Welcome to another MedCram COVID-19 update. As we look at our Johns Hopkins coronavirus tracker, we can see where the infections are in the world. Recently they’ve updated this to actually show a little bit more in terms of location. So you can actually look and zoom in as you can see that the number of cases is starting to rise quite precipitously.
欢迎来到MedCram COVID-19的另一个更新。当我们查看Johns Hopkins冠状病毒追踪器时,我们可以看到世界上感染的地方。最近,他们对其进行了更新,以实际显示更多的位置信息。因此,您实际上可以进行查看和放大,因为您可以看到案例数量开始急剧增长。
I want to highlight this free app called the COVID-19 Tracker that was developed by a retired OBGYN physician in Florida and his team of developers at a company called Healthlinked. To look for additional trends and clusters of cases, they’ve created a platform for users to report if they have COVID-19-like symptoms and if they’ve been tested for it. As you can see this app has already become one of the most popular medical apps. As testing availability and challenges continue in the United States and other countries, apps like this could be a helpful tracking tool for hospitals and communities.
我想强调一下这个免费的应用程序,称为COVID-19 Tracker,该应用程序由佛罗里达州的一位退休的OBGYN医生及其在名为Health Linked的公司的开发人员团队开发。为了寻找其他趋势和病例群集,他们创建了一个平台供用户报告是否有类似COVID-19的症状以及是否已经接受过测试。如您所见,此应用程序已成为最受欢迎的医疗应用程序之一。随着测试可用性和挑战在美国和其他国家/地区持续存在,类似这样的应用程序可能成为医院和社区有用的跟踪工具。
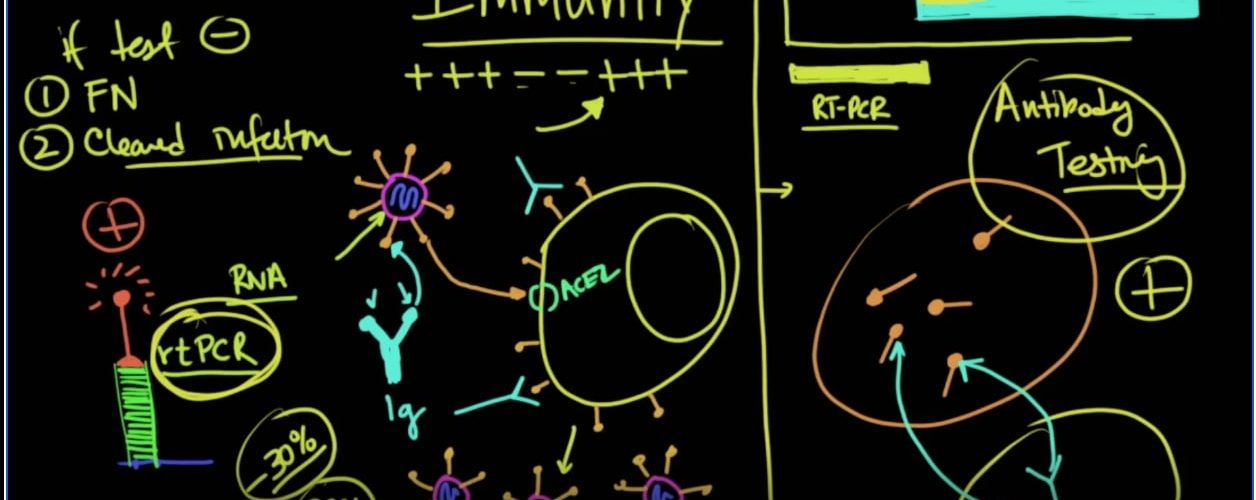
It’s finally time to talk about immunity. This is a complicated topic, so we are going to go through it fairly slowly but at a rapid pace as you’ll see. You’ve got a cell. In this case, the cell has the ACE2 enzyme, which is the receptor for the virus. Here comes the virus, and on the virus are spike proteins, and it is these spike proteins that allow it to bind and come into the cell.
