新冠病毒变异追踪及对患者、医务人员和医院的忠告
Testing Problems, Mutations, COVID-19 in Washington & Iran (Lecture 29)
Welcome to another MedCram covid-19 update, and I have been off for a few days from the updating because it was my turn to take the helm of the ICU. What we’re gonna be talking about is No1: 5 new deaths in Washington state yesterday. We are definitely in the growth phase here in the United States, but we can’t tell how much of a growth phase there is because we’re going to talk about testing and the lack of testing.
欢迎来到MedCram covid-19的另一个更新,由于该轮到我接管ICU了,所以我已经离开了几天。我们要谈论的是第一名:昨天华盛顿州有5例新死亡。在美国,我们肯定处于增长阶段,但由于我们要谈论测试和缺乏测试,因此我们无法确定增长阶段有多大。
And we’re also going to talk about preparation; what to do before this hits now. We’ll talk about mutations. We are at a total confirmed worldwide cases here of boards of 90,000; total deaths is over 3,000; total recovered is well over 10 times, that is at 47,000. And those are the published numbers.
我们还将讨论准备工作;现在该怎么做才行。我们将讨论突变。在全球范围内,我们已确认的董事会案例总数为90,000;死亡总数超过3,000;总回收率是10倍以上,即47,000。这些是已发布的数字。
I’ve heard a number of people talk about the numbers in Asia, and the model to look at in some people’s opinion is going to be South Korea because it is a country that’s doing very aggressive testing, and it’s an open and democratic country. But I think the biggest thing there is the fact that they are aggressively testing, and that’s not something that we’re doing yet here in the United States for a number of reasons, which we’ll talk about.
我已经听到很多人谈论亚洲的数字,而在某些人看来,该模型将是韩国,因为它是一个进行非常积极的测试的国家,并且是一个开放和民主的国家。但是我认为最大的事实是,他们正在积极测试,出于多种原因,我们在美国这里还没有这样做,我们将在后面进行讨论。
Going over to the Worldometer website. We look at the close cases to kind of get an idea of where we’re going on the mortality because these are closed cases. You’ve either recovered, or you haven’t, and if you look at this graph, you can see that the mortality rate continues to drop. These are the people that were tested, and we’re already at about 6%; that’s going to go much lower than that once we get the full scope of the infection.
转到Worldometer网站。我们看一些封闭的案例,以便对死亡率的去向有所了解,因为这些都是封闭的案例。您已经康复,或者尚未康复,如果您查看此图,您会发现死亡率继续下降。这些是经过测试的人,而我们已经达到6%。一旦我们获得了全部感染范围,这一数字将大大降低。
Here we have total cases worldwide. Things are starting to level off here. And I think the reason why we’re starting to accelerate again is because we’re going into the epidemic phase in a number of these other countries. And looking at latest updates for today, March 3rd, maybe a little bit behind because this is a fluid situation. By the time this gets published, there are 477 new cases and 6 deaths already today in South Korea, of course South Korea, being in the part of the world, that is the furthest ahead in time.
在这里,我们拥有全球范围内的全部案件。事情在这里开始趋于平稳。而且我认为我们之所以再次开始加速的原因是,我们正在其他许多国家进入流行病阶段。并查看3月3日今天的最新更新,可能有点落后,因为这是一个不稳定的情况。到本文出版时,韩国已经有477例新病例和6例死亡,当然,韩国在世界范围内,是时间最遥远的国家。
If we look at yesterday, we have the first case in Morocco. This was somebody from Italy. Yesterday 21 new cases and 5 new deaths here in the United States. And looking to Washington, it is going to be very important to see what’s going to work in this country and what’s not going to work. Notice that a lot of these people who are dying are in their 70s. However, there is a man in his 40s hospitalized in critical condition in Kirkland, 1 in Rhode Island, and that was a teenager contact of the previous case.
如果我们昨天看,我们在摩洛哥有第一例。这是来自意大利的人。昨天,美国有21例新病例,5例新死亡。展望华盛顿,了解该国的行之有效和不行的将非常重要。请注意,许多垂死的人都在70多岁。但是,有一个四十多岁的男子在罗克岛的柯克兰(Kirkland)住院,病情危重,一名在罗德岛(Rhode Island),那是上一次病例的少年接触。
All of these people again went to the same trip to Italy. They’re saying here this is precisely why we are being so aggressive and identifying contacts and testing people who are symptomatic. There are three people in California in Santa Clara County including a couple who has recently traveled to Egypt, and there are now two in Oregon, one an adult in a county hospital in Walla Walla Washington, and the other is the contact of the first case in Oregon who is recovering at home. There are two new cases in Florida, and that is the first one in New York.
所有这些人再次去了意大利。他们在这里说这正是我们如此积极进取并确定联系人并测试有症状人员的原因。在加利福尼亚州,圣塔克拉拉县有3个人,其中包括一对最近去过埃及的夫妇,现在在俄勒冈州有2个人,一个是成年人在华盛顿州Walla Walla的县医院里接受的,另一个是第一个病例的联系方式在俄勒冈州,他正在家里康复。佛罗里达有两个新病例,这是纽约的第一个。
Interesting interview on CNBC. That’s also here on the Worldometer website. Dr. Mac McCarthy, who is an ER physician at new york-presbyterian. He says I’m here to tell you right now at one of the busiest hospitals in the country. I don’t have at my fingertips a rapid diagnostic tests. I still have to make my case plead to test people. This is not good. We know that there are 88 cases the United States. They’re going to be hundreds by the middle of the week. They’re going to be thousands by next week. And this is a testing issue quote “in New York state, the person who tested positive is only the 32nd test we’ve done in this state; that is a national scandal.
