抗体,病死率,临床建议,二次感染
Antibodies, Case Fatality, Clinical Recommendations, 2nd Infections (Lecture 21)
Welcome to another MedCram lecture. We will talk about the coronavirus update, and we see here are 7,500 total confirmed cases based on the data from the WHO and CDC. Coming out of China, total deaths over 2000; total recovered 14, 772. If we look at the WorldOmeter, as it’s correctly pronounced, we can see here there are active and inactive cases. Closed cases 16,814, 88% of those have been recovered or discharged, and 12 percent deaths in the closed cases so far. Of course, these numbers are underreported.
欢迎参加另一个MedCram讲座。我们将讨论冠状病毒的更新,根据世卫组织和美国疾病预防控制中心的数据,我们在这里总共确认了7,500例确诊病例。从中国出来的总死亡人数超过2000;总共恢复了14,772个。如果我们正确地看一下WorldOmeter,我们可以看到这里有活动和不活动的案例。结案案件16,814例,其中88%已康复或出院,迄今为止,结案案件中有12%的死亡。当然,这些数字被低估了。
Most of those cases were mild cases, however. If we break those cases down again into the difference between what’s going on in China and what’s going on outside of China, we can get another picture. You can see here the trend is that every day there seems to be more and more new cases. Well, inside of China, the number of cases is actually diminishing, as we can see here overall. If we go up to total deaths, over 2,000 deaths total.
但是,这些病例大多数是轻度病例。如果我们将这些情况再次分解为中国境内发生的事情与中国境外发生的事情之间的差异,我们可以得到另一幅图。您可以在这里看到趋势是,每天似乎都有越来越多的新病例。好吧,在中国内部,案件数量实际上正在减少,正如我们在此处可以看到的那样。如果我们达到总死亡人数,则总共有2,000多人死亡。
I want to talk a little bit about what’s going on in terms of what the labs are doing to fight coronavirus, the covid-19 disease, specifically nice interview here on NPR regarding antibodies. First one to talk a little bit about antibodies, and how they’re made. So you have these B cells, and they each have different receptors on these B cells. These B cells are made to do one thing really; that is to make antibodies. And these receptors on the cells are there to receive any type of antigen that you might come in contact with. An antigen could be a protein of a virus or a protein of a bacteria, etc. etc.
我想谈谈实验室在抵抗冠状病毒,covid-19疾病方面所做的工作,特别是在NPR上有关抗体的采访。首先谈一些关于抗体及其制造方法的知识。因此,您拥有这些B细胞,并且它们在这些B细胞上各自具有不同的受体。这些B细胞实际上是在做一件事情。那就是制造抗体。细胞上的这些受体可以接收您可能接触的任何类型的抗原。抗原可以是病毒的蛋白质或细菌的蛋白质等。
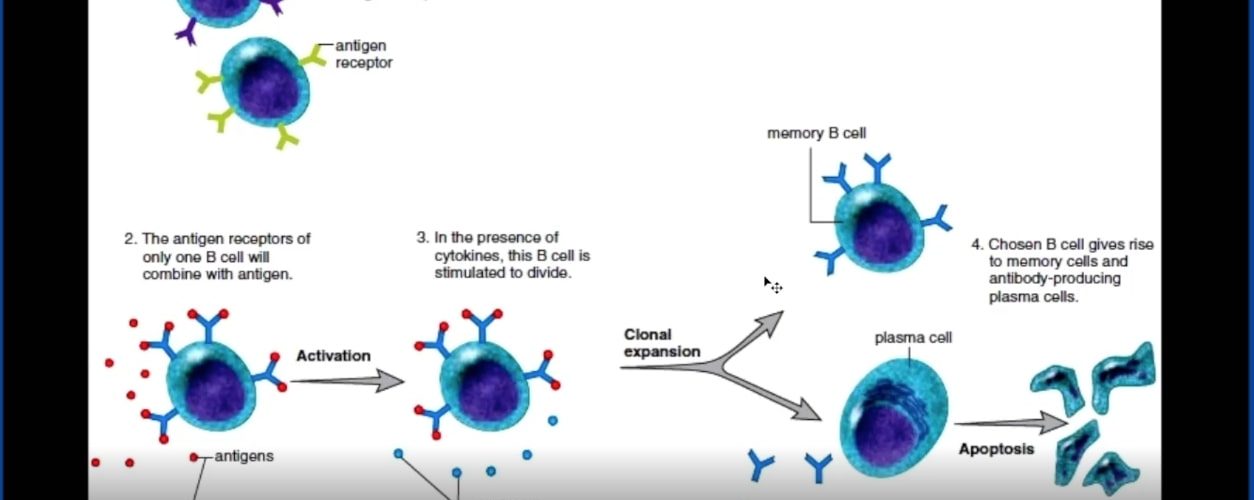
What is really quite amazing is that you have so many different types of receptors on millions and millions of B cells that just about any kind of foreign protein that gets introduced into your body will make a b-cell against that. And so here we can see that each B cell has a different antigen receptor, and the antigen receptors of only one B cell will combine with that antigen.
