Searching for Immunity Boosters & Possible Lessons from Spanish Flu (Lecture 47)
从西班牙流感中寻找免疫增强剂和可能的经验教训(第47讲)
MedCram.com
Welcome to another MedCram COVID-19 update. As the infection continues to grow around the world, the United States continues to lead the world in total cases and the epicenter at this point is clearly in New York.
欢迎来到MedCram COVID-19的另一个更新。随着感染在世界范围内的持续增长,美国在所有病例中继续保持世界领先地位,此时的爆发中心显然在纽约。
Yesterday we looked at data that seemed to imply that hot and cold temperature regulation affected the part of the immune system, namely the innate immune system that helps with targeting viral infections and foreign invaders. And this part of the immune system is particularly affected, especially in the SARS-CoV2 viral infection, specifically natural killer cells and monocytes.
昨天,我们查看了一些数据,这些数据似乎暗示着冷热温度调节会影响免疫系统的一部分,即有助于将目标对准病毒感染和外来入侵者的先天免疫系统。这一部分的免疫系统特别受到影响,尤其是在SARS-CoV2病毒感染中,具体就是自然杀手细胞和单核细胞受到影响。
And we showed some data that hyperthermia and then cooling off actually improved surrogates for the immune system in terms of the number of monocytes and their stimulation and response to foreign invaders.
并且我们显示了一些数据,就单核细胞的数量及其对外来入侵者的刺激和反应而言,高热然后冷却实际上改善了免疫系统的替代指标。
We also took the example of a sauna in terms of some of the data that’s been done in terms of preventing viral infections. But the point was not to advocate specifically for sauna bathing or for anything in particular, but just ways that people’s temperature can be elevated and then reduced. I think the ideal answer to this would be something that could be easily accessible for the majority of the world’s population and certainly, unlike Finland, we can’t all have our own sauna.
我们还以桑拿浴为例说明了在预防病毒感染方面所做的一些数据。但是重点并不是特别提倡桑拿浴或任何其他东西,而只是提倡人们升温然后降温的方法。我认为对此的理想答案是可以让世界上大多数人容易获得的东西,当然,与芬兰不同,我们不可能所有人都拥有自己的桑拿浴室。
And so the purpose of today’s video is really to get some practical solutions that answer the data that we’ve been given. So I encourage you to watch the whole video. Okay. I wanted to review again exactly what it is that’s going on with this coronavirus infection.
因此,今天的视频的目的实际上是获得一些实用的解决方案,以回答我们得到的数据。因此,我鼓励大家观看整个视频。好的。我想再次回顾一下这种冠状病毒感染到底是怎么回事。
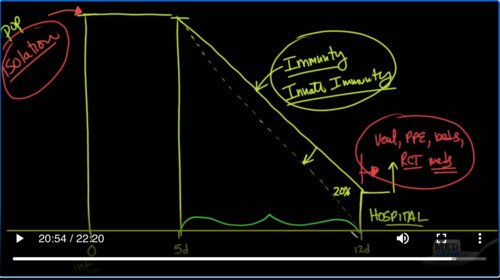
First of all, at day 0, when somebody becomes infected, there’s about a five-day period where there is no symptoms. We call that the incubation period and let’s say that of all the people that become infected, they won’t show signs during those 5 days. And so this is at a hundred percent and then over the next seven to eight days, so by the time we get to day 12, there’s going to be a pretty dramatic drop-off in the number of patients that are going to have issues so that we are down to approximately at this point twenty percent.
首先,在第0天,当有人被感染时,大约有五天的时间没有症状。我们将其称为潜伏期,假设所有被感染的人在这5天内不显示任何迹象。所以这是百分之一百,然后在接下来的七到八天内,所以到了第12天,有症状的患者数量将急剧下降,最终降到大约百分之二十。
And the reason for this drop is really for one reason and that’s the host’s immunity, your immune system. With a start-off at a hundred percent drop down to about 20%, this 20% will need to be hospitalized because of pneumonia shortness of breath, etc. And so they will go into the hospital at this point.
这种下降的原因实际上是一个原因,那就是宿主的免疫力,即你的免疫系统。由于最初的百分率下降到大约20%,这20%的患者将因肺炎呼吸急促等原因而需要住院治疗。因此,他们将在此时入院。
The specific part of your immune system that is really hammering this virus and is the reason why 80% exit the cycle and they don’t need any more care. It seems as though based on the studies that we looked at last time was because of innate immunity and this is the portion of the immune system that is very strong in terms of taking care of these viral pathogens. It is the monocytes. It’s the natural killer cells. Remember in our last video we showed you that these monocytes which should be up here in terms of frequency are actually down here. They are impaired.
