粪口传播、康复与死亡率
Fecal-Oral Transmission & Recovery vs Death Rate (coronavirus lecture 9)
Welcome to another MedCram coronavirus update. And as of today, we have 362 deaths, which is up from 305 yesterday, and we have 17,392 infected, which is up from 14,556. Now this ratio that we’re looking at here is simply the ratio of confirmed deaths to confirm infected.
欢迎来到另一个MedCram冠状病毒更新。截至今天,我们有362人死亡,比昨天的305人增加了,我们有17392人被感染,比14556人有所增加。现在,我们在这里查看的比率只是已确认死亡与已确认感染比率。
Of course, people are going to be diagnosed with the infection before they might have a chance of dying. So there’s a time lag there. So it’s not an accurate case of fatality or mortality rate, but it is something that we can look at and track.
当然,人们将有可能被诊断出感染,然后才有可能死亡。因此那里存在时间滞后。因此,这不是死亡或死亡率的准确案例,但我们可以研究和跟踪。
The other thing that you might have noticed on the website that we reference, and we’ll make a link to it, which is a nice official reporting dashboard from Johns Hopkins, is this 487 recovered. We’ll talk more about that as well. What are the criteria for recovered, and we’ll talk a little bit about the Lancet article and also some reporting out of China today.
您可能会在我们引用的网站上注意到的另一件事,我们将进行链接,这是Johns Hopkins的一个不错的官方报告仪表板,它已被回收487。我们还将讨论更多。回收的标准是什么,我们将略谈《柳叶刀》的文章以及今天在中国以外的报道。
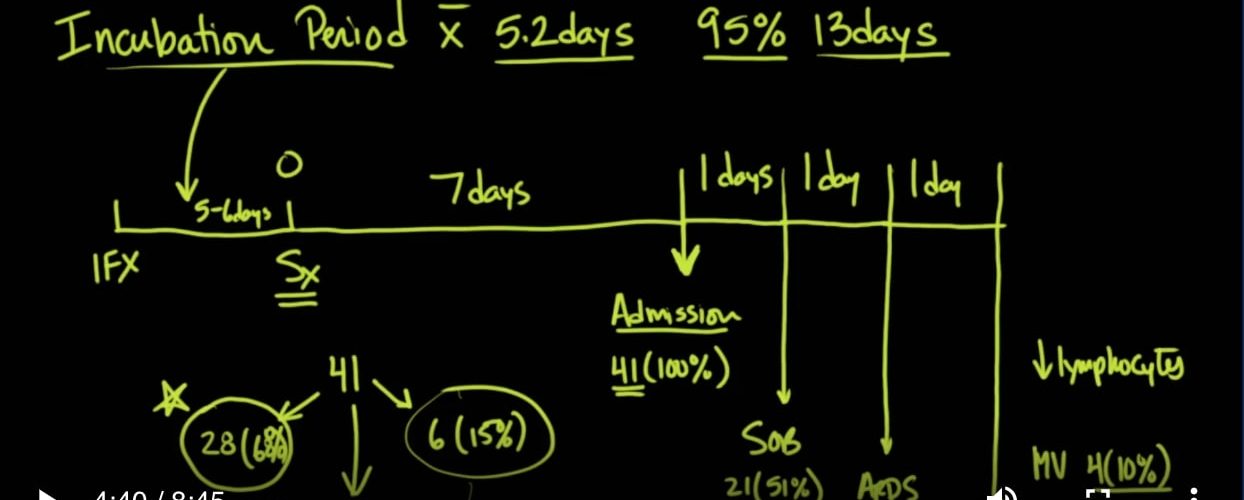
So in the Lancet article, which will give you a link to some really good information, the incubation period on average for these 41 patients that were admitted to a hospital right there in the middle of this epidemic was 5.2 days, but 95% of all of them had the incubation period within 13 days. You know that for citizens coming to the United States from that area, they’re holding them for at least 14 days to make sure that they do not have the virus.
因此,在柳叶刀文章中,该文章将为您提供一些非常好的信息的链接,在这种流行病的中间,这41名在该病住院的患者的平均潜伏期为5.2天,但占总数的95%他们有13天的潜伏期。您知道,对于从该地区来到美国的公民,他们将他们关押至少14天,以确保他们没有这种病毒。
Incidentally, there was a German plane yesterday that flew in with German nationals, and when they screened them on the plane, there were two people that were positive for coronavirus on that plane.
