Sharing Ventilators, More on Sleep, Immunity, & COVID-19 Prevention (Lecture 45)
共享呼吸机,更多关于睡眠,免疫和COVID-19预防的知识(第45讲)
Welcome to another MedCram covid-19 update. Now for the first time, the US tops the charts at 85653 infections that are confirmed, staggering 24,000 total deaths. Daily new cases in the United States are continuing to rise, and if we look at total cases in the United States, the state of New York tops that list by a large amount.
MedCram.com。欢迎来到MedCram covid-19的另一个更新。现在,美国首次名列榜首,确诊85653感染病例,死亡总数达到24,000例。美国的每日新病例持续增长,如果我们看一下美国的总病例数,纽约州位列第一。
It is the epicenter of the new cases at this point because supplies are running scarce. There’s an article in the New York Times talking about the scarcity of mechanical ventilators. New York starts sharing ventilators, and this was approved by the governor. To keep coronavirus patient’s breathing, hospitals pioneer a little tested method. You can see there a portable ventilator that ambulances use to transport patients who are on ventilators.
此时,纽约州是新增病例的爆发中心,因此,医疗设备供应短缺。 《纽约时报》上有一篇文章谈到了机械呼吸机的稀缺,纽约开始共用呼吸机。这是由州长批准的,为保障冠状病毒患者呼吸,医院可以率先使用几乎未经测试的方法。您可以在这看到一台便携式呼吸机,救护车用这种呼吸机运送患者。
They mention here that this is not the first time that this has happened. Before they did this in Las Vegas when there was a mass shooting. In previous updates here on MedCram, we showed you Dr. Babcock, the ER physician, demonstrating that in a video on YouTube.
他们在这里提到这不是第一次发生这种情况。之前他们在拉斯维加斯大规模枪击现场发生过。在MedCram上的先前更新中,我们向您介绍了急诊医师Babcock博士在YouTube视频中演示过如何使用。
Also in the news and updated about six hours ago was a story on Fox by Prisma Health that says that their new innovative ventilator adaptor can actually treat up to four patients on a ventilator at a time. It was another ER physician named Sarah Ferris and her husband who is a software engineer developed this device called Vesper as it turns out this is a 3D-printed device and they are making it available so that it can be printed in your local hospital.
另外在新闻中,大约六个小时前进行了更新,Prisma Health在Fox上发表了一篇报道,说他们改进的新型创新呼吸机实际上一次可以治疗多达四名患者。这是另一位名为Sarah Ferris的急诊医师和她的软件工程师丈夫,开发了这种称为Vesper的设备,是一种3D打印设备,他们正在推广使用该设备,以便可以在您当地的医院打印。
In addition to this, the US Food and Drug Administration has granted emergency use authorization for this type of ventilator, and down here you can see a link other hospitals that want to begin using Vsepr can receive the free source code and printing specifications for the device today by registering on Prisma Health website and you can see it there.
除此之外,美国食品药品监督管理局(US Food and Drug Administration)已授予此类呼吸机的紧急使用授权,在这里您可以看到其他想要开始使用Vsepr的医院的链接,可以获取该设备的免费源代码和打印规范。今天通过在Prisma Health网站上注册,您可以在那里看到它。
Okay, so not so fast because there is a joint statement that was put out by the American Association for Respiratory Care in conjunction with a number of other societies, which are pretty heavy-hitting like the society for Critical Care Medicine issued a joint statement basically saying no, we don’t think that this is a good idea. The reasons they include here are quite numerous, including the fact that volumes could go to the most compliant lung segments that it would be impossible to manage the positive end-expiratory pressure among other things. And you can read some of the others and they give references as well in this joint statement.