你免疫系统的这一特定部分确实会重击该病毒,这就是80%退出该循环且不再需要任何护理的原因。根据上次研究,似乎是由于先天免疫引起的,在照顾这些病毒病原体方面,这是免疫系统中非常重要的部分。它是单核细胞。这是自然的杀手细胞。请记住,在我们的上一个视频中,我们展示了本来在频率上位于这个地方的单核细胞实际上降到这里了。他们被损坏了。
We also showed you in this article “The longer incubation period is probably due to their immune evasion properties, efficiently escaping host immune detection at the early stage of the infection.” And that has to do with again these monocytes and part of the innate immunity. Look back at our last update for more information on that.
我们介绍了这篇论文。“更长的潜伏期可能是由于它们的免疫逃逸特性,在感染的早期有效逃避了宿主免疫检测。”这又与这些单核细胞和这部分先天免疫有关。回顾一下我们的最新更新,以获取更多信息。
We also showed how temperature, both hot and cold, could actually enhance this immunity and the question is whether or not we could figure out how to improve immunity. We could shift this curve down and actually have less needing to have hospitalization. Well, as it turns out COVID-19 is not the only disease that requires monocytes as the key player in the fighting of its infection.
我们还展示了温度(无论冷热)实际上如何都能增强这种免疫力,问题是我们是否可以弄清楚如何提高免疫力。我们可以将此曲线向下移动,实际上不需要住院。事实证明,COVID-19并不是唯一需要单核细胞作为抵抗其感染的关键因素的疾病。
Here’s a paper that was published less than a year ago in Frontiers in Immunology. They go through and they actually note “these results demonstrate for the first time that intermediate monocytes control the differentiation of Treg subsets in Treponema pallidum/HIV-1 co-infections. New insights into an immunological mechanism involving monocytes and Tregs in HIV-infected individuals with syphilis.”
这是不到一年前发表在《免疫学前沿》的论文。他们实际上指出这些结果首次证明,中间单核细胞可控制苍白密螺旋体/ HIV-1共感染中Treg亚群的分化。这篇论文对单核细胞和Treg在携带梅毒的艾滋病感染者身上的免疫作用提供了新见解。
So the key here I want you to see is that there is an association with monocytes with syphilis and that’s very interesting because as we showed last time “Human monocyte stimulation by experimental whole body hypothermia” was augmented and we could see here that “three hours after in vivo hyperthermia, the response of monocytes was enhanced.” But this shouldn’t come as a surprise to anyone who knows the history of the treatment of neurosyphilis as we know now, but they didn’t know then monocytes are involved with the treatment of neurosyphilis and also syphilis.
因此,我想让你们看到的关键是,梅毒与单核细胞有关,这很有趣,因为正如我们上次展示的那样,“实验性全身低温对人单核细胞的刺激增加了”,我们可以看到“三个小时体内热疗后,单核细胞的反应增强了。”但是,这对于任何我们现在知道的神经梅毒治疗历史的人来说都不应该感到惊讶,但是他们当时不知道单核细胞会参与神经梅毒和梅毒的治疗。
And if we look here there was a physician by the name of Julia’s Wagner-Jauregg. And what he found interestingly is that by stimulating the body to make a fever actually sped up the treatment of neurosyphilis. Well, how did he cause the patient to actually have a fever? By infecting him with malaria. Now, of course, we’re not advocating to infect people with malaria. Remember this was before penicillin and as it’s noted here in the article. They say “actually malaria infection was an acceptable risk for the patients, as quinine would be administered as soon as the syphilis was cured.”
我们来看一下,有一位名叫朱莉娅·瓦格纳·雅鲁格的医生。有趣的是他发现,通过刺激身体发烧实际上加速了神经梅毒的治疗。那么,他是如何导致患者发烧的呢?通过用疟疾感染他。当然,现在,我们不主张用疟疾感染患者。请记住,这是在青霉素之前,正如本文在此处所述。他们说:“实际上,疟疾感染对患者来说是可以接受的风险,因为梅毒一旦治愈就将立即服用奎宁。”
They also mentioned interestingly that “for centuries heat has been used in various ways for the cure of mental diseases and even Hippocrates noted that malarial fever could have a calming effect in epileptics. It should also be noted that Dr. Wagner-Jauregg received for his work in terms of treating neurosyphilis the Nobel Prize in medicine.