顺便说一句,昨天有一架德国飞机与德国国民一起飞来,当他们在飞机上对他们进行检查时,有两个人对该飞机上的冠状病毒呈阳性反应。
So let’s look closer at this Lancet article because I think it’s very instructive in terms of periods of time and looking at things. So here we have the infection that starts, and that incubation period would go right in here. So on average, it would be about, you know, five or six days, and then the time from symptom onset to admission to the hospital. That’s a very key thing there because most patients probably don’t even go to the hospital, and they may do just fine.
因此,让我们仔细看一下《柳叶刀》上的这篇文章,因为我认为这对于时间和事物的观察很有启发性。因此,在这里我们开始感染,潜伏期就在这里。因此,平均而言,大约需要五到六天,然后是从症状发作到住院的时间。那是非常关键的事情,因为大多数患者甚至可能都不去医院,而且他们可能做得很好。
But for those that do go to the hospital, it was noted to be about a seven-day period. And then from admission, and that was 100% of the cohort that was looked at in the study because they looked at those 41 patients within a day admitting to the hospital, about 51 percent of them developed shortness of breath, another day later 27% went into ARDS. And if you want more information about ARDS, look at our MedCram video on this channel titled How Coronavirus Kills. Then another day before they got to the Intensive Care Unit, and there about 10% or for patients requiring mechanical ventilation.
但是对于那些确实要去医院的人来说,大约需要7天。然后从入院开始,这是研究中研究的同类人群的100%,因为他们在入院的一天之内检查了这41名患者,其中约51%出现了呼吸急促,第二天又有27%进入ARDS。如果您想了解有关ARDS的更多信息,请观看此频道上名为冠状病毒如何杀死的MedCram视频。然后在他们到达重症监护室的前一天,那里大约有10%的病人需要机械通气。
So what was the outcome of this study? And I think it was very interesting. Of the 41 people at the time of publication of this in the Lancet, there were 28 people that were discharged home. There were six people that passed away. That’s about 15%, and of the 28 that is a 68%, which leaves seven that were still alive, and in the hospital being treated.
那么这项研究的结果是什么呢?我认为这非常有趣。在《柳叶刀》上发行该刊物时的41人中,有28人被出院了。有六个人去世了。大约占15%,在28个中占68%,剩下7个还活着,并在医院接受治疗。
So the question is what were the criteria? And this gets back to that number that we see on the site. What were the criteria for allowing these people to go home? And this is very important. So from my understanding, there are some guidelines now that are being instituted nationally in China about what constitutes someone that’s recovered. And at least for this hospital, it was ten days without a fever; it was that the chest x-ray was improving because all 41 patients had abnormal CT scans chest x-rays.
那么问题是什么标准?这又回到了我们在网站上看到的数字。允许这些人回家的标准是什么?这非常重要。因此,据我了解,目前在中国全国范围内制定了一些有关康复者的指导方针。至少对于这家医院来说,这是十天没有发烧。这是因为胸部X线检查有所改善,因为所有41例患者的CT扫描均异常。
This next one is important. To be discharged home, there has to be no virus detected in the upper respiratory tract. And so that’s a pretty high bar, and with that 68% of those people that enter the hospital were able to go home and deemed cured. We don’t know what happened to the other seven. So if we look at just those that entered into the hospital, we’re looking at about a 15% mortality rate in the least.
下一个很重要。要出院,上呼吸道必须没有发现病毒。因此这是一个很高的标准,进入医院的患者中有68%能够回家并被治愈。我们不知道其他七个发生了什么。因此,如果仅查看那些进入医院的患者,则死亡率至少约为15%。
And from there, it could go up depending on what those other seven did. If one or two of those died, then the mortality rate goes up. By stress again, this is not the overall mortality rate of the virus; this is the mortality rate for those people that have to go to the hospital because their symptoms were so severe.
从那以后,它可能会上升,这取决于其他七个国家的所作所为。如果其中一人或二人死亡,则死亡率会上升。再次强调,这不是病毒的总死亡率。这是因为症状非常严重而必须去医院的人的死亡率。
Okay, three other stories I want to talk about real quick. There was in the local Chinese media a story that I picked up, and I’ll work in the link to that one as well in the description below, a doorknob was found to have the RNA PCR of the coronavirus on it. So again this highlights the need for hand hygiene carrying around, alcohol-based hand sanitizers. Make sure you’re washing your hands.
