New Data on COVID-19 vs Other Viral Infections (Ventilator Outcomes) (Lecture 49)
关于COVID-19与其他病毒感染的新数据; 呼吸机结果
Welcome to another MedCram Covid-19 update. We are now officially over 1 million cases confirmed. The United States is well on its way to a quarter of a million cases. If Europe was a country, then it actually would be number one in the world in terms of infections.
欢迎大家收听MedCram Covid-19最新一期课程。现在,我们已经正式确认超过100万确诊病例。美国即将达到250,000病例。如果欧洲是一个国家,那么就感染而言,它实际上将是世界第一。
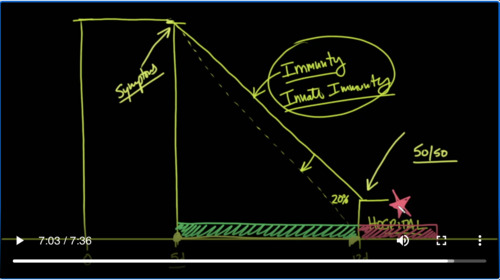
Keep in your mind the chart of what is going on here with Covid-19. We have here on Day Zero infection and then the infection persists for about 5 days of incubation, between day 5 and day 12 is the symptomatic period of growing and build. And this is of course an average, and 80% of people in this period will exit out of this cycle without any further intervention, no need for oxygen, no need to visit the emergency room, no need to be admitted.
请看这张Covid-19的趋势表。我们在第零天感染,然后感染潜伏约5天,在第5天和第12天之间是生长和形成的症状期。这当然是平均水平,并且在此期间80%的人无需任何进一步干预即可退出这一周期,无需氧气,无需前往急诊室,无需入院。
But it’s about 20% of those people here that need to be hospitalized. And of course some of those will just need supplemental oxygen, maybe some observation. But again, some of those may need to be put on a ventilator. I know ventilators intimately well. I’ve trained for most of my educational life on how to run a ventilator and how to control a ventilator. The ventilator is a major tool in my toolbox of pulmonary treatments.
但是,大约有20%的人需要住院。当然,其中一些只需要补充氧气,也许需要观察一下。但是同样,其中一些可能需要上呼吸机。我非常了解呼吸机。在我的大部分教育生涯中,我都接受过关于如何操作呼吸机和如何控制呼吸机的培训。呼吸机是我肺部治疗工具箱中的主要工具。
So you have to understand that there was a little bit of disdain when I saw this article titled Ventilators Are No Panacea For Critically Ill Covid-19 Patients. And I have to say deep down. I know this is true for the flu. And for these viral pneumonia is, in general. Often, we see a tremendous precipitous down trend in patients who are admitted in shock and intubated and within hours are being coded on the ventilator.
你必须了解,当我看到这篇标题为《Covid-19重症患者的呼吸机不是灵丹妙药》的文章时,有些不屑。我必须深入说。我知道对流感确实如此。一般而言,对于这些病毒性肺炎的确如此。通常,我们发现因电击入院、插管、并且几小时之内就在上呼吸机的患者数量急剧下降。
And this article goes through some of the data on this. The first sentence of the story says quite a bit. Most coronavirus patients who end up on ventilators go on to die, according to several small studies and many of the patients who continue to live can’t be taken off the mechanical breathing machines. And they cite a number of articles for it. Probably the most comprehensive article is related to the United Kingdom.
这篇文章介绍了一些数据。第一句话涵义挺多。根据几项小型研究,大多数最终依赖呼吸机的冠状病毒患者会死亡,许多活下来的患者离不开呼吸机。他们为此引用了许多文章。最全面的文章可能与英国有关。
And this report that was just published a few days ago is a report by the Intensive Care National Audit and Research Centre in London, England. And what they did was took information from intensive care units across the United Kingdom and looking at the demographics of these patients that were being admitted and looking at them within the first 24 hours and categorizing them.
几天前刚刚发布的这份报告是位于英国伦敦的重症监护国家审计和研究中心的报告。他们所做的是从英国各地的重症监护病房获得信息,并分析了这些住院患者的人口统计资料,并在最初的24小时内对他们进行了分类研究。
For our benefit, here’s a diagram of the demographics. The mean age at admission was around 60 years of age. There is definitely a predilection of male versus female here in terms of those patients being admitted to the Intensive Care Unit.
这是一张人口统计图,对我们有益。入院时的平均年龄约为60岁。就重症监护病房入院的患者而言,男性与女性之间绝对存在差异。
And here when we look at the body mass index remembering that a body mass index of 25 to 30 is deemed to be overweight and greater than 30 is deemed to be obese, you can see that the majority of the patients are definitely in the overweight category, with approximately 70% of the patients being admitted to the Intensive Care Service being overweight.
当我们查看体重指数时,记住体重指数25至30被认为是超重,而体重指数大于30被认为是肥胖,你可以看到大多数患者肯定属于超重类别,重症监护病房中约有70%的患者超重。
Here we can see a breakdown of admission what the age of the patient is. And you can see it in relation to male versus female. Just about every category males outnumber females in terms of admission to the Intensive Care Service.