他们还有趣地提到:“几个世纪以来,人们一直在以多种方式使用热来治疗精神疾病,甚至希波克拉底也指出,疟疾热可能会使癫痫病患者镇静。另外,瓦格纳医生因在治疗神经梅毒方面的工作获得了诺贝尔医学奖。
Now interestingly the article goes on to show that the therapeutic regimen that was completed with the administration of quinine sulphate to terminate the malarial infection was done in the hospital under strict monitoring of patients‘ vital signs. And there’s a number of ways of actually causing the patient to have a fever. They talked about the injection of foreign protein, parasitic diseases, chemical substances. But it’s interesting what they end up on here, which is immersion of the individual in a hot bath or placing them in a heat cabinet. And this was used well into the 1950s.
现在,有趣的是,该文章继续表明,在严格监测患者生命体征的情况下,在医院中完成了用硫酸奎宁治疗终止疟疾感染的治疗方案。实际上有多种方法可以使患者发烧。他们讨论了外来蛋白质,寄生虫疾病,化学物质的注射。但是有趣的是,他们最后谈到热水浴或加热柜的方法,这种方法一直用到二十世纪五十年代。
However, with the introduction of penicillin in syphilis treatment, fever therapy effectively ended because now we had an antibiotic. And so one has to realize here that there was a major change in the way we did medicine in the United States and in the world instead of doing home remedies or these other things that were done as mentioned in this article.
但是,随着青霉素的引入治疗梅毒,发烧疗法实际上终止了,因为现在我们有了抗生素。因此,人们必须在这里意识到,我们在美国和世界范围内治疗方式发生了重大变化,而不是像本文所述的那样进行家庭疗法或其它方法。
We went down a road of randomized placebo-controlled trials that were funded by companies that were able to make medications, not to say there was anything wrong with that because we’ve certainly derived the benefit in the last 50 to 60 years in this department. But the question is what’s happened to some of these other potential treatments and are any of these other treatments worthy of looking at once again?
我们走了由能够制造药物的公司资助的随机安慰剂对照试验之路,并不是说这有什么不对,因为我们当然已经在该部门获得了过去50至60年的收益。但是问题是,其它一些潜在的治疗方法又发生了什么,这些其它治疗方法中的任何一种值得再次关注吗?
Remember our timeline. When a patient has symptoms at five days and goes to the emergency room, what is told to him is for him to go back home because he doesn’t meet the admission criteria to go in the hospital. Meanwhile, the virus is making inroads on the patient and is suppressing the immune system until finally the house is fully inflamed and the patient is admitted to the hospital with pneumonia.
记住我们的时间表。当患者五天后出现症状并去急诊室时,告诉他要回家,因为他不符合住院标准。同时,病毒正在侵入患者体内并抑制免疫系统,直到最终完全发展成肺炎才能入院。
And what we’ve been doing up to this point for Covid-19 in this country is we’ve been trying to improve and increase the resources at the hospital in terms of ventilators, in terms of rooms, in terms of medications and in terms of staffing to meet that demand of 20% who will eventually need to be hospitalized.
到目前为止,我国针对Covid-19所做的工作就是尝试改善和增加医院在呼吸机,病房,药物和人员方面的资源来满足20%最终需要住院的需求。
And the question that remains is there‘s some simple remedy that could be investigated that would be available in someone’s home, that they wouldn’t have to go to the store to buy, that a production company wouldn’t have to deliver. Is there something simple enough that can reduce this curve enough to bring down the demand at the hospital and prevent this overwhelming tsunami of patients that require health care delivery.
接下来的问题是,有一些简单的疗法,可以在某人的家中使用,他们不必去商店购买,也不需要公司送货。有没有足够简单的方法可以降低这条曲线,从而降低住院需求并防止需要医疗服务的患者海啸发生。
So this statement here where it was used well into the 1950s intrigued me. So I decided based on the internet and all of the archives that we have available to us to dig down deeper and figure this out.
这个方法一直用到二十世纪五十年代,这引起了我的兴趣。因此,我决定基于互联网和所有可用的档案库,对此进行更深入的研究并找出答案。
So there’s probably no more illustrious character in the history of hydrotherapy than John Harvey Kellogg. This physician wasn’t the inventor of hydrotherapy, but he was certainly its most ardent advocate.