现在是时候谈谈免疫力了。这是一个复杂的主题,因此您将看到,我们将以非常缓慢的速度进行研究。你有一个牢房。在这种情况下,细胞具有ACE2酶,它是病毒的受体。病毒来了,病毒上有刺突蛋白,正是这些刺突蛋白使它结合并进入细胞。
But inside this virion is an RNA molecule, and it’s this RNA molecule that gives instructions to the cell to make more viral particles. So what you get as a result of that are more viral particles.
但是在这个病毒体内部是一个RNA分子,正是这个RNA分子向细胞发出指令以制造更多的病毒颗粒。因此,您得到的是更多的病毒颗粒。
Of course, each of those viral particles have their own RNA, which is copied from the original. But remember when that virus particle fuses with the cell, that membrane fuses with this membrane. Then the cell shows that it’s infected because it has those particles on the surface as well. So the general way that we’ve been testing for the virus is by looking at specifically the RNA, and that’s the testing that’s been done up to this point.
当然,每个病毒颗粒都有自己的RNA,该RNA是从原始病毒复制而来的。但是请记住,当病毒颗粒与细胞融合时,该膜与该膜融合。然后该细胞表明它已被感染,因为它的表面也有这些颗粒。因此,我们一直在测试该病毒的一般方法是专门查看RNA,这是到目前为止已完成的测试。
The technique that is used is called reverse transcriptase polymerase chain reaction or RTPCR. It takes a little fragment of that RNA, and it finds a specific sequence that’s unique to that sequence, and it copies it and then it takes that and it copies it, so it can amplify from RNA a bunch of DNA which looks just like it.
所使用的技术称为逆转录酶聚合酶链反应或RTPCR。它提取该RNA的一个小片段,找到一个对该序列唯一的特定序列,然后将其复制,然后将其复制并复制,因此可以从RNA中扩增出看起来像它的一堆DNA。
Because we have a certain code in that DNA that’s unique to that and therefore is unique to this RNA, we can put onto it a nice thing that lights up that will bind called a probe. If we see that this thing lights up, huh, we have a positive test. If on the other hand, we don’t see that, then the reverse transcriptase won’t recognize the specific sequence of that RNA, which is specific to this virus and no other, it won’t amplify it and we will get a negative result. This is how we test whether or not somebody is positive for COVID-19 or negative for COVID-19.
因为我们在DNA中具有特定的代码,因此该DNA是唯一的,因此对于该RNA是唯一的,因此我们可以在其上放上一个发光的好东西,它将结合在一起,称为探针。如果我们看到这件事点亮了,嗯,我们得到了积极的检验。另一方面,如果我们看不到,则逆转录酶将无法识别该RNA的特定序列,该序列对这种病毒是特异性的,而对其他病毒则没有特异性,它不会扩增它,我们将得到阴性结果。结果。这是我们测试有人对COVID-19阳性还是对COVID-19阴性的方法。
Unfortunately, based on the statistics that I have seen, notwithstanding some of the reports from South Korea versus their testing, I have seen anywhere from a 60 to 70 percent sensitivity, and some of you may see different numbers. Sensitivity tells you what percent likely that if somebody is negative, then you can rule it out. Though if someone test negative for coronavirus or negative for COVID-19, then there is, in this case, a 30% chance that they could still potentially have the disease. When you’re talking about isolating somebody, what you really want to have for sensitivity is something as close as possible to 99 or a 100% sensitivity.
不幸的是,根据我所看到的统计数据,尽管有一些来自韩国的报告与他们的测试,但我看到的灵敏度在60%到70%之间,有些人可能会看到不同的数字。敏感度告诉您,如果某人为负面,那么您可以排除百分之几。尽管如果某人的冠状病毒检测结果为阴性或COVID-19检测结果为阴性,那么在这种情况下,他们仍有30%的可能性仍可能患有该疾病。当您谈论隔离某个人时,您真正希望获得的灵敏度是尽可能接近99或100%的灵敏度。
So that’s been an issue with regard to this type of testing. Obviously this is the kind of testing that you want to do in the acute situation. If someone is infected with this coronavirus, and they have a bunch of these viral particles floating around, it’s going to be easy to detect whether or not they are positive. If the person has recovered, and there is no more RNA, then their test is going to be negative. If their test is negative, and here’s the key point: if the test is negative, there are two possibilities: number one, it could be a false negative or number two, they could have cleared the infection.