真正令人惊讶的是,您在成千上万的B细胞上有如此多种不同的受体,几乎任何一种引入人体的外源蛋白质都会使B细胞产生这种作用。因此,在这里我们可以看到每个B细胞都有一个不同的抗原受体,只有一个B细胞的抗原受体会与该抗原结合。
So if you have a virus; that virus is going to stimulate its particular b-cell, and it will activate, and it will get help from T-cells, cytokines. And it will cause the cell to divide and rapidly enlarge into a huge clonal representation of that b-cell. So you have thousands, millions of these B cells, and all these B cells do is they produce antibodies, and these antibodies go out and attack cells that have the virus in it or the virus itself. And finally when the infection is done, then these B cells just kind of go away, but there’s always a certain amount of a population of these B cells ready to strike again if that virus comes again, and this is typically how it works with a particular virus.
因此,如果您有病毒;该病毒将刺激其特定的b细胞,并会激活,并会从T细胞,细胞因子获得帮助。它将导致细胞分裂并迅速扩大为该b细胞的巨大克隆表示。因此,您拥有成千上万的此类B细胞,而所有这些B细胞所做的就是它们产生抗体,这些抗体会消灭并攻击其中含有病毒或病毒本身的细胞。最后,当感染完成后,这些B细胞就消失了,但是如果该病毒再次出现,总是会有一定数量的这些B细胞再次发生攻击,这通常是通过与特定病毒。
So if you get a vaccine against the virus, like polio, if you get a vaccine against the virus, like the Hepatitis B virus, that vaccine goes through the same way. Here, you get an antigen stimulating a b-cell. Of course, when we give a vaccine in some of the cases, we give a vaccine that has just the protein without the virus, so you don’t get the actual disease, and that causes your B cells to make a lot of these antibodies in preparation for if you ever were to be infected with that virus, you’ll be ready to make an immune response.
因此,如果您获得了针对脊髓灰质炎的抗病毒疫苗,而您获得了针对诸如乙型肝炎病毒的抗病毒疫苗,那么该疫苗将以同样的方式进行。在这里,您获得了刺激b细胞的抗原。当然,在某些情况下注射疫苗时,我们所提供的疫苗仅含有不含病毒的蛋白质,因此您不会患上真正的疾病,这会导致您的B细胞产生大量此类抗体在准备感染该病毒的过程中,您将做好免疫反应的准备。
Of course, sometimes what happens is the virus may mutate, and so the proteins are different enough that the antibodies that you have against those proteins may not be as effective. This is kind of what happens with colds. You might get multiple colds in a year, and it’s possibly because, well, it could be a different virus of rhinovirus versus a regular coronavirus, or it could be a rhinovirus that’s mutated enough so that the former immunization that you got against the virus is no longer effective because it’s mutated.