因此,在水疗史上,没有比约翰·哈维·凯洛格(John Harvey Kellogg)更杰出的人物了。这位医生不是水疗法的发明者,但他无疑是水疗法的最热情的拥护者。
He also is the one that invented Kellogg’s Corn Flakes. His brother was the entrepreneur who started the business. He wanted to change breakfast in the morning because of what people were eating at the time. It was all eggs and ham and he was a health advocate.
他也是Kellogg玉米片的发明人。他的兄弟是企业家,开创了这个生意。当时人们早上都吃鸡蛋和火腿,他想改变早餐,他是健康倡导者。
As an interesting side note, one of the people that visited him at the Battle Creek Sanitarium, where he was presiding, was a man by the name of Post, who took the idea and erected his history.
有趣的是,有一个叫波斯特(Post)人在他主持的巴特尔克里克疗养院里拜访过他,这个人拿走了他的想法并树立了自己的历史。
He actually was the doctor to many famous patients, including President William Howard Taft. And you can see the rest of the list there, including Henry Ford and Thomas Edison.
他实际上是许多著名患者的医生,包括总统威廉·霍华德·塔夫脱(William Howard Taft)。大家可以在此处看到列表的其余部分,包括亨利·福特和托马斯·爱迪生。
He wrote a 1500 page compendium on rational hydrotherapy and the technique of their application in the treatment of disease. And I show this to illustrate a couple of things. Number one: just how quickly treatment can completely be obsolete and not practiced in most hospitals in the United States today, hydrotherapy is not used at all in terms of an infectious disease standpoint.
他撰写了1500页的关于合理水疗及其在疾病治疗中应用的纲要。我通过展示来说明一些事情。第一:今天在美国大多数医院中,治疗方法淘汰得多快,就传染病的观点而言,水疗法根本没有被使用。
One must realize that this book was published decades before the discovery of penicillin and antibiotics. And so from an infectious disease standpoint, the randomized placebo-controlled trial in terms of medications that can treat and prophylaxis against infections has been the way that we have gone in the last hundred years. And of course specifically the issue with Covid-19 is we have no randomized placebo-controlled trials at this point.
必须意识到这本书是在发现青霉素和抗生素之前数十年出版的。因此,从传染病的角度来看,在过去的一百年里,关于可以治疗和预防感染的药物进行的随机安慰剂对照试验一直是我们走过的路。当然,特别是Covid-19的问题,目前我们尚无随机的安慰剂对照试验。
The other point that this brings up is to clarify and to show what the state of affairs were in the other denominational sanitariums that were sister sanitariums of the Battle Creek Sanitarium at this time. So when we come back to our initial issue here of trying to bring down this curve, we are left with this situation after 1950. We have a world where we live in randomized placebo-controlled trials, and we’re able to compare. Prior to 1950, we do not have that very often.
提出的另一点是要澄清并表明当时作为巴特尔克里克疗养院的姐妹疗养院的其它宗派疗养院的状况。因此,当我们回到试图降低此曲线的最初问题时,在1950年之后我们就处于这种情况。我们有一个生活在随机安慰剂对照试验中的世界,我们可以进行比较。在1950年之前,我们没有那么频繁。
Typically, there is physicians that are practicing based on observation, based on anecdotal evidence. Because of the drop of hydrothermal therapy from the scene prior to 1950, it is going to be very difficult to find a randomized controlled trial looking at hydrotherapy in a population base where we have people who are infected and are being treated. We have already shown in this update and in the last update some interesting findings that are surrogates in most cases and in some cases mild viral infections of little consequence like colds.
通常,有医生根据观察和轶事证据行医。由于1950年之前热液疗法的兴起,很难找到一个随机对照试验来研究一个有人口感染和正在接受治疗的人群中的水疗。我们已经在此更新中和在最后更新中显示了一些有趣的发现,这些发现在大多数情况下是替代的,在某些情况下是轻度病毒感染,其后果不明显,例如感冒。
The question of course is: can hydrotherapy or hydrothermal therapy or temperature regulation affect Covid-19 in any way, shape or form? And unfortunately, I don’t think we’ll ever have that answer. What we can do is we can look at next best scenarios, and that’s what we attempt to do next.