因此,对于这种类型的测试,这一直是一个问题。显然,这是您要在紧急情况下进行的测试。如果有人感染了这种冠状病毒,并且他们周围有一堆病毒颗粒,那么将很容易检测它们是否为阳性。如果此人已经康复,并且不再有RNA,那么他们的检测将为阴性。如果他们的测试是否定的,那就是关键所在:如果测试是否定的,那么有两种可能性:第一,可能是假阴性,第二,他们可能已经清除了感染。
Here comes the issue with regards to reinfection, and that’s been the real key question up to this point. If you do serial testing on somebody, and you get something that looks like this positive, positive, positive, negative, negative, positive, positive, positive. Let’s say you tested them eight times in this situation. What is the reason why this is positive, is it because these were false negatives or is it because they truly were negative and then they got reinfected again? You don’t really know especially when you have a sensitivity that is less than a 100%.
再感染问题到此为止,这一直是真正的关键问题。如果您对某人进行了串行测试,那么您得到的结果看起来像是阳性,阳性,阳性,阴性,阴性,阳性,阳性,阳性。假设您在这种情况下测试了八次。这是阳性的原因是什么,是因为这些是假阴性,还是因为它们是真正的阴性然后又被再次感染?当您的灵敏度小于100%时,您并不是很清楚。
Now generally speaking, when you do actually get immunity to the virus, what occurs at that point is antibodies are made to the virus, and specifically it’s going to be these proteins that are on the surface that are going to be the easiest to make antibodies. Antibody typically looks like this, it’s got a nice constant protein, and here are the variable ends, here with these being hypervariable where you can actually have different protein confirmations that will fit perfectly into this type of a spike protein.
现在一般来说,当您确实对病毒具有免疫力时,此时会产生针对该病毒的抗体,特别是表面上的这些蛋白质将最容易制造抗体。抗体通常看起来像这样,它有一个很好的恒定蛋白质,这是可变末端,这里这些都是高变的,在那里您实际上可以拥有不同的蛋白质确认,这些确认将完全适合这种尖峰蛋白质。
So when you make these kinds of antibodies, the antibodies will signal out these types of cells and mark them for destruction by other parts of the immune system. In terms of a timeline, starting from zero here, generally speaking, what you would see the positive results at this point when you have the illness until finally you recover and the virus is no longer detectable, and that would be the reverse transcriptase PCR test, that’s this test over here. Then at some point, you’re going to develop an antibody response which is then going to be picked up. So these antibodies hopefully will give you immunity to this virus for the rest of your life. This is why you get vaccinations for measles, mumps, rubella, etc.
因此,当您制作这些类型的抗体时,这些抗体会发出信号通知这些类型的细胞,并标记它们被免疫系统的其他部分破坏。就时间轴而言,从零开始,通常来说,当您生病直到最终恢复并且不再检测到病毒时,此时您会看到阳性结果,这就是逆转录酶PCR检测,这就是这里的测试。然后在某个时候,您将产生抗体应答,然后将其应答。因此,这些抗体有望在您的余生中为您提供对该病毒的免疫力。这就是为什么要接种麻疹,腮腺炎,风疹等疫苗的原因。
These are called immunoglobulins, but they’re different types of immunoglobulins, there are immunoglobulins that occur early in the immune response, and that’s called an IgM. So M is the first one that you would see and then later on, you’re going to get an IgG molecule instead. If somebody were to be positive on an IgG for a specific virus, then I would say you, generally speaking, had immunity from an infection a long time ago. But if your IgM was positive then I would say, ah, this is an antibody to a viral protein that must have happened just recently, maybe in the last few weeks or even days, depending on the immune response. Generally speaking, it’s more along the lines of weeks to a month or so.
