年龄的增长睡眠的四个阶段的变化;睡眠效率的定义及其与年龄变化的关系;深度睡眠与REM睡眠的减少对健康的影响;失眠类型;导致失眠的疾病与非疾病因素等。
Insomnia_ Normal Sleep, Age, Definitions, & Types of Insomnia
本文由‘中国推动’学者,中山大学南方学院梁芷晴同学和天津医科大学RamktZ翻译编辑。
Welcome to another MedCram lecture! In the next set of lectures, we’re going to talk about insomnia, what causes it, what are the different diseases that can cause it, and how to manage it. I would say that even though I am a sleep specialist, some of the recommendations I’m going to be giving are not for everybody. So you need to make sure that you follow up with your own physician, but let’s go through insomnia.
欢迎再次参加MedCram讲座!在下一组讲座中,我们将讨论失眠,引起失眠的原因,导致失眠的各种疾病以及如何治疗的失眠。我想说的是,即使我是睡眠专家,我要提出的一些建议也不适合所有人。因此,您需要确保与自己的医生进行跟进,但让我们讨论下失眠。
The first thing we got to do is talk about what happens with normal aging. There are different stages of sleep. There is stage 1, what we term N1, stage 2 and stage 3, a couple of other stages as well. There is REM sleep, which I’m sure you’ve heard about.
我们要做的第一件事是谈论正常衰老会发生什么。睡眠有不同的阶段。有第1阶段(我们称为N1,第2阶段和第3阶段),以及另外两个阶段。有REM睡眠,我相信您已经听说过。
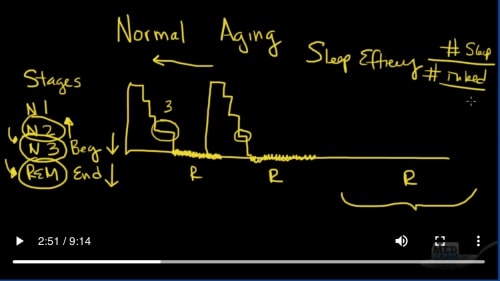
Generally speaking, what happens over the period of a night is someone starts out awake, go down into very transient sleep phase called stage 1, and then they go down to stage 2, and eventually go down into Stage 3 where they stay until they go into REM sleep, which I’ll code here as very dark. Then they come out of that and they go right back up to the beginning of stage 1, and they repeat the same thing again.
一般来说,在一夜之间发生的事情是某人开始醒着,进入非常短暂的睡眠阶段,称为阶段1,然后他们进入阶段2,最后进入阶段3,直到他们离开进入REM睡眠,我在这里将其编码为非常暗。然后他们从那出来,然后一直回到阶段1的开始,然后再次重复同样的事情。
Now as this occurs throughout the night, this REM sleep gets longer and longer until actually most of the REM sleep is towards the end of the night. These deep stages of sleep, stage 3, are usually longer towards the beginning of sleep. So something that we see here in normal sleep is that stage 3 is concentrated toward the beginning of the night, and REM sleep is concentrated more towards the end of the night.
现在,随着这种情况在整个晚上的发生,这种REM睡眠变得越来越长,直到实际上大多数REM睡眠快到一夜了。这些深度睡眠阶段(第3阶段)通常在开始睡眠之前会更长。因此,我们在正常睡眠中看到的是阶段3集中在深夜,而REM睡眠更多集中在深夜。
Both of these are very restful. Stage 3 sleep is physically restful; stage 3 sleep was where growth hormone is produced. REM sleep is very mentally restorative, so both of these are very very important. Unfortunately, as we get older, we see a reduction in both of these types of sleep, an increase in this very sort of bland and two types of sleep which really is more of a light sleep. So this is what we see within normal aging.
这两个都能帮助我们获得很好的休息。第三阶段睡眠使身体获得休息;第三阶段睡眠是产生生长激素的地方。 REM睡眠在精神上非常具有恢复作用,因此这两者都非常重要。不幸的是,随着年龄的增长,我们发现这两种类型的睡眠都有所减少,这种平淡无奇的睡眠增加了,而两种类型的睡眠实际上是一种轻度睡眠。这就是我们在正常老化过程中看到的。
Most of these changes occur by the age of 40 or 50 years of age, and sleep remains pretty constant from the age of 60 to 90. There is one exception and that is sleep efficiency. So what is sleep efficiency? Sleep efficiency is simply the amount of time of sleep divided by the amount of time in bed, and that steadily decreases from about 95% down to about 80% in general as one approaches 80 years of age.
这些变化大多数在40或50岁时发生,并且从60到90岁时睡眠保持相当稳定。有一个例外,那就是睡眠效率。那么什么是睡眠效率?睡眠效率只是睡眠时间除以床上时间,而随着人们接近80岁,睡眠效率通常从大约95%下降到大约80%。
So what happens when you approach middle-age? There’s a number of things that occur normally. There is increased awakenings. So you’re waking up more in the middle of the night. There are arousals. And there are more stages shifts. These are the stages I was talking about before. You also see a decrease in stage 3 sleep, and you’ll also see a decrease in REM sleep; as I mentioned before you get a decrease in sleep efficiency.
那么,当您接近中年时会发生什么?通常有很多事情发生。觉醒增加。因此,您在深夜醒来更多。有唤醒感。而且还有更多的阶段转移。这些是我之前谈论的阶段。您还会看到第三阶段睡眠减少,并且REM睡眠减少。正如我之前提到的,您会降低睡眠效率。
As you reach middle age, there is more of what we call a phase advancement. What do I mean by phase advancement? With phase advancement, you’re going to be getting up earlier, which means you are getting up from bed earlier and going to bed earlier. The interesting thing, however, is that despite all of these things, you are a little bit more resistant to sleep deprivation or to the effects of sleep deprivation.