当然,问题是水疗或水热疗法或温度调节会以任何方式影响Covid-19吗?不幸的是,我认为我们永远不会得到这个答案。我们可以做的是,我们可以研究下一个最佳方案,这就是我们接下来要尝试的方案。
So this is by no means a medical journal. In fact, it is a religious periodical published by the review and herald publishing company. But in its 1919 edition, there is an article written by Doctor Ruble, who is the medical director of the New England Sanitarium in Massachusetts.
因此,这绝不是医学期刊。实际上,这是由评论和先驱出版公司出版的宗教期刊。但是在1919年版中,有一篇由马萨诸塞州新英格兰疗养院的医学主任卢布医生撰写的文章。
So this is what Dr. Ruble had to say in the height of the Spanish Flu pandemic in the northeast of the United States. He says here that the infecting agent of influenza, whether germ or virus, has not yet been identified, and there is no laboratory method by which it can be differentiated from a common cold, or bronchitis, or other inflammation of the respiratory tract. Remember that Doctor Ruble is writing this prior to the discovery of DNA, prior to the electron microscope.
这就是卢布医生在美国东北部西班牙流感大流行中的发言。他在这里说,还没有发现流感的病原体,无论是细菌还是病毒,而且还没有实验室方法可以将其与普通感冒,支气管炎或其它呼吸道炎症区分开。请记住,卢布医生是在发现DNA之前,在电子显微镜之前写这篇文章的。
And I find that his insights are quite valuable. “The following are the principal methods of prevention: First, isolation of those who have symptoms of the disease from those who are well. Second, inoculation seems to have good effect in some cases, but its value is questionable. Third, each person should keep as well as possible, by proper habits of eating, drinking, sleeping, exercising, and breathing.“
而且我发现他的见解非常有价值。“以下是预防的主要方法:首先,将那些有疾病症状的人与身体健康的人隔离开。第二,接种在某些情况下似乎有很好的效果,但其价值值得怀疑。第三,每个人都应该保持适当的饮食,饮水,睡眠,运动和呼吸习惯。”
It’s interesting that even at that time they knew that sleeping was important. “An important matter in treating the disease is to protect the patient from exposure, especially immediately following the cessation of abnormal temperature. Every subject of the disease should remain in bed as many days after the temperature becomes normal as he had a temperature, in order to be sure to avoid a recurrence of a possible pneumonia.” And then he goes on to talk about in the Boston Medical Journal millions of people that this influenza virus has taken around the world.
有趣的是,即使在那时,他们都知道睡觉很重要。“治疗该疾病的重要事项是保护患者免于暴露,尤其是在异常体温停止后立即暴露。在体温恢复正常后的每一天,该疾病的每个患者都应躺在床上,以确保其体温正常,确保避免可能的肺炎复发。”然后他继续在《波士顿医学杂志》上谈论这种流感病毒在全球范围内已感染的数百万人。
And I want you to be understanding of a certain point. In these days, there was no intensive care units. There were no ventilators. There were no ICU nurses. There were no intensivists. And so if you’d got pneumonia, you had about a 50/50 chance of making it. The entire treatment at this point was to prevent you from getting the pneumonia.
我希望你们能理解某一点。在这些日子里,没有重症监护室,没有呼吸机,没有ICU护士。没有强化器。因此,如果你得了肺炎,你大约有50/50的机会活下来。此时的整个治疗是防止得肺炎。
I find that an interesting dichotomy because today if you go to the emergency room, they will tell you not to come back until you do have a pneumonia, and then they can treat you with antibiotics, with an intensive care nurse, with a respiratory therapist and, if needed, a ventilator.
我发现这是一个有趣的矛盾,因为今天如果你去急诊室,他们会告诉你等到你得了肺炎后再来,然后他们可以用抗生素,重症监护护士和呼吸治疗师来治疗,如果需要,还可以使用呼吸机。
The next part of Dr. Ruble’s treaties is talking about the sanitarium treatment of influenza, which I find very interesting. So what Dr. Ruble describes is two situations: the situation in the Army Camps and the situation in the sanitariums in New England. And so the Army Camps, remember that these were soldiers coming back from the first world war and bringing with them unfortunately the Spanish flu epidemic, which became the pandemic.
卢布医生条约的下一部分讨论的是流感的疗养院治疗,我发现这很有趣。卢布医生描述的是两种情况:陆军营地的情况和新英格兰的疗养院的情况。在军营中,请记住,这些士兵是第一次世界大战后回来的士兵,不幸的是,他们带来了西班牙流感,后来变成大流行病。
Now Doctor Ruble doesn’t report the actual number of cases, but he does have percentages, so we don’t know the number of cases, but we do know that about 20% of the soldiers coming back in the Army Camps came down with the influenza virus.
