美国睡眠专家讲解导致失眠的十大非疾病因素、良好的睡眠习惯、失眠因素管理等。如这些办法还不能解决失眠问题,则考虑对失眠患者采取行为治疗或药物治疗。药物治疗为最后选项。
Insomnia_ CBTI, Stimulus Control, Sleep Hygiene (Lecture 3)
本文由 ‘中国推动’ 学者、吉林大学医学院毛宗韬同学编辑整理
Welcome to another MeCram lecture! What we were talking about before was the general approach to somebody with insomnia, and the general approach was to look for diseases that could cause it. If that didn’t elucidate exactly what the cause was, then look for other things.
欢迎参加另一个MeCram讲座!我们之前谈论的是失眠症患者的一般治疗方法,而一般方法是寻找可能引起失眠的疾病。如果那不能完全阐明原因,则寻找其他东西。
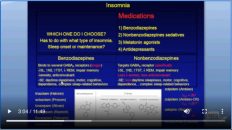
Specifically, sleep hygiene, stimulus control, which we’re now going to talk about, and then move on to behavioral therapy and medications. We said in the last lecture that medications are actually a lot lower down on the list than what I might think. So in this section, let’s talk about what sleep hygiene and stimulus control are. Here, I’ve got listed the category of sleep hygiene and stimulus control, specifically, the different components of sleep hygiene and stimulus control. They are actually different. So, let’s take this one step at a time.
具体来说,我们现在要讨论的是睡眠卫生,刺激控制,然后转向行为疗法和药物治疗。我们在上一讲中说过,药物实际上比我想的要低得多。因此,在本节中,我们将讨论什么是睡眠卫生和刺激控制。在这里,我列出了睡眠卫生和刺激控制的类别,特别是睡眠卫生和刺激控制的不同组成部分。它们实际上是不同的。因此,让我们一次迈出这一步。
First of all, sleep hygiene specifically is making sure that you are performing and doing the right things when you go to bed, which ensures that we don’t perpetuate some bad habits that could keep you up at night.
首先,睡眠卫生特别是要确保您上床睡觉时表现良好,做正确的事,这可以确保我们不会养成使您彻夜难眠的不良习惯。
So the first thing is to sleep until rested and then get up. The key here is to get up. We do not want you to stay in bed after you’ve woken up. Some people wake up early and they stay in bed for another hour, which is not a good thing because what we’re doing is we’re associating the bedroom with being awake. We want you to associate sleeping with the bedroom. So sleep until rested and then get up. Get out of bed and do your activity.
因此,第一件事就是睡觉直到休息,然后起床。这里的关键是起床。我们不希望您醒后躺在床上。有些人会早起,然后再躺在床上一个小时,这不是一件好事,因为我们正在做的是将卧室与清醒联系起来。我们希望您将睡眠与卧室联系起来。所以睡觉直到休息然后起床。起床做您的活动。
You also want to keep a regular sleep schedule, which is to make sure that your circadian rhythm is in tune. It’s gonna be much easier if when it’s time to go to bed you are actually going to bed. So keeping a regular sleep schedule would be important. This can be broken with people who do, for instance, graveyard shifts or nocturnal shifts. So that can be a problem.
您还希望保持定期的睡眠时间表,以确保您的昼夜节律保持一致。如果您上床睡觉的时间到了,那会容易得多。因此,保持规律的睡眠时间表很重要。有些人,比如上夜班的人,这样做会很苦难。
Number three: do not force sleep. There’s nothing worse than trying to go to sleep when your body doesn’t want to go to sleep. When your body doesn’t go to sleep, you become anxious; then you associate anxiety with the bedroom, and you get performance anxiety. Remember we called that psychophysiological insomnia. We don’t want that.