当您达到中年时,我们称其为阶段性进步。阶段推进是什么意思?随着阶段的发展,您将早起,这意味着您要早起床,早起床。然而,有趣的是,尽管有所有这些事情,您对睡眠剥夺或睡眠剥夺的影响更有抵抗力。
What I mean by this is that let’s say as a teenager, if you missed four or five hours of sleep, it wouldn’t affect you as much as if you were older and you missed four or five hours of sleep. You’ll be able to perform a little better, which is kind of paradoxical from what you would think.
我的意思是说,作为一个少年,如果您错过了四五个小时的睡眠,那对您的影响不会像您成年后而错过了四五个小时的睡眠一样。您将能够表现得更好,这与您的想法有点矛盾。
Now, in terms of disease and actual disease, insomnia goes up as we get older. No surprise there if we look at a study of 18 to 34 year-olds. Now, there’s about 14 percent incidence of insomnia from the age of 35 to 49. The incidence is about 15%, so it remains pretty stable.
现在,就疾病和实际疾病而言,失眠随着年龄的增长而上升。如果我们对18至34岁的孩子进行研究,也就不足为奇了。现在,从35岁到49岁,失眠的发生率约为14%。发生率约为15%,因此保持相当稳定。
However, when we get to 50 to 64 years of age, we hit about 20% incidents; here’s the key though. From sixty-five to seventy-nine years of age, that jumps up to 25%. This is a pretty astounding figure when you realize that a quarter of the population of retirement age has a problem with insomnia. And insomnia is a pretty generic term. I mean if we could use a number of different words to describe it.
但是,当我们达到50至64岁时,发生了约20%的比例;这是关键。从65岁到79岁,这一比例上升到25%。当您意识到退休年龄的四分之一患有失眠问题时,这是一个非常惊人的数字。失眠是一个非常普通的名词。我的意思是,如果我们可以用许多不同的词来描述它。
Some about 19 percent of people wake up too early. Another nineteen percent would describe trouble falling asleep? 25% have daytime napping. Twenty-nine percent basically come right out and just say they’ve got insomnia.
大约19%的人起床太早。另有19%的人会描述入睡困难? 25%的人白天睡觉。基本上有29%的人说他们失眠了。
And then if you look at both initiating and maintaining sleep, we’re looking at 43 percent of older adults. So these are people who have a mean age of 74 years of age. Of those people, these are what they’re complaining about; and 43% have problems with initiating and maintaining both.
然后,如果您同时考虑启动和维持睡眠,那么我们所看到的是43%的老年人。因此,这些人的平均年龄为74岁。在这些人中,这些是他们所抱怨的。和43%的人在启动和维护方面都有问题。
Now, this is by no means a geriatric diagnosis. There are many young people and middle-aged people who have this problem now in terms of the different causes of insomnia. Let’s say we got rid of all of the easy causes of insomnia, for instance, drinking too much caffeine or some of these things. If we were to break it down, what would be the breakdown of insomnia in terms of causes? Well, it turns out the biggest reason for people to have insomnia, so 35 percent of people who have insomnia have some sort of psychiatric illness, and what I mean by that is depression.
现在,这绝不是老年诊断。就失眠的不同原因而言,现在有许多年轻人和中年人有这个问题。假设我们摆脱了失眠的所有容易原因,例如,喝了太多的咖啡因或其中的一些东西。如果我们将其分解,失眠的成因将是什么?好吧,原来这是人们失眠的最大原因:35%的失眠症患者患有某种精神疾病,我的意思是抑郁。
So you got to know that in terms of treatment: because if you don’t treat the depression, the insomnia is not going to get better. Next on the list, about 15% have what we call psychophysiological or what we call performance anxiety.
因此,您必须在治疗方面知道这一点:因为如果您不治疗抑郁症,失眠症将不会好转。在名单上的下一位,约有15%的人患有我们所谓的心理生理学或所谓的表现焦虑症。
What do I mean by that? Have you ever been in the kitchen, or in the living room, or the family room felt really tired? And then as soon as you went into the bedroom, you just could not fall asleep. This is psychophysiological. We’re going to explain about that in the upcoming lectures.
那是什么意思?您曾经去过厨房,客厅或家庭室感到非常疲倦吗?然后,一旦进入卧室,您就无法入睡。这是心理生理的。我们将在接下来的讲座中对此进行解释。
12% is alcohol or drug. Yes, these can cause insomnia. Another 12% is Restless Leg Syndrome – something that we’ll talk about, as well 10% is circadian rhythm disorder, and finally, the last nine percent is kind of a weird diagnosis. It’s actually where they think they can’t sleep, but they actually are sleeping if you test them. It’s called paradoxical.
12%是酒精或毒品。是的,这些会导致失眠。剩下的12%是躁动性腿综合症-我们将要讨论的话题,还有10%是昼夜节律紊乱,最后,最后9%是一种奇怪的诊断。实际上,他们认为他们无法入睡,但是如果您对其进行测试,他们实际上正在入睡。这被称为悖论。
So you can see here that this is where the bulk of your diagnosis is. This one’s going to be the most interesting. So what we’re going to do is we’ve kind of laid the groundwork of what insomnia is, where it comes from. Let’s talk about where the path of physiology meets the road in terms of causes, diagnosis, management, and treatment. Join us for the next lecture!
因此,您可以在这里看到大部分诊断内容。这将是最有趣的。因此,我们要做的是为失眠的根源,根源奠定基础。让我们从成因,诊断,管理和治疗方面谈谈生理学路径与道路相交的地方。加入我们的下一个讲座!


Add comment