当然,有时会发生这种情况,因为病毒可能会突变,因此蛋白质的差异足够大,以至于您针对这些蛋白质的抗体可能效果不佳。感冒就是这种情况。一年中您可能会多次感冒,这可能是因为,它可能是与常规冠状病毒不同的鼻病毒,也可能是经过充分变异的鼻病毒,因此您以前针对该病毒的免疫由于它已被突变而不再有效。
Well, going back to this interview. What they’re looking at is drugs that will prevent the virus from replicating, but there’s an interesting company that they’re looking at called ABcellera, which they identify antibodies from patients who have already recovered from infection because they’re finely-tuned immune systems have already figured out a way to clear the virus. So what they can do is they can look through millions of different immune cells and find the one that is right for coronavirus.
好了,回到这次采访。他们正在寻找能够阻止病毒复制的药物,但是他们正在寻找一家有趣的公司ABcellera,该公司可以从已经从感染中恢复过来的患者中识别抗体,因为他们的免疫力经过微调系统已经找到清除病毒的方法。因此,他们可以做的是,他们可以浏览数百万种不同的免疫细胞,找到最适合冠状病毒的细胞。
In fact, what they’ve done, and this is kind of amazing as they’ve taken mice, and instead of making mouse antibodies, these mice are actually using human immune system cells to make not mouse antibodies, but to actually make fully human antibodies, and that’s just amazing. So, of course, the next step is to inject these coronaviruses into these mice and start getting these antibodies out, and actually seeing whether or not they work. Testing them in trials and then seeing whether or not this antibody against the coronavirus, specifically the one that makes the covid-19 disease, otherwise known as SARS-COV2, is going to be effective.
实际上,他们做了什么,就像带了老鼠一样,这真是太了不起了,这些老鼠没有制造小鼠抗体,而是在利用人类免疫系统细胞制造的不是小鼠抗体,而是在制造真正的人类抗体。抗体,真是太神奇了。因此,当然,下一步是将这些冠状病毒注射入这些小鼠中,并开始清除这些抗体,并查看它们是否有效。在试验中对其进行测试,然后查看该抗冠状病毒抗体,特别是引起covid-19疾病的抗体,即SARS-COV2,是否会有效。
So this is one of the treatments that’s on the horizon, and the reason why this is really important for us to get, as we see here in this USA Today article, looking again at that data from China that we talked about yesterday. They’re looking at statistics here, and they’re saying that the coronavirus is 20 times more lethal than the flu based on the case fatality rate as the death toll as we talked about passes 2000.
因此,这是一种即将到来的治疗方法,也是对我们而言获得这种治疗非常重要的原因,正如我们在《今日美国》一文中所看到的,再次回顾了我们昨天谈到的来自中国的数据。他们在这里查看统计数据,他们说,根据案例死亡率(因为我们谈到的死亡人数超过2000),冠状病毒的致死性比流感高20倍。
We can see here that based on the calculations that they were doing, the global death toll from the virus was listed at 2009 as of Tuesday evening, and that the total infections rose to more than 75,000. If you do the calculation, the overall death rate for the virus was 2.3 percent. However, the season’s flu death in the United States was at about 0.1%, making this, of course, a more deadly than the regular flu, but not as deadly as the SARS outbreak back in 2002, which was at around 10%.
我们在这里可以看到,根据他们的计算,截至周二傍晚,该病毒的全球死亡人数已列于2009年,总感染人数上升至75,000多人。如果进行计算,该病毒的总死亡率为2.3%。但是,在美国,该季节的流感死亡人数约为0.1%,这当然比常规流感更具致命性,但不及2002年SARS爆发时(约10%)致命。
Fortunately, we have to talk about another physician who’s died in China, Dr. Liu. He was the director of a Chinese hospital at the epicenter of the coronavirus outbreak and was one of the neurosurgeons as well.
幸运的是,我们不得不谈论另一个在中国去世的医生刘博士。他曾是冠状病毒爆发震中的一家中国医院的主任,也是神经外科医师之一。
So these B cells, and how they become plasma cells, and how they secrete immunoglobulins, or antibodies. It is all very specific and distinct, including how viruses infect the human cells. This is something that I would like to go into a little more detail.