这些被称为免疫球蛋白,但是它们是不同类型的免疫球蛋白,在免疫反应的早期就有免疫球蛋白,这就是所谓的IgM。因此,M是您会看到的第一个,然后再获得IgG分子。如果有人对某种特定病毒的IgG呈阳性反应,那么我想说,一般来说,您很早以前就具有免疫力。但是,如果您的IgM呈阳性,那么我会说,嗯,这是一种病毒蛋白抗体,必须在最近才发生,可能在最近几周甚至几天,这取决于免疫反应。一般而言,通常是几周到一个月左右。
What about testing for that? Well, the way that we test for these antibodies, scientists manufacture little portions of those spike proteins, but they are manufactured, and so if they mix their reagent with the blood from the patient which may or may not have antibodies, you’re going to see here that those antibodies are going to mix, and they will have a certain thing that occurs when these things mixed together, and it will turn out to be a positive test, and they can tell based on the test which we won’t get into, whether it’s an IgM or an IgG.
那测试呢?好吧,按照我们测试这些抗体的方式,科学家只能制造出很少部分的刺突蛋白,但是它们是被制造出来的,因此,如果将它们的试剂与患者血液中可能有或没有抗体的抗体混合,那么您将在这里看到这些抗体将要混合,当它们混合在一起时,它们会发生某种确定的事情,结果将是一个阳性测试,他们可以根据测试判断出我们不会不管是IgM还是IgG。
So this type of testing here on the right side of this line here is just now starting to come on. This could be potentially important because even though you might not have symptoms of the original infection, you will be able to know whether or not you have been infected using this kind of a test, and we will bring up other applications of this later on in this video. But understand that there is a difference between PCR testing and antibody testing. Antibody testing is checking to see whether or not you have immunity against the virus whereas the reverse transcriptase PCR is looking to see whether or not you actually have viral particles still inside your body.
因此,此行右侧的这种测试刚刚开始进行。这可能很重要,因为即使您可能没有原始感染的症状,也可以使用这种测试知道您是否被感染了,稍后我们将在此提出其他应用程序。这个视频。但是请理解,PCR测试和抗体测试之间存在差异。抗体测试旨在检查您是否对该病毒具有免疫力,而逆转录聚合酶链反应(PCR)则用于查看您体内是否确实还有病毒颗粒。
So the question is in this situation, is the patient testing falsely negative because of these poor sensitivities on these reverse transcriptase PCR’s or is the patient really becoming infected again? There was a non-peer-reviewed article that recently put some of those questions to answer. This article set out trying to determine whether or not infection with the COVID-19 disease with the SARS-CoV-2 virus conferred immunity to the host for repeated infections afterwards. Now, let’s go over what they did, and I want to let you know that this does involve animal research, in this case, rhesus monkeys, which are fairly close to us in terms of genetics.
所以问题就在这种情况下,患者是否由于对这些逆转录酶PCR的敏感性差而检测为假阴性,还是患者真的再次受到感染?最近有一篇未经同行评议的文章,回答了其中一些问题。本文着手尝试确定SARS-CoV-2病毒感染COVID-19疾病是否赋予宿主免疫力,以防其后再次感染。现在,让我们回顾一下他们所做的事情,我想告诉您,这确实涉及动物研究,在这种情况下,是恒河猴,在遗传学方面与我们非常接近。
They took four rhesus monkeys, and they infected all four of them with the SARS-CoV-2 virus. All of them had similar symptoms, the symptoms and signs that you would imagine. They lost a little bit of weight, they showed signs and symptoms of the virus. Furthermore, they checked viral loads using that reverse transcriptase PCR that we talked about, and those peaked at about three days in all of the monkeys.