好的,不要那么快,因为美国呼吸护理协会与许多其它协会发表了一份联合声明,这些协会的影响很大,就像重症医学会发表联合声明,基本上对这个做法说不,我们认为这不是一个好主意。他们在此提出的原因很多,其中包括以下事实:大量气体可能流向最顺应的肺段,除其他事项外,不可能管理呼气末正压。大家可以阅读其它一些原因,这份联合声明中他们也提到在哪里去查找。
So it’s going to be interesting to see what happens because as the New York Times pointed out ‘The Other Option Is Death. The AARC, however, is saying that it could jeopardize both patients on the ventilator. I think, regardless of which way you take it, it’ll be clear that there’ll be people taking care of people on ventilators that aren’t used to taking care of people on ventilators.
因此,了解一下实际情况会很有趣,因为正如《纽约时报》发表了一篇题为“另一个方法就是死亡”的文章。但是,AARC表示共用呼吸机可能会危及呼吸机上的两名患者。我认为,不管采取哪种方式,很明显,会有人照顾呼吸机上的人,而他们并不习惯于照顾呼吸机上的人。
If you or if you know somebody that’s going to be taking care of somebody on the ventilator, we wanted to offer this course as a refresher on mechanical ventilation.
如果您或您知道有人要照顾呼吸机上的某人,我们希望提供关于机械呼吸的进修课程。
Okay, I wanted to continue our discussion with improving immunity. We talked before about the beneficial effects of an elevated body temperature with respect to killing infections in the virus, and we are going to move on to other things, but I wanted to restate and reunderline the importance of rest and sleep in terms of the activation of the immune system, especially at a time like now where people are very concerned they may not be getting enough sleep. It’s important for us to not underestimate the benefits of sleep.
好的,我想继续讨论提高免疫力。之前我们谈到了升高体温对杀死病毒感染的有益作用,我们将继续探讨其它事情,但是我想重申一下,并强调休息和睡眠在激活人体免疫系统方面的重要性,特别是在像现在这样的时候,人们非常担心自己可能睡眠不足。对我们来说重要的是,不要低估睡眠的好处。
Now, we’re just going to review a little bit. But if you want to know more in detail, go back to update 17 on the coronavirus that we’ve done. But real briefly, this was a study that looked at the effects of sleep deprivation on response to immunization.
现在,我们将要回顾一下。但是,如果您想了解更多详细信息,请返回我们已经完成的关于冠状病毒的更新17。我简短介绍一下,这是一项研究睡眠剥夺对免疫反应的影响。
The participants were sleep-deprived and given a vaccine to the influenza virus. And those that were not sleep-deprived had a much better immune response in terms of antibodies to the vaccine, and the conclusions that the authors drew were these results indicate that the response to the influenza vaccination is likely to be impaired in individuals who suffer from chronic partial sleep restriction because adults who show poor responses to vaccines and other antigenic challenges also experience higher rates of clinical illness. Our findings support the concept that adequate amounts of sleep are needed to maintain resistance to an infectious challenge such as COVID-19.
参与者被剥夺睡眠,并接种了流感病毒疫苗。就疫苗的抗体而言,那些没有被剥夺睡眠的人的免疫反应要好得多。作者得出的结论是,这些结果表明,患有慢性睡眠不足的个体对流感疫苗接种的反应可能会受损,因为对疫苗及其它抗原疾病反应不佳的成年人也经历了更高的临床疾病发病率。我们的发现支持这样一个概念,即需要足够的睡眠来保持对传染性疾病(例如COVID-19)的抵抗力。
This is the other study that we looked at in update 17 and it looked at the sleep habits: how long they slept and what was the efficiency of their sleep in terms of 14-day baseline, and then they went ahead and dropped rhinovirus-filled drops into the nasopharynx of these subjects and they waited to see how many of them would develop the common cold symptoms, and what they found was quite astounding.