我们在这可以看到患者年龄的入院细分,并且可以看到男女之间各项差异。就进入重症监护室而言,几乎所有类别的男性数量上都超过女性。
Perhaps however, this is the most interesting table. In the First Column, we’re looking at the data from just Covid-19 patients. But in the second column, we’re looking at non Covid-19 viral pneumonia patients. So there are other viruses that can also cause pneumonia. These of course could be influenza or respiratory syncytial virus. In the past non Covid-19 patients, patients with pneumonia, 77 percent of them would leave the Intensive Care Service alive. Here 52% of Covid-19 patients are ending up leaving the Intensive Care Service alive and a whopping 48 percent are dying in the Intensive Care.
这是最有趣的表。在第一栏中,我们仅查看Covid-19患者的数据。但是在第二栏中,我们正在研究非Covid-19病毒性肺炎患者。因此,还有其他一些病毒也会引起肺炎。这些当然可能是流感或呼吸道多核体病毒。在过去的非Covid-19肺炎患者中,有77%的患者活着离开重症监护。在这里,有52%的Covid-19患者最终活着离开了重症监护室,而48%的病人死于重症监护,这一百分比还是相当多的。
The thing that’s interesting at least in the United Kingdom is whether its length of stay or the duration of organ support. When you look and compare to other viral pneumonia, the critical care time, either in survivors, nonsurvivors, advanced respiratory support, total respiratory support, total cardiovascular support or renal support, seems to be less time in Covid-19 and more time in non Covid-19, meaning that things perhaps are getting better quickly or getting worse quickly in this situation.
至少在英国,有趣的是不管停留时间还是器官支撑的时间,当你与其它病毒性肺炎进行比较时,在Covid-19中,不管是幸存者、非幸存者、晚期呼吸支持、总呼吸支持、总心血管支持还是肾脏支持中的重症监护时间似乎更少,而在非Covid- 19更长,意味着在这种情况下情况可能会快速好转或快速恶化。
Here’s an interesting table in terms of critical care outcomes by patient subgroup. And you can see here that the majority of the patients that are being admitted are in the 50 to 69 age group when they are discharged alive from critical care, but when they died in critical care, the majority of those patients are coming from the 70 plus. When we look at females they have a sixty two point five percent chance of being discharged alive from Critical Care, whereas the males typically have a 50/50 chance of surviving ICU care.
这有一张有趣的表格,按患者亚组的重症监护结果分类的。你可以在这里看到,活着离开重症监护的大多数接受重症治疗的患者年龄是50至69岁年龄段,但死与重症监护中的大多数患者是70岁以上。当我们看女性时,有62.5%的几率从重症监护室中活着出来,而男性通常有50/50的机会活下来。
Interestingly, in terms of BMI, those who are in the obese range tend towards more chance of dying in critical care. And of course I wanted to make an acknowledgement here. So you have to realize that if you are ending up the hospital right here at the end, only a fraction of these patients will go to the Intensive Care Unit and end up on a ventilator. But if you do, it looks as though on average it’s about a 50-50 chance depending on what age group or demographic you’re part of and here is where you start to realize that you have symptoms of some sort of viral infection.
有趣的是,就BMI而言,那些处于肥胖范围的人在重症监护中死亡的机会更大。当然,我想在此承认一点。你必须意识到,接受入院治疗患者中只有一小部分会去重症监护病房,最后要依赖呼吸机。但是,如果你这样做了,根据你所处的年龄段或人群,似乎平均有50-50几率,这是你开始意识到自己患有某种病毒感染症状的地方。
And you of course you can’t tell if you have Covid-19 at the onset of these symptoms. You probably have the virus for about 5 days and you’ve got a certain time period between the time of onset of symptoms until when you might need to go into the Intensive Care Unit. In my estimation, the time period between onset of symptoms and needing to go to the hospital is the golden period of time that you need to act to make a difference. And it seems as though increasingly more and more that this period here in the hospital is going to be a more difficult time to act.
而且,你当然无法确定在这些症状发作时是否患有Covid-19。你可能已感染病毒约5天,而且从症状发作到可能需要进入重症监护病房还有一段时间。根据我的估计,从症状发作到需要去医院之间的时间段是你需要采取行动以做出改变的黄金时间段,并且似乎越来越是这样的情况,即在医院这段时间将是一个更困难的时期。
However, I do have to acknowledge that this area here is where I am trained to do my best work, but we will tell you this. Whether or not we are looking at the prevention of the infection here at this point in the first phase, whether it is after your infection and in the early portions of the viral infection here in the second stage or whether or not it’s towards the ends where the patient is coming into the hospital with severe symptoms towards the third phase, we are going to look at all of these areas and bring you the latest information.
但是,我确实必须承认,这是我受过训练能做到最好的地方,但是我们会告诉你这一点。在中,我们现在是否考虑在第一阶段预防感染,是在感染之后以及在第二阶段在病毒感染的早期阶段,还是到最后患者在第三阶段时出现严重症状进入医院,我们将研究所有这些领域并为您提供最新信息。
Thanks for joining us.




Add comment