他们带了四只恒河猴,并用SARS-CoV-2病毒感染了全部四只。他们都有相似的症状,您会想像的症状和体征。他们减轻了一点体重,显示出病毒的体征和症状。此外,他们使用我们所说的逆转录酶PCR检查了病毒载量,并在所有猴子中大约三天达到峰值。
Of note, they check not only the nasopharyngeal swabs, but they also did anal swabs to make sure that they had checked for viral shedding in both places, and the peak was around three days after the initial infection. They sacrificed one of the animals, and after evaluating the monkey they went to go look to see exactly where the virus ended up in that body. They were able to see that the virus was in the nose, pharynx, which is the mouth, lungs, which is where most of the virus hung out, the gut, spinal cord, the heart, skeletal muscle and the bladder.
值得注意的是,他们不仅检查鼻咽拭子,而且还检查了肛门拭子,以确保检查了两个地方的病毒脱落,并且高峰期是在初次感染后三天左右。他们处死了其中一只动物,在评估了猴子之后,他们去看清楚了该病毒在该体内最终的位置。他们能够看到病毒在鼻子,咽,嘴,肺,肠道,脊髓,心脏,骨骼肌和膀胱中,那里是大多数病毒的发源地。
Then what they did in the remaining three monkeys is they measured antibodies at day 14, at day 21 and at day 28, and what they saw in those three remaining monkeys were all of the things that you would notice to see if someone had immunity, which was basically there were increasing signs of antibodies being made, showing that these monkeys were recovering from the initial infection of the SARS-CoV-2 virus.
然后,他们在剩下的三只猴子中所做的就是在第14天,第21天和第28天测量了抗体,而在剩下的三只猴子中所看到的就是您会注意到某人是否具有免疫力的所有东西,基本上已经有越来越多的抗体在生产,这表明这些猴子正在从SARS-CoV-2病毒的最初感染中恢复过来。
Of note, they looked at the chest x-rays on day 28, and the chest x-rays were negative. They were essentially normal at that point. The other thing that they did was check the viral load at that time as well using reverse transcriptase PCR, and in all of them, the viral load was all negative. So at day 28, we essentially have recovered primates without an abnormal chest x-ray and with undetectable viral load.
值得注意的是,他们在第28天观察了胸部X光,胸部X光为阴性。那时他们基本上是正常的。他们要做的另一件事是同时使用逆转录酶PCR检查病毒载量,在所有这些病毒载量中,所有病毒载量均为阴性。因此,在第28天,我们基本上已经恢复了灵长类动物,没有异常的胸部X射线和无法检测到的病毒载量。
What they did on day 28 was they reinfected the remaining three monkeys and monitored them. Other than an initial spike in temperature in all three of them, they showed none of the signs that they had back here with the weight loss and the signs and symptoms that you would expect with a viral infection. None of those signs were present other than a very small spike in body temperature which quickly went away.
他们在第28天所做的工作是重新感染了其余三只猴子,并对其进行了监视。除了他们三个人的体温最初升高外,他们都没有出现体重减轻以及病毒感染可能带来的体征和症状的迹象。除了极小的体温峰值迅速消失以外,没有任何迹象出现。
And after about five days they sacrificed one of these animals and looked to see if there was any kind of abnormality or virus anywhere, and they looked in all three of these a total of 96 times to see if there was any virus, any viral load using RT-PCR, and the answer in every single case was none.
大约五天后,他们处死了其中一只动物,看是否有异常或病毒,然后对这三只动物总共进行了96次检查,看是否有病毒,病毒载量。使用RT-PCR,在每种情况下都没有答案。
When they looked at that sacrifice monkey after five days, they showed that there was no viral replication in all tissues, as well as no pathological damage and viral antigen in lung tissues. They go on to say, ‘’therefore our results suggested that the monkeys with SARS-CoV-2 infection after recovery could not be reinfected with the same strain. Longitudinally, the monkey that had undergone single infection in this study did not appear to show signs of recurrence after the recovery, either’’.