这是我们在第17版更新中进行的针对睡眠习惯另一项研究。他们睡了多长时间以及以14天基线为基础的睡眠效率如何,然后他们继续进行研究,将鼻病毒填充剂滴入这些受试者的鼻咽,他们等着看其中有多少会出现普通感冒症状,他们发现的结果令人震惊。
They found that those with an average sleep duration of fewer than seven hours were not 10% more or 50% more or even a hundred percent more likely to develop the cold, but actually almost three times more likely to develop a cold. And when they look for confounders, these things could not be explained in terms of differences in pre-challenge virus, specific antibody, demographics, season of the year, body mass, socioeconomic status, psychological variables or health practices.
他们发现,平均睡眠时间少于七个小时的人患感冒的可能性不会高10%或50%甚至100%,而实际上患感冒的可能性却几乎高出三倍。当他们寻找混杂因素时,这些问题无法用病毒、特异性抗体、人口统计学、一年四季、体重、社会经济地位、心理变量或健康习惯的差异来解释。
And so here we have at least for rhinovirus evidence that poor sleep efficiency and shorter sleep duration in the weeks preceding and exposure were associated with lower resistance to the viral illness. But there’s even more research that just came out last year and this is the focus of sleep that I want to look at today.
因此,这里至少对于鼻病毒,我们有证据表明,睡眠效率差及在接触和接触前几周的睡眠时间短与对病毒性疾病的抵抗力较低有关。但是去年还有更多的研究,这就是我今天要讲的关于睡眠的重点。
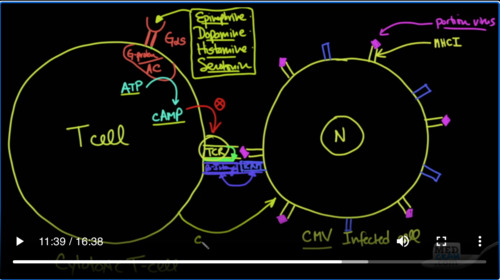
So the first thing you have to understand is that there is a cell, which is infected with a virus. And in this case, it was a CMV infected cell. CMV stands for cytomegalovirus. It’s a common virus that can cause a chronic infection. Here we have the nucleus and because this cell is infected with cytomegalovirus, it makes its normal proteins on the cell surface so that the cells of the immune system would recognize it, but it also puts a little portion of that cytomegalovirus protein out on the surface to let the immune cells know that it’s an infected cell.
因此,大家首先要了解的是,有一个细胞被病毒感染。在这种情况下,它是被CMV感染的细胞。 CMV代表巨细胞病毒。这是一种常见的病毒,可以引起慢性感染。在这里,我们有细胞核,并且由于该细胞感染了巨细胞病毒,因此它会在细胞表面形成其正常蛋白质,从而使免疫系统的细胞能够识别它,但是也会将巨细胞病毒蛋白质的一小部分放到表面让免疫细胞知道它是被感染的细胞。
And so these regular proteins that are made in the cell are known as ICAM. That’s not that important to understand, but that’s the name of the protein. This here is a portion of the virus that lets the immune system know that it is in fact an infected cell. There are other proteins that are also on the cell and these proteins help immune cells dock with them so that they can make the appropriate determination of whether or not this cell should be destroyed or should survive, and this protein is known as ICAM-I C A M.
因此,这些在细胞中产生的常规蛋白质被称为ICAM。这个并不重要,但这就是蛋白质的名称。这是病毒的一部分,它使免疫系统知道它实际上是被感染的细胞。细胞上还有其他蛋白质,这些蛋白质帮助免疫细胞与它们对接,以便它们可以确定该细胞是应被消灭还是让它活下来,这种蛋白质被称为ICAM-ICA M.
So far so good. Now let’s bring in our immune cell. It’s our cytotoxic T-cell. It’s responsible for going around and making sure that cells are not infected and taking care of cells that are infected and this would be the cells that would be going around and getting rid of coronavirus infected cells, so they don’t produce more virus to infect more cells. And in fact, if this can be done early in the course, you would have a limited disease and it wouldn’t lead to many many cells being infected, causing many T cells to have to try to fight and causing that cytokine storm.
