美国睡眠专家阐述三个失眠理论,即三种因素(predisposing factors, or premorbid factors, precipitating factors, and perpetuated factors);急性失眠成因;perpetuated factors因素对其它失眠因素造成的叠加影响等。
Insomnia 3P_ Theory and Approach to Insomnia (Lecture 2)
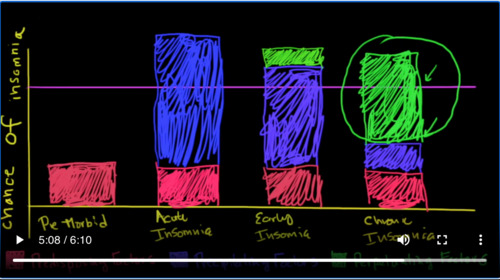
Here is another MedCram lecture. We’re going to continue with our talk on insomnia. So here I’ve got, a graph that’s going to describe what the theory is in terms of insomnia, and how people get insomnia. This is a little bit of a graph here to explain over a number of months to years how this could happen.
这是另一个MedCram讲座。我们将继续讨论失眠。所以在这里,我得到了一张图表,它将描述失眠症的理论以及人们如何失眠。这是一张图表,用于解释数月到数年的时间如何发生。
So we’ve got in red here: predisposing factors. So what are predisposing factors? This is just the way you are made. It’s your genetics. It’s your tendency to have anxiety. It’s something that’s pre-wired. You can’t do anything about it. It’s just there.
因此,这里有红色:先天因素。那么什么是先天因素呢?这就是您的制作方式。这是你的遗传。你有焦虑的倾向。这是预先接线的。你对此无能为力。就在那儿。
Next one is the blue, which is the precipitating factor. You can’t control this either; something just happens in your life, either good stress or bad stress, you’re moving away to college, you’re getting married, you’re getting divorced, someone that’s born in the family disowned, or died in the family. So these are major life events. These are the precipitating factors.
下一个是蓝色,这是突然因素。您也无法控制;生活中只会发生一些事情,无论是好压力还是好压力,您正要去上大学,要结婚,要离婚,在家庭中出生的人去世或在家庭中死亡。因此,这些都是重大的生活事件。这些是诱发因素。
Finally, these are perpetuating factors, which I will talk about. These are the things that we do to ourselves that are harmful in terms of our sleep hygiene, and keep us from having a good night’s sleep. So let’s talk about this a little bit here.
最后,这些是永久性因素,我将在后面讨论。这些是我们对自己做的事情,对我们的睡眠卫生有害,使我们无法睡个好觉。因此,让我们在这里稍作讨论。
The first graph that I want to talk about is called the pre-morbid condition. What do I mean by this? If you can remember back to your childhood, this is how you were, you could sleep. Some people had problems sleeping their whole lives. But let’s just assume here that you are fine. Here is the premorbid condition, and this is just your genetics, this is just how you are; there’s nothing you can do about it. This is the contribution of your genetics, otherwise known as predisposing factors, that are going to cause you to have problems.
我要谈的第一个图称为病前状态。我是什么意思如果您能记得自己的童年时代,这就是您的样子,那么您就可以入睡。有些人一辈子都睡不着。但是,让我们在这里假设您还好。这是病前病,这只是你的遗传,这就是你的状态;您无能为力。这是您的遗传学(也称为诱发因素)的贡献,这些都会导致您遇到问题。
Now you can see here. This is the summation of all the problems, and it’s well short of the threshold that’s going to cause insomnia. The spline is the insomnia threshold. So since you’re below the insomnia threshold, you don’t have insomnia now.
现在您可以在这里看到。这是所有问题的总和,远远低于会引起失眠的阈值。样条曲线是失眠的阈值。因此,由于您处于失眠阈值以下,因此您现在没有失眠。
Let’s move on to the next phase in your life, and the next phase in your life is acute insomnia. Again, you cannot change, so you have your basic set of inherent factors that are part of you, that either do or don’t make you have a tendency to insomnia. But instead of just that, now you have major life stressors, and that major life stressors have a high enough magnitude that actually goes over the insomnia threshold. As a result of this, you have insomnia.