五天后,他们看着那只祭祀的猴子,他们发现在所有组织中都没有病毒复制,在肺组织中也没有病理损伤和病毒抗原。他们继续说,“因此我们的结果表明,恢复后感染SARS-CoV-2的猴子无法用同一菌株再次感染。从纵向上看,在这项研究中经历过一次感染的猴子似乎也没有在恢复后显示出复发的迹象。
Taken together the team concludes: ‘’our results indicated that the primary SARS-CoV-2 infection could protect from subsequent exposures which have vital implications for vaccine design and disease prognosis’’. That is not to say that it would be unusual to have multiple infections of the same virus. This was documented several times in his reports on the epidemic of smallpox in Trinidad from 1902 to 1904.
研究小组共同得出以下结论:“我们的结果表明,原发性SARS-CoV-2感染可以预防随后的暴露,这对疫苗设计和疾病预后至关重要”。这并不是说同一病毒被多次感染是不寻常的。他在1902年至1904年间特立尼达关于天花流行的报告中多次记录了这一点。
On page 83, Dr. Seheult talks about second attacks, the possibility of second attacks was recognized as far back as the 10th Century by Rhazes, the Arabian Galen, and his experience has been confirmed by many observers up to the present day. He goes through and actually documents in several patients that he attended to in Trinidad on people who had multiple bouts of smallpox, even some that had been vaccinated successfully. And who is the author? Dr. Murray Francois Raoul Seheult who happens to be my great grand uncle. He was the top surgeon in the colonial hospital in Port of Spain, Trinidad.
在第83页上,Seheult博士谈到了第二次袭击,Rhazes,Arabian Galen早在10世纪就认识到第二次袭击的可能性,直到今天,他的经验已得到许多观察家的证实。他仔细检查并实际记录了他在特立尼达(Trinidad)接受过治疗的几例患者,这些患者患有多发性天花,甚至有些人已经成功接种了天花。谁是作者?穆雷·弗朗索瓦·拉乌尔·塞休特, 特立尼达西班牙港殖民医院的高级外科医师, 也是我曾祖父的兄弟。
Despite this though reinfection is a rare thing. In this case, in the SARS-CoV-2 situation it seems as though the virus follows what we normally would see, which is if there isn’t that much of a change in the virus, hosts develop immunity to it.
尽管如此,再感染还是很罕见的。在这种情况下,在SARS-CoV-2情况下,病毒似乎遵循了我们通常看到的样子,也就是说,如果病毒的变化不大,则宿主会对它产生免疫力。
So if that’s the case, can we have blood tests quickly that would check for antibodies? It could be very helpful if we could check for antibodies because we could see who was actually infected, how widespread is the infection. If it is widespread enough, you might be able to actually at 50, 60 even 70 percent get into herd immunity where the virus would not spread as fast, and you would not have to do isolation.
因此,是的,我们可以快速进行血液检查以检查抗体吗?如果我们可以检查抗体,可能会很有帮助,因为我们可以看到实际感染者,感染程度。如果它足够广泛,您实际上可以以50%,60%甚至70%的速度进入畜群免疫,而病毒不会以如此快的速度传播,因此您不必进行隔离。
In addition to that, you wouldn’t have to worry about personal protective equipment in healthcare providers who already have antibodies because they wouldn’t be able to get the disease again.
除此之外,您不必担心已经有抗体的医疗保健提供者中的个人防护设备,因为他们将无法再次感染该疾病。
Here’s an article that was published in Science that looks for new blood tests. They basically go over the same things that we’ve been talking about, companies have been racing to develop antibody tests.
这是一篇刊登在《科学》杂志上的文章,旨在寻找新的血液测试。他们基本上处理了我们一直在谈论的相同事情,公司一直在竞相开发抗体测试。
Here’s one out of Icahn School of Medicine at Mount Sinai. They posted a preprint yesterday describing a SARS-CoV-2 antibody test that they’ve developed. It’s a relatively simple procedure and other labs could easily scale it up. Then they go on to describe exactly what we’ve talked about, where they find that this spike protein on the outer coat to see whether or not it will bind to antibodies if they’re there, and if they do bind to these receptor-binding-domains as we talked about, then it would trigger a detection so that you could see whether or not the antibodies are there.