到目前为止, 一切顺利。现在让我们引入免疫细胞。这是我们的细胞毒性T细胞。它负责四处巡视并确保细胞不被感染,并照顾被感染的细胞,这将是会四处巡视并摆脱冠状病毒感染的细胞,因此它们不会产生更多的病毒来感染更多的细胞。实际上,如果可以在病程中尽早做到这一点,病情就不会加剧,也不会导致许多细胞被感染,从而导致许多T细胞不得不努力抵抗并引起细胞因子风暴。
Well, there’s a couple of proteins on these T cells. So this is a T-cell and it’s a cytotoxic T-cell, not toxic to you but cytotoxic to the cell that’s infected. These are actually your friends. So there is a receptor on the T cell that sees that little particle of the virus and understands that this cell needs to be destroyed and that is called the T Cell receptor or the TCR.
注意,这些T细胞上有两种蛋白质。这是一个T细胞,它是一种细胞毒性T细胞,对你没有毒性,但对被感染的细胞具有细胞毒性。这些实际上是你的朋友。因此,T细胞上有一个受体,可以看到很小的病毒颗粒,并且知道该细胞需要被消灭,这就叫作T细胞受体或TCR。
The TCR also activates right next to it and I’ll show this here in green that it’s activating the beta integrin. This interaction between beta integrins and the ICAMs allows for a very strong docking that allows these cells to bind very very strongly to these infected cells and that allows these T cells to secrete cytokines that will shut down and kill the cell before it produces more viruses.
TCR也在其旁边激活,我将在此处以绿色显示它正在激活β整合素。β整合素与ICAM之间的这种相互作用可实现非常强的对接作用,从而使这些细胞非常牢固地与这些被感染的细胞结合,并使这些T细胞分泌细胞因子,这些因子会在产生更多病毒之前关闭并杀死该细胞。
So it’s very important that the beta integrins and the ICAMs are able to bind together. Normally, the beta integrins are not activated and they will not bind these ICAMs. Otherwise, your immune system would start to destroy your own body. So they’re shut down, but there are certain situations where they need to be turned on and, if they are not turned on, your immune system is not going to work very well.
因此,β整合素和ICAM能够结合在一起非常重要。通常,β整合素不会被激活,并且它们不会结合这些ICAM。否则,你的免疫系统将开始破坏自己的身体。因此,它们被关闭,但在某些情况下需要将其打开,如果未打开,则您的免疫系统将无法很好地发挥作用。
Well, in this case, it is the TCR that activates these beta integrins and allows this to occur. The purpose of this article was to see whether or not things can affect this turning on of the beta integrins and sure enough, they discovered that there is a receptor called the G alpha S receptor, and this receptor is coupled to what is known as a g-protein. And it’s coupled to an enzyme known as adenylate cyclase.
在这种情况下,正是TCR激活了这些β整合素并使其发生。本文的目的是了解β整合素的这种开启是否会受到影响,他们确实发现了一种叫做G alpha S的受体,该受体与所谓的ag蛋白结合,它与腺苷酸环化酶结合。
There’s a lot of moving parts to this receptor, but I’m going to simplify it and show you that essentially it takes ATP, which is abundant in the cell, and it converts it into something called cyclic AMP and as it turns out cyclic AMP shuts down the ability of the TCR to activate the beta integrase. So the question is what is actually stimulating this G alpha S receptor.
该受体有很多运动部件,但我将对其进行简化,并向大家展示,它实际上吸收了细胞中丰富的ATP,并将其转换为称为循环AMP的物质,结果证明是循环AMP关闭了TCR激活β整合酶的能力。因此,问题是什么实际上在刺激该G alpha S受体。
There are a number of things that can activate this. One of them is epinephrine, typically dopamine, histamine, serotonin. And the thing about all of these things that can actually stimulate this receptor here. They’re all quite elevated when you are awake, and so you can see it’s possible that epinephrine, dopamine, histamine, and serotonin could stimulate this receptor, which would eventually convert ATP into cyclic AMP, which would then inhibit TCR‘s ability to have the beta integrin bind with ICAM and to have this T-cell destroy with cytokines this infected cell.