卢布医生没有报告实际病例数,但是他有百分比报告,因此我们不知道病例数,但是我们知道,回到陆军营地的士兵中约有20%死于流感病毒。
Those translated into cases of pneumonia (about 16%). They said about one in six. And then from there, there was about a 40 percent conversion rate into deaths, which gives us a total of about six point four percent case fatality rate for the Army Camps.
那些转化为肺炎病例(约16%)。他们说大约六分之一。然后从那里大约有40%的死亡转化率,这使我们军营的病死率总计达到大约6.4%。
But over in the sanitariums, they were able to treat the inpatients with the hydrotherapy, but they’re also able to treat outpatients. There was nothing special about being inpatient. And they try to match the treatment with the outpatients.
但是在疗养院里,他们能够通过水疗来治疗住院病人,但是他们也能够治疗门诊病人。住院没有什么特别的。并且他们尽量使治疗与门诊病人匹配。
Remember, this is the time where they didn’t have ICU beds. There was no ventilators. There was no ICU nurses. So a lot of the treatment could be done both in and outpatients at the same time. However, the outpatients may have differed a little bit from the inpatients in that they may have waited a little bit longer to be treated, whereas those in the inpatient side were treated immediately.
请记住,那时候他们没有ICU病床,没有呼吸机,没有加护病房护士。因此,很多治疗可能对住院和门诊病人同时进行。但是,门诊病人可能与住院病人有所不同,因为他们可能要等待更长的时间才能接受治疗,而住院病人则立即接受治疗。
So on the outpatient side, they recorded 677 patients, of which 55 cases got pneumonia and that was about eight percent and then those 55, 26 of them died, which worked out to about 3.8 percent mortality. Now the inpatient side: these patients were being treated in the sanitariums and these might have been more likely to be the doctors, the nurses who came down with symptoms in the sanitarium and they knew what to do and they started therapy right away.
因此,在门诊方面,他们记录了677名患者,其中55例患有肺炎,约占8%,然后55例中有26例死亡,占死亡率的3.8%。住院方面:这些患者正在疗养院接受治疗,而这些患者更有可能是在疗养院染病的医生、护士,他们知道该怎么办并立即开始治疗。
So those had about 446, which led to 11 cases of pneumonia, which is about two percent and that led to six that died, which was giving us a total mortality of about 1.3 percent. So of the 55 that went to 26 here in the outpatient, that was about 47 percent, and of the 11 here, six went to deaths. That’s about 55 percent.
因此,这些患者约有446人,导致11例肺炎,约占2%,导致6例死亡,这使我们的总死亡率约为1.3%。因此,在门诊的55名患者中,有26名门诊患者,占47%;这有11名患者,6例死亡,大约占55%。
So how would I interpret these results? Well, the first thing that I notice is in the army camp versus the sanitarium. The army camp would be where I would expect the best physicians, the best technique and the best ancillary services, and for those patients that developed pneumonia, you can see here that the Army had the best outcomes.
那么我将如何解释这些结果?我注意到的第一件事是军队营地和疗养院对比。我认为在军队营地有最好的医生,最好的技术和最好的辅助服务,对于那些患有肺炎的患者,你们可以在这里看到军队取得了最佳的效果。
However, how many actually developed pneumonia in this case? 16% develop pneumonia in the army camp, 8% as an outpatient and 2% as an inpatient. You can see that the hydrotherapy or hydrothermal therapy, because they used hot and cold, was the best at reducing the incidence of pneumonia.
但是,在这种情况下实际有多少人患上肺炎?军队营地中有16%患上肺炎,门诊病人中有8%,住院病人中有2%。你们会看到,水疗法或水热疗法(冷热疗法),最能减少肺炎的发生。
And you’ve got to remember that in this day and age pneumonia was a death sentence pretty much and so everything was done to prevent the patient from getting pneumonia. You remember what Dr. Ruble said about making sure that the patient laid in bed and still so that they wouldn’t get the secondary infections that cause pneumonia.