第三:不要强迫睡眠。当您的身体不想入睡时,没有比尝试入睡更糟糕的了。当您的身体无法入睡时,您会感到焦虑。然后将焦虑与卧室联系起来,就会出现’表现焦虑’。记住,我们称其为心理生理失眠症。我们不想要那个。
Next: exercise regularly, but make sure you don’t do it right before you go to bed. Make sure it’s at least four to five hours before you go to bed because while exercise is good, it can also limit your ability to go to sleep right afterwards.
下一步:定期运动,但要确保上床睡觉之前不要做运动。确保至少在睡前四到五个小时,因为虽然运动很好,但它也可能限制您之后立即入睡的能力。
Number five is pretty obvious: avoiding caffeinated drinks in the afternoon or evening. This is going to ramp you up and it’s going to make it more difficult for you to go to bed.
第五点很明显:在下午或晚上避免喝含咖啡因的饮料。这将使您起床,并使您上床更加困难。
In a similar token, avoiding alcohol at bedtime. Now this may seem counterintuitive, because alcohol is a central nervous system depressant. However, you have to realize it may help someone go to sleep initially, but because it is so short acting, you’re going to get a rebound awakening maybe two, three, four hours later. So, you might find it in the middle of the night waking up because of alcohol.
同样,就寝时避免饮酒。现在,这似乎违反直觉,因为酒精是中枢神经系统抑制剂。但是,您必须意识到它可能会帮助某人最初入睡,但是由于动作太短,您可能会在两个,三个,四个小时后得到反弹的唤醒。因此,您可能会在半夜由于酒精而醒来。
You want to avoid smoking in the p.m. I would say avoid smoking altogether. This is for many different reasons, of course, but smoking causes edema of the airway and can exacerbate obstructive sleep apnea among other things.
您要避免在下午吸烟。我要说完全避免吸烟。当然,这有许多不同的原因,但是吸烟会引起呼吸道水肿,并可能加剧阻塞性睡眠呼吸暂停。
Don’t go to bed hungry. We want to be satisfied when we go to bed. It’s much easier to fall asleep.
不要饿着肚子睡觉。 我们在睡觉时感到满足,入睡要容易得多。
You want to adjust your bedroom environment. So make sure the room is a little bit cooler. Make sure that there is no light coming in. Make sure that you are soundproofed. Just take care of the obvious things that would prevent you from going to sleep. If you sleep with a dog or baby, these things may kick you and maybe wake you up without your even knowing it.
调整您的卧室环境。因此,请确保房间有点凉。确保没有光进入。确保您是隔音的。只需照顾一些会阻止您入睡的明显事情。如果您与狗或婴儿一起睡觉,TA们可能会踢您,甚至可能在您不知道的情况下将您叫醒。
So just be sure that is taken care of, and then deal with your worries before bedtime. I would advise avoiding television or the news, especially the bad news. If you’ve got worries on your mind, you may want to write those things down on a pad and put it on your bedside, and say I’m going to deal with those things in the morning.
因此,请确保已妥善处理,然后在就寝之前解决您的后顾之忧。我建议避免电视或新闻,尤其是坏消息。如果您有烦恼,可以将这些东西写在垫子上,放在床边,然后说我要在早晨处理这些东西。
Sleep hygiene is one of the first things that we do in somebody who just can’t sleep. And it’s to make sure that we’re avoiding some of these perpetuating factors that could prevent them from going back to a regular sleep schedule.
好的,所以睡眠卫生是我们对失眠者要做的第一件事。 这是要确保我们避免了一些可能阻止他们回到正常的睡眠的永久性因素。
Stimulus control is a little bit different. Stimulus control has to do with classical conditioning. You remember Pavlov’s dogs? Pavlov’s dogs were these creatures that Pavlov, the scientist, kept. He noticed that before feeding them, if you rang a bell, eventually got to the point where all he had to do was ring the bell, and they would salivate instead of when he put the food in front of them, they would start to salivate. And the reason is that the brain of the dogs associated the bell with dinner time.