有很多东西可以激活它。其中之一是肾上腺素,通常是多巴胺,组胺,5-羟色胺。而所有这些事情实际上可以刺激此受体。当您醒着时,它们都非常升高,因此您可以看到肾上腺素,多巴胺,组胺和5-羟色胺可能会刺激该受体,最终将ATP转化为环状AMP,从而抑制TCR的抗癌能力。 β整联蛋白与ICAM结合,并使该T细胞通过细胞因子破坏该感染的细胞。
So it is possible that sleep could stop epinephrine, dopamine, histamine and serotonin from binding this receptor and allow the beta integrin and the ICAM to bind tightly so that the immune response would be more robust.
因此,睡眠可能会阻止肾上腺素,多巴胺,组胺和5-羟色胺与该受体的结合,并使β整联蛋白和ICAM紧密结合,从而使免疫反应更加牢固。
And so now the title becomes a little bit more understandable—Gas coupled receptor signaling and sleep regulate integrand activation of human antigen-specific T-cells—and this was published last year in the Journal of Experimental Medicine. They infected these with the Epstein-Barr virus as well. And so we’ve got data for both of those.
现在,标题“Gas结合的受体信号传导及睡眠调节抗原特定T细胞的整合物激活”变得更加容易理解,这篇论文去年在《实验医学杂志》上发表。他们也用爱泼斯坦–巴尔病毒感染这些细胞。这样我们就获得了这两个数据。
So here we can see the data for CMV-specific CD8 cytotoxic T cells. They looked at isoproterenol, which does hit that receptor epinephrine, which does hit the receptor, and norepinephrine as well. Here on the x-axis, as we increase the concentration, you can see that the binding of ICAM one as a percentage of the control starts to drop off precipitously. And you can see that here with prostaglandins, as well as adenosine in the EBV, or the Epstein-Barr virus-cell cultures that were infected as the increased concentration of the same substances that we talked about. You can see that the ICAM does drop.
因此,在这里我们可以看到CMV特异性CD8细胞毒性T细胞的数据。他们研究了异丙肾上腺素和肾上腺素,异丙肾上腺素确实击中了受体肾上腺素,肾上腺素也击中了受体。在x轴上,随着浓度的增加,您会看到,ICAM 1的结合量占对照的百分比开始急剧下降。您会发现在这里前列腺素以及EBV中的腺苷或爱泼斯坦-巴尔病毒细胞培养物被感染时,所谈论的相同物质的浓度增加了。您可以看到ICAM确实下降了。
So it’s one thing to say that these specific substances make it drop, but the question is whether or not sleep is actually beneficial in making sure that the cells can bind to their targets and take them out, and that’s what they attempted to show here in human patients.
可以说这些特定物质会使它降低,但是问题是睡眠是否真正有益于确保细胞能够结合其靶标并将其取出,这就是他们试图要在患者身上展示的。
What we see here again is the same thing on the y-axis. We’re looking at ICAM binding, but we have two types of patients in this scenario. We have the ones that are filled in with black circles. And these were the ones that were sleeping at night and awake during the day as opposed to these Open Circles, which are white in the middle where they’re awake during the night and also awake during the day. And so you can see the effects here in the CMV-infected cells on the left and the EBV infected cells on the right.
