How COVID-19 Infection Attacks the Immune System & Differs from HIV (Lecture 55)
COVID-19感染如何攻击免疫系统及与HIV的不同(第55讲)
Welcome to another MedCram COVID-19 update. Let’s go to Worldometer and take a look at the individual numbers at this point. It looks like the daily new cases in the United States are starting to level off and maybe even reduce a bit. Here we can see a graph of daily new deaths in the United States, and that seems to be going down as well.
欢迎收听MedCram COVID-19最新课程。现在让我们转到Worldometer,看看各个数字。看起来美国的每日新病例开始趋于稳定,甚至可能有所下降。在这里,我们可以看到美国每日新增死亡人数的图表,而且这一数字似乎也在下降。
[It’s] a kind of a disturbing Nature article that was just published recently looking at the SARS-CoV-2 infection pattern, and it seems to indicate that SARS-CoV-2 may have another target in the human body, and that is the T lymphocyte, which is very important in the immune system.
这是最近发表的有关SARS-CoV-2感染模式的一篇令人不安的Nature文章,似乎表明SARS-CoV-2可能在人体中还有另一个靶标,这就是T淋巴细胞,它在免疫系统中非常重要。
This article goes through a number of molecular techniques in its communication. It’s open communication with nature.com, and it talks about how we know that the SARS-CoV-2 virus is interacting with the ACE2 receptor on the Type II pneumocytes.
这篇文章详细论述了许多分子技术,在nature.com网上开放,讨论了我们如何知道SARS-CoV-2病毒正在与II型肺细胞上的ACE2受体相互作用。
But they also show that in patients with Covid-19, some studies reported that there was lymphocytopenia, basically meaning low white blood cell counts, and part of that white blood cell counts are the lymphocytes, specifically the CD4 and CD8 lymphocytes.
他们还说明了在Covid-19的患者中,一些研究报告说存在淋巴细胞减少症,基本上意味着白细胞计数低,部分白细胞计数是淋巴细胞,特别是CD4和CD8淋巴细胞。
They also mention that this was also a finding in MERS. MERS was the Middle East Respiratory Syndrome that was seen back in 2012. In this article, they talked about their molecular techniques that tried to set out and to see whether or not SARS-CoV-2 also infects T cells, resulting in lymphocytopenia.
他们还提到,这种情况也出现在MERS中。 MERS是2012年出现的中东呼吸综合症。在本文中,他们谈论了他们的分子技术,这些技术试图阐明SARS-CoV-2是否也感染T细胞,从而导致淋巴细胞减少。
What they were able to show here is with SARS-CoV, which, remember, is the SARS virus of 2002, and the SARS-CoV-2, which of course is the recent one 2019 and now 2020. They were able to see whether or not these viruses, which appear as these bright dots in the fluorescence field, were able to infect these cells and fuse with them.
他们在这里可以显示的是SARS-CoV,这是2002年的SARS病毒,以及SARS-CoV-2,当然是最近的2019年和现在的2020年。他们能够看到这些病毒(荧光场中的亮点)是否能够感染这些细胞并与之融合。
As you can see SARS-CoV, there was no fusion cells. In other words, there weren’t these big blobs of cells that were kind of lighting up. You can see that nothing here of the sort. But when they did it with SARS-CoV-2, they were able to see these blobs of cells where the virus was able to get in. Therefore, they were able to show that the virus was able to fuse with these T lymphocyte type cells and show that the SARS-CoV-2 virus through a spike protein was able to infect and go into these T lymphocytes.
正如大家看到的,SARS-CoV没有融合细胞。换句话说,并没有这些大的发光的细胞团。你在这里看不到任何东西。但是,当他们使用SARS-CoV-2进行处理时,他们能够看到病毒能够进入的这些斑点。因此,他们能够证明该病毒能够与这些T淋巴细胞型细胞融合,这说明SARS-CoV-2病毒通过刺突蛋白能够感染并进入这些T淋巴细胞。
The good news though is when the SARS-CoV-2 virus infects the T Cell via the CD 147 protein, the infection is a dead end, and it’s known as abortive. On the other hand, when the virus infects the Type II pneumocytes via the ACE 2 receptor, that infection of that cell does lead to replication of the virus. And the protein that the SARS-CoV-2 uses to enter into the T-cell is the CD 147, that is present on the surface of the T lymphocytes.
好消息是,当SARS-CoV-2病毒通过CD 147蛋白感染T细胞时,这种感染是死胡同,被称为流产。另一方面,当病毒通过ACE 2受体感染II型肺细胞时,该细胞的感染确实导致病毒复制。SARS-CoV-2用于进入T细胞的蛋白质是CD 147,它存在于T淋巴细胞的表面。
So some have compared SARS-CoV-2 with HIV in this sense because there are some similarities. SARS-CoV-2 is an RNA virus, so that’s RNA inside SARS-CoV-2 here on the left, and it’s also an RNA virus in HIV.