好的,我想谈谈另外三个故事。我在当地的中国媒体中听到一个故事,在下面的说明中,我还将与之链接,一个门把手上发现了冠状病毒的RNA PCR。因此,这再次强调了随身携带酒精类洗手液的手卫生的必要性。确保您正在洗手。
The other thing I want to highlight is that there were some local media in China about a patient being discharged home. This is a patient that was 30 years old. He was admitted on the 20th of January, and he was being discharged today on the 3rd of February. Again, I looked very carefully at the media report of what was the criteria, and they did mention that this was the standard criteria for discharging a patient home.
我要强调的另一件事是,中国有一些当地媒体报道了一名患者出院回家。这是一名30岁的患者。他于1月20日入院,他于2月3日今天被释放。再次,我非常仔细地查看了媒体报道中的标准,他们确实提到这是出院的标准。
In this case, the patient had a normal temperature times three days, and they were doing PCR to look specifically for the RNA of this virus, and it was negative, and they were checking it at every 24-hour intervals. So this patient felt better. The PCR was negative for the virus, wasn’t shedding it in other words, and temperature above normal for three days. So I think that adds a little bit more in terms of what that number means on the website people that have recovered. Think about this though in terms of a timeline.
在这种情况下,患者的温度为正常温度三天,他们正在进行PCR检查以专门寻找该病毒的RNA,结果为阴性,并且每隔24小时检查一次。所以这个病人感觉好多了。 PCR对病毒是阴性的,换句话说,它没有脱落,并且温度超过正常温度三天。因此,我认为,该数字对已康复网站的人们的影响增加了一些。不过,请从时间上考虑一下。
The first thing that’s going to happen is someone’s going to a confirmed case. The second thing that could happen is they could die. And then the third thing that would happen is that they would recover.
将会发生的第一件事是某人要确认一个病例。可能发生的第二件事是他们可能会死亡。然后发生的第三件事是它们将恢复。
Obviously, they’re not going to recover after they die. But these things are going to happen in this order. So it’s going to take the longest to have a recovery? It’s going to take the shortest to have it confirmed case, and it’s going to take intermediate somewhere between that time to have a death. So look for in the future as we progress through this epidemic, that the number of recoveries is going to surpass the number of deaths, and we hope that that is by a large amount.
显然,他们死后不会恢复。但是这些事情将按此顺序发生。因此,恢复需要最长的时间吗?确认病例将用最短的时间,而在这段时间之间要在中间死亡。因此,随着我们在这一流行病中的前进,寻找未来的机会,就是康复的人数将超过死亡人数,我们希望这是一个很大的数目。
Let’s talk a little bit about how it spreads. So we all are familiar with the common cold the flu, and the importance for mask, and also the need for eye protection in this case, especially in the healthcare setting.
让我们谈谈它的传播方式。因此,我们都熟悉感冒流感,戴口罩的重要性以及这种情况下对眼睛的保护,尤其是在医疗机构中。
What may be something that we may have underestimated, and that is the fecal-oral route, and the reason why that’s the case, and we’ll put a link to this in the description, is because the man in Washington state, they found the coronavirus in his stool. And why this is important is because this goes back to 2002, 2003 where there was a big outbreak of SARS in a particular apartment complex in China, and it was because of this toxic viral plume after the man had diarrhea, and that aerosolize viruses into the air, and it went into the other apartments, and that’s where the other people picked up the virus. And so it is possible that this fecal-oral route may be a big determining factor.
我们可能低估了什么,那就是粪-口途径,之所以如此,我们将其与描述联系起来,是因为他们发现华盛顿州的那个人粪便中的冠状病毒。之所以如此重要,是因为这可以追溯到2002年,2003年,当时中国某特定的公寓大楼内爆发了严重的非典,这是因为该人腹泻后出现了这种有毒的病毒羽状病毒,病毒散播到空中,然后进入其他房间,其他人在那里拾起了病毒。因此,这种粪口途径可能是一个很大的决定因素。
But it highlights that fecal-oral transmission of this virus is potentially in play, and so washing hands is an important thing to understand. We are witnessing, and in the middle of, a human tragedy that is pretty scary to say the least. There are a lot of people that are suffering, but there are some things that we can do about this. We can educate ourselves. We can understand the virus. We can make sure that we’re doing everything that we can to prevent that virus from spreading. We can make a difference.
但是,它突显了这种病毒的粪便传播途径可能正在发挥作用,因此洗手是一件很重要的事情。我们正在目睹并在其中发生至少可以说非常可怕的人类悲剧。有很多人在受苦,但是对此我们可以做一些事情。我们可以自我教育。我们可以了解该病毒。我们可以确保我们正在尽一切努力防止该病毒传播。我们可以有所作为。




Add comment