你们要记住,在当时,肺炎几乎是一种死刑,所以会尽一切努力防止患者患上肺炎。大家还记得卢布(Ruble)医生所说的确保患者卧床静养,以免他们被二次感染,引发肺炎。
Remember this was before antibiotics and you can see when this approach was taken that the best mortality rate was patients that were treated for early in the sanitarium, when they knew they would be treating them exactly according to the protocol. Second best was when they trained the facilities at home to take care of the patient and then worst is when they weren’t doing the hydrotherapy and presumably these cases led extensively to a lot of pneumonia, which led to an excess case fatality rates.
请记住,这是在抗生素出现之前。大家会看到采用这种方法时,在疗养院早期接受治疗的患者死亡率最低,他们知道医生会严格按照治疗方案进行治疗;死亡率第二低的是在家里有受过训练的人来照顾病人时;死亡率最高的是当他们没有进行水疗时,大概这些病例导致了很多肺炎,从而导致病死率过高。
So that kind of brings us back to our graph and here we have the population. And what we’re trying to do is isolate, which is trying to prevent the number of people from getting infected, which is represented here by this first bar.
让我们回来看我们的图表,看一下人口。我们试图做的是隔离,这是为了防止这些人被感染,这在第一个柱形条上显示出来了。
Then we have symptoms and there’s about twenty percent of these people who are infected, which will end up at the hospital and what we’re trying to do there is increase the capacity at the hospital by getting ventilators, by making sure that our health care workers have personal protective equipment, by getting more beds, by getting nurses and respiratory therapist and ancillary services ramped up.
然后我们看到现症状,其中约有20%的人被感染,最终将被送往医院,而我们正在尝试做的是通过获得呼吸机、确保我们的医疗保健工人拥有个人防护设备、增加床铺、增加护士,呼吸治疗师和辅助服务来提高医院的接纳能力。
But also we are doing randomized control trial, so we can have medications to treat people with. So we’re working a lot here at this end and that happens only when the patient comes to the hospital after they have shortness of breath and pneumonia. And we’re doing a lot here at this end to make sure that only a small portion of the population actually gets the infection and I think those are all important things that we should do.
但是我们也在进行随机对照试验,以便我们可以用药物治疗。因此,我们在这里为此付出了很多努力,只有在患者出现呼吸急促和肺炎之后才去医院就可以了。为此,我们在这里做了很多工作,以确保只有一小部分人口实际上感染了病毒,我认为这些都是我们应该做的重要事情。
But when the patient comes to the emergency room here and is told to go home and not come back unless they have symptoms of shortness of breath. We are doing a lot of nothing in this period of time here when the immune system I believe needs help. And remember here if we have a situation where 80% of the people who get the infection are going to do well and it’s this 20 percent that needs to come to the hospital.
但是,当病人来到这里的急诊室并被告知要回家且除非他们有呼吸急促的症状,否则不要回来。在我认为免疫系统需要帮助的这段时间内,我们在此期间无所作为。请记住,如果我们遇到这样的情况,即80%的感染者会好起来,而就这20%的人需要去医院。
If we can just improve that immune function by a few percentage points, five percentage points, then what we’re doing is we’re only having 15% going to the hospital. If you can drop this 20 down to 15%, then that there represents a 25 percent reduction in the number of people needing ventilators, needing beds.
如果我们可以将免疫功能提高几个百分点,五个百分点,那么我们会看到去医院就只有15%。如果将这20个降低到15%,则意味着需要呼吸机和床的人数减少了25%。
What’s also important here is that whatever it is that you need to do here it has to be something that doesn’t have to be produced. You don’t have to go to the store to buy it. And the nice and interesting thing about hydrothermal therapy, if in fact this works and we don’t have randomized placebo-controlled trials that show us that it works, but if it does work, it’s something that anybody can do.
还有一点很重要,无论你需要在这做什么,都不应该是需要生产的东西。你不必去商店购买它。这就是关于水热疗法的一件有趣的事:如果实际上它好用,而且我们没有随机安慰剂对照试验证明它好用。但是,如果它确实起作用,那么任何人都可以做。
And with that, I just want to thank the viewers out there who’ve been watching these videos because there’s been a lot of feedback and there’s been a lot of ideas and some of you have forwarded me articles that I would not have known about if it wasn’t for your work and time. And I think that’s one of the things about this forum and this channel that allows us to move forward.
在此,我只想感谢一直在观看这些视频的观众,因为有很多反馈,并且有很多想法,并且有些人转发给我一些不知道的文章,这都要感谢你们的付出。我认为这就是会使我们这个平台继续前行的关键。




Add comment