刺激控制有些不同。刺激控制与经典条件有关。您还记得巴甫洛夫的狗吗?巴甫洛夫的狗就是科学家巴甫洛夫饲养的生物。他注意到,在给他们喂食之前,如果您按了一下门铃,最终到了他只需要按门铃的地步,他们就会垂涎三尺,而不是他将食物放在他们面前时垂涎三尺 。原因是狗的大脑将钟声与晚餐时间联系在一起。
In this situation with sleep, we want to associate correct things with the bedroom. We don’t want to associate non–sleep activity with the bedroom. Because if we do that, it’s going to dilute that stimulus control to cause us to go to sleep. So just like on sleep hygiene, we said sleep until rested and then get up. Congruently, we want to only go to bed when sleepy. So, if we go to bed when we’re not sleepy, we’re not going to sleep. Then we associate not being able to go to sleep, the anxiety associated with that, with the bedroom. So what I’m saying here is that, if you go to the bedroom and you can’t sleep, then get out of bed and go to another room in the house.
在这种睡眠状态下,我们希望将正确的事物与卧室联系起来。我们不想将非睡眠活动与卧室相关联。因为如果这样做,将会稀释刺激控制,导致我们入睡。因此,就像保持睡眠卫生一样,我们说睡觉直到休息,然后再起床。恰好,我们只想在困倦时上床睡觉。因此,如果我们在不困的时候上床睡觉,就不会睡觉。然后,我们将无法入睡,与之相关的焦虑与卧室联系起来。因此,我在这里要说的是,如果您去卧室而无法入睡,那么就起床去房子里的另一个房间。
The other one is to use the bedroom for sleep and sex only. No television, no reading, no eating, no other activity in the bedroom. We don’t want to dilute the stimulus of the bedroom. Number three: get out of bed if not able to sleep in 20 minutes. This goes along with number one. So you would only return to the bed when you were sleepy and you need to repeat this as many times as necessary throughout the night. This is to ensure that your only associating sleep with the bedroom.
另一种是仅将卧室用于睡眠和做爱。没有电视,没有读书,没有饮食,在卧室没有其他活动。我们不想淡化卧室的刺激。第三:如果20分钟内无法入睡,请起床。这与第一。因此,只有在困倦时才回到床上,并且需要整夜重复多次。这是为了确保您唯一的与卧室相关的睡眠。
Number four is wake up at the same time each day use an alarm clock if necessary. Again, this is kind of congruent with keeping a regular sleep schedule. Finally, no napping. Napping in the afternoon is going to rejuvenate you, and it’s going to reduce your homeostatic drive to sleep when you get to nighttime.
第四天每天在同一时间醒来,如有必要,请使用闹钟。同样,这与保持规律的睡眠时间表是一致的。最后,没有小睡。午睡将使您恢复活力,并减少夜间睡觉时体内稳态的睡眠。
So again, this is sleep hygiene stimulus control. These are the sort of things that we do for an insomnia patient on the initial intake after we’ve ruled out some obvious diseases that could cause the insomnia. Again, if you look at our approach for insomnia. The general approaches, we’re going to look for diseases. We’re going to do hygiene and stimulus.
这是睡眠卫生刺激控制。这些都是我们在排除了一些明显的可能导致失眠的疾病后为失眠症患者做的初步治疗。 再次说明,如果您考虑我们的失眠方法。 一般的方法,我们将寻找疾病。 我们将要进行卫生和刺激。
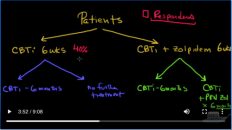
If that doesn’t work and your patient still has insomnia, then we would move on to the next step with just behavioral therapy and medication. Join us for the next lecture where we talked about behavioral therapy. Thanks for joining us.
如果这些都不起作用,您的病人仍然失眠,那么我们就可以进行下一步的行为疗法和药物治疗。下一节课我们会讲到行为疗法。感谢收看我们的节目。



Add comment