这些B细胞,以及它们如何变成浆细胞,以及它们如何分泌免疫球蛋白或抗体。这都是非常具体和独特的,包括病毒如何感染人类细胞。我想对此进行详细介绍。
There have been a lot of questions about immunity, and what happens after someone recovers, and we’ve seen some examples here the United States of people who have recovered, specifically the gentleman in Washington, but there have been some questions, some rumors, and some claims that people can get the virus twice, and that, for instance, people can have a lot worse reaction the second time around, and that there may not be immunity.
有关豁免权的问题很多,有人康复后会发生什么。我们在这里看到了一些美国康复者的例子,特别是华盛顿的绅士,但也有一些疑问,谣言,有些人声称人们可以两次感染该病毒,例如,人们第二次可能会有更差的反应,并且可能没有免疫力。
I haven’t seen any reports of that, and so it’s very difficult to come up with an answer to that question. I think it might be a little early in the course to see if that is in fact happening. One thing. I will make a point, however, is that often times when someone gets a viral infection, their ability to withstand secondary bacterial infections is reduced, and so it’s not uncommon to have secondary bacterial infections when someone has a severe viral infection.
我还没有看到有关此问题的报道,因此很难为该问题找到答案。我认为也许这还为时过早。一件事。但是,我要指出的是,通常当某人受到病毒感染时,他们承受继发性细菌感染的能力会降低,因此,当某人受到严重病毒感染时,继发细菌感染并不罕见。
And so I want to end this update with an excellent article that was published on the 12th of February 2020 on the practical recommendations for critical care and anesthesia teams caring for novel coronavirus patients, and I will put a link in the description below.
因此,我想以一篇出色的文章作为结尾,该文章于2020年2月12日发表,内容为照顾新的冠状病毒患者的重症监护和麻醉小组的实用建议,我将在下面的描述中添加一个链接。
This article that is written in Canada talks about their experience with the SARS virus back in 2002. And it talks about very practical things to do. For instance, in the Intensive Care Unit, what kind of personal protective equipment to be wearing; how the flow of air in these rooms; whether or not they’re negative or positive pressure rooms are very important.
这篇写在加拿大的文章讨论了2002年他们对SARS病毒的使用经验,并谈到了非常实际的事情。例如,在重症监护室,要佩戴什么样的个人防护设备;这些房间的气流如何;无论是负压室还是正压室都很重要。
For instance, if you are doing, generally speaking, an operation that’s in an operating room, and that room is run under positive pressure ventilation, something that, of course, you would never want to have happened if you’re doing an operation on somebody with this kind of virus. And so they talk about switching those kind of patients into negative pressure rooms to do the operation so that you don’t infect other people in the hospital. And so I think it’s an excellent read for physicians, health care providers, who are going to be taking care of these coronavirus or covid-19 patients.
例如,通常来说,如果您正在手术室中进行手术,并且该手术室是在正压通风条件下运行的,那么,如果您要在手术室中进行手术,那当然就不会发生有人感染这种病毒。因此,他们谈论将这类患者转到负压室进行手术,以免感染医院的其他人。因此,对于那些要照顾这些冠状病毒或covid-19患者的医生,卫生保健提供者,我认为这是一本不错的书。
It also talks about when to use n95 masks versus these powered air-purifying respirators, otherwise known as peppers, and who should be wearing them, and talking about, for instance, hot zones, warm zones, and cold zones. Hot zones being in the patient’s room, specifically where there’s negative pressure ventilation; warm zones when you’re outside the patient’s room but still in the Intensive Care Unit; and then finally cold zones when you’re outside of the intensive care unit. So I think this is really important information. And again, we will put a link to it in the description below. Thanks for joining us!
它还讨论了何时使用n95口罩与这些动力式空气净化呼吸器(又称胡椒粉)相比,谁应该佩戴它们,并讨论了例如高温区域,温暖区域和寒冷区域。高温区域位于患者房间内,尤其是负压通风的地方;当您不在患者房间内但仍在重症监护室时,请进入保暖区;当您不在重症监护室外面时,最后是寒冷区域。因此,我认为这是非常重要的信息。同样,我们将在下面的描述中添加一个链接。感谢您加入我们!




Add comment