让我们进入人生的下一个阶段,人生的下一个阶段是严重的失眠。再说一次,你不能改变,所以你拥有一些基本的内在因素,这些内在因素使你容易失眠。但是,不仅如此,现在您还拥有主要的生活压力源,而主要的生活压力源具有足够高的强度,可以超过失眠的阈值。结果,您失眠。
Okay. This is normal people have this all the time. They’ve got to test the next day. They have a major report that they have to do. They’ve got to go on a trip. This is all part of life. Sometimes it’s difficult to sleep in those situations; you can’t prevent that okay, but something happens.
好的。这是正常人一直都有的。他们必须第二天进行测试。他们有一份必须要做的重要报告。他们必须去旅行。这就是生活的一部分。在某些情况下,有时候很难入睡。您无法阻止这种情况,但是发生了一些事情.
Some people are well adapted. When this insomnia acute factor goes away, they go right back to normal and they have good sleep. However, in some people, early insomnia, something else that happens. Here again, are our predisposing factors. As the stress, it is still over the threshold, but as the stress from that insomnia starts to recede, we unwittingly begin to add these perpetuating factors. We’ll talk about what those perpetuating factors are very shortly.
有些人适应能力强。当失眠的急性因素消失后,他们就会恢复正常,并且睡眠良好。但是,在某些人中,早期失眠会发生其他事情。同样,这是我们的诱因。随着压力的增加,压力仍然超过阈值,但是随着失眠的压力开始减轻,我们无意中开始添加这些永久性因素。我们将在短期内讨论这些永续因素。
But nonetheless, we add perpetuating factors until finally, we get to the situation of chronic insomnia. Now again, we have the thing that we cannot change, which is our predisposing factors, and the actual acute event may be very minimal. In fact, by itself, it would be well below the insomnia threshold, but because we have these perpetuating factors, and because we have unwittingly engaged in behaviors, we continue in a situation where we are still over the insomnia threshold.
但是,尽管如此,我们增加了持久性因素,直到最后,我们才进入了慢性失眠的境地。再说一次,我们有无法改变的东西,这是我们的诱因,实际的急性事件可能很小。实际上,它本身将远远低于失眠阈值,但是由于我们具有这些永存的因素,并且由于我们无意中参与了行为,因此我们继续处于失眠阈值以上的情况。
If we could somehow figure out what we’re doing here and correct that, we could be down here enjoying a good night’s sleep. So the rest of these lectures are dedicated to figuring out what that stuff is and how to do something about it.
如果我们能以某种方式弄清楚我们在这里所做的事情并纠正它,我们可能会在这里睡个好觉。因此,这些讲座的其余部分都致力于弄清这些东西是什么以及如何对其进行处理。
Now notice, I haven’t talked about sleep medication. We’re going to talk about what the societies that deal with insomnia recommend. Let’s talk about that very briefly before we end this video and go on to the next for insomnia.
现在注意,我还没有谈论安眠药。我们将讨论有关失眠的社会的建议。在结束本视频并继续进行下一个失眠之前,让我们简短地讨论一下。
The general approach that I use in the office. First, it is to look for diseases that could cause the patient to have insomnia; things like obstructive sleep apnea. Look at our videos on obstructive sleep apnea to get a better understanding about that. We look at sleep hygiene.
我在办公室使用的一般方法。首先,要寻找可能导致患者失眠的疾病。阻塞性睡眠呼吸暂停之类的事情。观看我们有关阻塞性睡眠呼吸暂停的视频,以更好地了解这一点。我们看睡眠卫生。
So we review a list that will talk about when we talk about stimulus control. This is very interesting, and we’ll talk specifically about stimulus control in the next couple of lectures. It’s only then after we’ve done that, that we still haven’t made headway that we start looking at behavioral therapy, and then finally medication. Notice how far down the list medication is for insomnia, and yet if you look at television and commercials, you’ll think that the first thing you should do if you can’t sleep is to take a sleeping pill. let’s talk about that and we’ll move on to the next lecture. See you next time.
因此,我们审查了一份清单,该清单将在讨论刺激控制时讨论。这是非常有趣的,我们将在接下来的两个讲座中专门讨论刺激控制。只是在这样做之后,我们仍然没有取得进展,我们开始研究行为疗法,然后才是药物。请注意,失眠治疗药物的种类有多低,但是如果您看电视和商业广告,您会认为如果无法入睡,您应该做的第一件事就是服用安眠药。让我们讨论一下,我们将继续下一个演讲。下次见。


Add comment