有人将SARS-CoV-2与HIV在这方面进行了比较,因为存在一些相似之处。 SARS-CoV-2是一种RNA病毒,左边这个是SARS-CoV-2内部的RNA,它也是HIV中的RNA病毒。
But let’s take a look at the differences between those. Let’s first look at HIV. So with HIV, you have an RNA virus and in this case, it docks with the docking protein CD4, which targets the T-cell specifically, in fact the helper T cells. But in this case, when the virus docks with the protein and comes into the cell, what is released is the RNA.
我们来看一下两者之间的区别。首先让我们看一下艾滋病毒。HIV有RNA病毒,在这种情况下,它与蛋白CD4对接,后者专门针对T细胞,实际上是辅助T细胞。但是在这种情况下,当病毒与蛋白质对接并进入细胞时,释放的是RNA。
Now, the RNA and a couple of other enzymes are used in this infection without getting into too much detail, but there are two proteins that are very important to understand. The first one is something called reverse transcriptase (RT), and another one is called integrase or I. And what reverse transcriptase does in HIV is it uses the RNA as a template to make a DNA molecule and then very quickly it will make the other double strand of that DNA molecule.
RNA和其他几种酶很容易造成这种感染,但是有两种蛋白质非常重要。第一个是逆转录酶(RT),另一个是整合酶或I。逆转录酶在HIV中的作用是:它使用RNA作为模板来制造DNA分子,然后很快就会制造出DNA双链。
Then what happens is integrase takes this molecule, this double-stranded DNA molecule, which is a copy essentially of the RNA from the original HIV, and what does it do is it actually integrates it into the host cell’s DNA, and it stays there permanently so that when the cell divides and divides, a copy of the HIV RNA will now be incorporated into its very nucleus. So every single time it divides, the progenitor T cells, or the daughter T cells of this division, will have that HIV genome in it.
然后整合酶带走这个分子,这个双链DNA分子,基本上是原始HIV的RNA的一个拷贝,它的作用是将其实际上整合到宿主细胞的DNA中,并永久地留在那里,这样,当细胞分裂时,HIV RNA的一个拷贝就会被整合到细胞核中。因此,每分裂一次,祖先T细胞或该分裂的子代T细胞中都会有HIV基因组。
So what can happen is when you have RNA polymerase coming by and reading this off, it will read this area off and it will make new copies of the HIV virus in terms of RNA, which can then be packaged and new virus can be made, so you can see how a HIV infection is going to be incorporated into the very cell. That’s different with SARS-CoV-2.
因此,当你得到RNA聚合酶并将其读取时,它将读取该区域,并以RNA的形式复制HIV病毒,然后将其包装并制造新病毒,这样你就可以了解HIV感染是如何被整合到整个细胞中。这与SARS-CoV-2不同。
With SARS-CoV-2, when there is an infection of the RNA virus, it will dock with a different protein. In this case, it is the CD 147 and what will happen here is that the RNA will come into the cell and it will stay there and if there is another CD 147, there will be another virus with a genome and it will dock and another virion will come in and there will be another one. And so what happens is this cell will build up with a bunch of RNA genomes from the SARS-CoV-2.
对于SARS-CoV-2来说,当感染RNA病毒时,它将与另一种蛋白质对接。在这种情况下,它是CD 147,此时将发生的是RNA进入细胞并停留在细胞中,如果存在另一CD 147,将存在另一个带有基因组的病毒,它将进行对接,另一种病毒中病毒粒子会进来,还会有另外一个。因此,发生的情况是该细胞将由SARS-CoV-2的一堆RNA基因组构建。
So you can see interestingly this cell here is just filled with the virions, that shows fusion. So this article shows again how important it is to have a functional and good immune system, especially since this virus seems to be doing a one-two punch on it.
你可以看到有趣的是,该细胞充满了病毒粒子,这就是融合。这篇论文再次显示了拥有一个功能强大且良好的免疫系统的重要性,尤其是因为该病毒似乎对其进行了1-2次攻击。
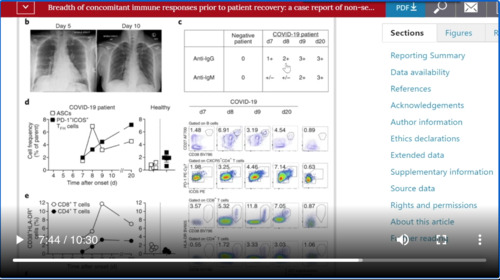
We’ve already shown a couple of times this article from nature medicine. This was a patient that was hospitalized in Australia. And they did a very good job looking specifically at the lymphocytes in this patient and we can see here that in terms of CD8 and CD4 cells if you look at what is normal in a healthy subject. These were actually a little bit higher and lower respectively in that category, but that this patient seemed to recover and there was a large increase in the number in this case of 8 cells and a large increase here in the number of CD4 cells. That may be the determining factor in whether a patient recovers or not.