我们在这里再次看到的是在y轴上的相同内容。我们正在研究ICAM绑定,但是在这种情况下,我们有两种类型的患者。我们有被黑色圆圈填充的那些。这些是晚上睡觉而白天醒来的,与这些空心圆圈相反,空心圆圈在中间是白色的,它们在晚上醒来,在白天也醒着。因此,您可以在左侧看到CMV感染的细胞,在右侧看到EBV感染的细胞看到的效果。
In the night time, which is shaded here and over here as well, at least at two o’clock in the morning and here at six o’clock in the morning, there was a statistically significant increase in ICAM binding in these patients that were sleeping at two o’clock in the morning as opposed to being awake at 2 o’clock in the morning. And I just wanted to point out for those of you who are doing shift work that, so long as you are working at night and going home and sleeping with your lights off and no light coming in through the windows and you do this every single day throughout the weekend, you can also get the same benefit from getting sleep even though it’s when the sun is up.
在夜间(这里被涂黑,这里也是),至少在凌晨两点及凌晨六点,这些患者的ICAM结合在统计学上显着增加。他们早上两点睡觉,而不是早上两点醒。我只是想为那些倒班工作的人指出,只要您晚上工作,回家,关着灯睡觉,窗户没有光线进入,并且每天都这样(包括周末),即使太阳升起,你也可以从睡眠中获得相同的好处。
And then they decided to look at that over the different types of differentiation of these cytotoxic T cells. They looked at ones that were early in their life, intermediate in the cell life, and late in the cell life. And what they found was these effects seem to be the strongest in the early phase of the cell’s life despite the fact that it didn’t have a lot of these G receptors that we talked about. That might suggest that it’s the early cells that are being amplified against the infection at hand that is more influenced by the effect of sleep versus wake.
然后,他们决定针对这些细胞毒性T细胞的不同分化类型进行研究。他们研究细胞早期,中期和晚期。他们发现这种作用似乎在细胞生命的早期阶段是最强的,尽管我们讲过的这些G受体并不多。这可能表明,针对眼前感染而被扩增的早期细胞更受睡眠与非睡眠作用的影响。
So the conclusions of the authors are this. We show here that several Gas–coupled receptor ligands potently inhibit TCR-mediated integrin activation on antigen-specific CD8+ T cells, (These are the ones that are doing the killing here), whereas sleep-up regulates integrin activation by suppressing Gas–coupled receptor signaling. Given the importance of integrin activation for the formation of immunological synapses, our data suggest a critical role of conditions like sleep that are characterized by low levels of Gas–coupled receptor ligands, in boosting the T-cell responses. And I’ll tell you it’s those T Cell responses that are very important in your immune system getting rid of coronavirus infected cells.
因此,作者的结论是这样的。我们在这里表明,几种Gas结合的受体配基有效抑制TCR介导的整合素在抗原特定的CD8 + T细胞上激活(这些是细胞杀手),而睡眠则通过抑制Gas结合的受体发送信号来调节整合素激活。考虑到整合素激活对于形成免疫突触的重要性,我们的数据表明,像以低水平的Gas结合的受体配基为特征的睡眠条件在增强T细胞反应中起着至关重要的作用。我告诉你们,正是这些T细胞反应对于你的免疫系统摆脱被冠状病毒感染的细胞非常重要。
So you can imagine the current scenario and it doesn’t take a lot of drawing on here to modify this picture for the current Covid-19 situation. Sleep is important and you don’t have to go to the store to buy it and you don’t have to wait for pharmacists to dispense it. It’s something that we can do. Put down your iPads, put down your phones and go to sleep and wake up with a better immune system.
大家可以想象当前的情况,并且无需进行很多描绘就可以针对当前的Covid-19情况修改这张图。睡眠很重要,大家不必去商店购买它,也不必等待药剂师配药。这是我们可以做的。放下你的iPad,放下你的手机,去睡上一觉,带着一个更好的免疫系统醒来。
For those of you who have difficulty sleeping if you have insomnia, we have a free course on how to deal with insomnia. Thanks for joining us.
对于那些因失眠而难以入睡的人,我们提供有关如何处理失眠的免费课程。感谢加入我们。
Word count: 2585




Add comment