这是西奈山伊坎医学院的一所。他们昨天发布了预印本,描述了他们开发的SARS-CoV-2抗体测试。这是一个相对简单的过程,其他实验室可以轻松地扩大规模。然后,他们继续准确地描述我们所讨论的内容,他们发现外层的这种尖峰蛋白可以观察它是否会与抗体结合(如果它们存在的话)以及它们是否确实与这些受体结合-就像我们所说的结合域,那么它将触发检测,以便您可以查看抗体是否存在。
Here’s another antibody test, BioMedomics, who is still seeking FDA approval on this COVID-19 rapid diagnostic test. You can see here that it’s fairly simple. We’ll put a link into the description below regarding this, but in terms of the sensitivity and specificity, let’s take a look at that.
这是另一种抗体测试BioMedomics,他仍在寻求COFID-19快速诊断测试的FDA批准。您可以在这里看到它非常简单。我们将在下面的描述中添加一个与此相关的链接,但就敏感性和特异性而言,我们来看一下。
This was published in the Journal of Medical Virology, the Development and Clinical Application of a Rapid IgM. Remember we talked about IgM being in the acute phase and IgG being in the more chronic phase, combined antibody test for SARS-CoV-2 infection diagnosis. The overall testing sensitivity was 88.66%, meaning that if you had a negative test you could be 88.66% sure that that was not a false negative result.
这发表在《医学病毒学杂志》中,快速IgM的开发和临床应用。记得我们曾说过IgM处于急性期,而IgG处于较慢性期,联合抗体测试可诊断SARS-CoV-2感染。总体测试灵敏度为88.66%,这意味着如果您进行阴性测试,则可以确保88.66%的判断结果不是假阴性。
Additionally, specificity was 90.63%; that means that if the test was positive there is a 90.63% chance of it being a true positive. Again, high sensitivity means that if it is negative, you can rule out; high specificity means that if it is positive you can rule in. In both cases here, we’ve got good results.
另外,特异性为90.63%。这意味着,如果测试为阳性,则有90.63%的机会是真正的阳性。同样,高灵敏度意味着如果它为负,则可以排除;高特异性意味着如果它是阳性的话,您可以介入。在这两种情况下,我们都有很好的结果。
So we hope that this test gets FDA approved soon so that we are able to do antibody testing to see who has had the disease already, and who may not have known it. That’ll give us an idea about herd immunity and how fast this virus is going to continue to spread. Remember that if 50 to 60 percent of the people in a community already have tested positive for the virus, it is very difficult for that virus to spread much more. Also, healthcare workers can be tested, and if they’re positive and have already had the disease, that could potentially save equipment for those that have not yet tested positive.
因此,我们希望该测试能够尽快获得FDA的批准,以便我们能够进行抗体测试,以查看谁已经患有该疾病,以及谁可能不知道该疾病。这将使我们对牛群的免疫力以及这种病毒将继续传播的速度有所了解。请记住,如果社区中50%到60%的人已经对该病毒进行了阳性检测,那么该病毒很难传播更多。另外,可以对医护人员进行测试,如果他们是阳性的并且已经患上了疾病,则可能为那些尚未测试出阳性的人节省设备。
While we went over a lot of things today, I would offer you a couple of reminders for those health care providers that want a refresher course or to learn it for the first time, don’t forget our free course on updating and learning about ventilator management.
虽然今天我们讨论了很多事情,但我想为那些想要进修或首次学习复习课程的医疗保健提供者提供一些提醒,请不要忘记我们免费的有关更新和学习呼吸机的课程管理。
I hope to over the next number of days this week go over practical things that we can do to improve our immunity as this virus continues to spread throughout our community.
我希望在本周接下来的几天里,研究一些实际的方法,以提高这种免疫力,因为这种病毒继续在整个社区中传播。
Thanks for joining us.
感谢您加入我们。




Add comment