我们已经介绍过几次有关自然医学的文章。这是在澳大利亚住院的病人。他们专门针对该患者的淋巴细胞做了非常出色的工作,如果你看一下健康受试者的正常情况,我们可以在这里看到CD8和CD4细胞方面的信息。实际上,该类别中有的稍微高一些,有的稍微低一些,但是该患者似乎已经康复,CD8 及CD4细胞数量大大增加。这可能是患者是否康复的决定因素。
The other interesting thing I found about this article was it showed when anti IgG and IgM were increasing in this patient, you can see here that it was by day 9 that the anti-IgM was two plus to three plus and anti-IgG was already starting to come up by day 7 and day 8. So that’s an important thing to keep in mind, especially as we enter into a season of antibody testing.
我在这篇文章中发现的另一件有趣的事情是,当该患者的抗IgG和IgM升高时,你可以在这里看到第9天抗IgM为2加、3加,而抗IgG已经存在,在第7天和第8天开始出现。因此,请记住这一点,尤其是在进入抗体测试的季节时。
And speaking of improving your immune system, I also wanted to sort of clear up a number of comments and things that I’ve seen. There seems to be a theory at least that sauna baths or hot air can kill the virus and I don’t believe that anyone is making that claim at least here at MedCram. The claim or the interesting aspect is that heat followed by cold can actually improve immunity, which in turn can help potentially kill viruses, perhaps even Covid-19.
谈到改善你的免疫系统,我还想澄清一些意见和见过的事情。至少有一种理论认为,桑拿浴或热空气可以杀死该病毒,而且我认为除了在MedCram没有人提出这一说法,即加热后再进行冷却实际上可以提高免疫力,进而可以帮助潜在地杀死病毒,甚至Covid-19。
There seems to be some discussion of that. Even going back a number of years, I found this article for those who are really interested in this type of research to be a good clearing house and discussion of that. This is from The Business Insider, the article titled taking regular sauna seems to transform your health—more evidence that there could be a 3rd pillar of physical fitness be on diet and exercise.
对此似乎有一些讨论。甚至追溯到几年前,我觉得对于那些对此类研究非常感兴趣的人来说这篇文章是一个很好的讨论依据。这来自《商业内幕》(The Business Insider),标题为定期洗桑拿似乎可以改变你的健康–更多证据表明,饮食和运动可能是身体健康的第三大支柱。
And you can see here that they list off that people in Finland regular take saunas, where they go into extremely hot dry rooms for short periods of time. The more saunas people take, the healthier they seem to be. According to a new medical review, health benefits include improved heart health, mental health, immune system function.
你会在这里看到他们列出了芬兰的人们定期去桑拿,然后在短时间内进入极热的干燥房间。越桑拿,就越健康。根据新的医学评论,健康益处包括改善心脏健康,心理健康,免疫系统功能。
And there’s also significant evidence that exposing yourself to cold temperatures improves health as well. And there’s actually a number of important and interesting medical articles and their links all through this article and I encourage you to take a look. We’ll leave a link to this in the description below.
而且,还有大量证据表明,将自己置于寒冷的环境中也可以改善健康状况。实际上,这篇文章提供了许多重要而有趣的医学文章及链接,我鼓励大家看一下。我们将在下面的描述中提供链接。
I also wanted you to be aware of some news that’s breaking. We talked about ventilators and using one ventilator to ventilate multiple patients and we talked about how there was a letter from the AARC and a number of other societies that are involved with ventilation. They were concerned that this would not be a good idea because patients would have different sized lungs and different compliance.
我还希望大家了解一些突发事件。我们讨论了呼吸机,使用一台呼吸机为多名患者通气,我们还谈到了AARC和许多其它涉及呼吸的团体的来信。他们担心这不是一个好主意,因为患者的肺部大小不同,适应性也不同。
Well, there was a press release today showing that there is a new device that would allow control over the amount of tidal volume going to specific patients, even though they’re hooked up to one ventilator, and that’s called a vent multiplexer. And apparently it was successfully deployed at Yale New Haven Hospital for Crisis Care Co-Ventilation during this pandemic. And apparently according to this press release, it was successful. They are still working with the FDA for full approval.
今天有新闻发布表明,有一种新设备可以控制到达特定患者的潮气量,即使这些患者已连接到一个呼吸机,也就是所谓的通风口多路复用器。显然,在这一大流行期间,它已成功地部署在耶鲁大学纽黑文医院的危急护理共用呼吸中。显然,根据这条新闻,它是成功的。他们仍在与FDA进行沟通,期望获得全面批准。
But that that work is going through right now as we speak. So we’ll see what happens. I think that’s interesting.
这项工作现在正在进行中,我们将看到结果。我认为这很有趣。




Add comment