CNBC有趣的采访。也可以在Worldometer网站上找到。 Mac McCarthy博士是纽约长老会的急诊医师。他说我现在在这里告诉你在该国最繁忙的医院之一。我没有触手可及的快速诊断测试。我仍然必须让我的案子去测试人们。这个不好。我们知道美国有88例。到本周中旬,他们将成百上千。下周他们将成千上万。这是一个测试问题的报价:“在纽约州,测试阳性的人只是我们在该州进行的第32次测试;这是全国性的丑闻。
“They’re testing 10,000 a day in some countries, and we can’t get this off the ground,” McCarthy said, ” I’m a practitioner on the firing line, and I don’t have the tools to properly care for patients today.” And I can tell you I resonate with that as a healthcare worker. In the ICU all last week seeing patients in the emergency room. We are taking protective measures to make sure that we don’t get exposed to people coming into the hospital with covid-19, causing a lot of our health care workers to be quarantined.
麦卡锡说:“他们在某些国家/地区每天要测试10,000个,我们无法将其付诸实践。”今天的病人。”我可以告诉您,作为医疗保健工作者,我对此表示共鸣。上周在重症监护病房都在急诊室就诊。我们正在采取保护性措施,以确保我们不会与暴露于covid-19的人接触,从而导致我们的许多医护人员受到隔离。
So it’s really important that if anybody goes to the emergency room, to call ahead, make sure that they’re following instructions, make sure that they’re wearing a mask, especially if they have a fever, and they have symptoms, because anybody that they infect, no matter who they are, will have to be quarantined, and of course if those people that are being quarantined are our healthcare providers, well, that’s just fewer people to be able to care for other people that need it.
因此,重要的是,如果有人去急诊室打电话,请确保他们遵循指示,确保他们戴着口罩,尤其是在发烧且有症状的情况下,因为任何人无论他们是谁,都必须进行隔离,当然,如果那些被隔离的人是我们的医疗保健提供者,那么,能够照顾其他需要它的人的人就更少了。
Now the good news there is that, as I understand it, there are going to be a lot more tests available, but they’re not going to be available until later this week. There are regulations that the FDA imposes on commercial manufacturers of these tests. They have to reach certain goals, and it’s a long and laborious procedure to get these things approved by the FDA. Those are being relaxed so we can get enough tests on the market and get labs up and running.
现在,好消息是,据我了解,将会有更多的测试可用,但是直到本周晚些时候才可以使用。 FDA对这些测试的商业制造商有规定。他们必须达到某些目标,要使这些东西获得FDA批准是一个漫长而费力的过程。这些放宽了,因此我们可以在市场上进行足够的测试,并建立并运行实验室。
What you ideally want to do, and this goes back to the days of medical school when we were trained in surgery. It was always a good thing. If you took somebody occasionally to surgery for appendicitis and you pulled out a completely normal appendix. That means that you are not missing any, that means you work fighting negative test results, true negatives. So you actually need to screen widely enough so that you know you’re getting enough negative testing. What you don’t want to be doing is testing so limited that the number of tests you’re getting, you’re not catching the full magnitude of the infection.
您理想地想做的事情,可以追溯到我们接受外科手术培训的医学院的时代。这总是一件好事。如果您偶尔因阑尾炎而接受手术,而您拔出了完全正常的阑尾。这意味着您不会错过任何东西,这意味着您将与否定的测试结果抗争,真正的否定。因此,您实际上需要进行足够广泛的筛选,以使您知道自己得到了足够的负面测试。您不想做的是测试非常有限,以至于要进行的测试数量众多,无法完全感染。
And so I think everyone believes, and everyone’s on the same page here, that the amount of testing that needs to be done right now in this country needs to be ratcheted up by orders of magnitude over what we’re getting right now.
因此,我认为每个人都相信,并且每个人都在同一页面上,该国家现在需要完成的测试数量需要比我们现在所获得的数量多几个数量级。
Here’s a story that was published in the AP a couple of days ago, and it talks about what’s going on, especially up in Washington, where the hot spots are, says here as Americans prepared, researchers at the Fred Hutchinson Cancer Research Center and the University of Washington on Sunday said that they had evidence the virus may have been circulating in the state for up to six weeks undetected.
这是几天前在美联社上发表的一个故事,它讲述了正在发生的事情,特别是在华盛顿热点地区,正如美国人准备的那样,这里是弗雷德·哈钦森癌症研究中心和华盛顿大学周日表示,他们有证据表明该病毒可能已经在该州传播长达六周之久,未被发现。
A finding that if true could mean hundreds of undiagnosed cases in the area. They posted their research online, but it was not published in a scientific journal or reviewed by other scientists. Trevor Bedford, an associate professor who announced the preliminary findings on the virus in Washington state, said on Twitter late Saturday that genetic similarities between the state’s first case on January 20th and a case announced Friday indicate that the newer case may have descended from the earlier one.
如果发现为真,则可能意味着该地区数百例未诊断的病例。他们在网上发布了他们的研究成果,但没有发表在科学期刊上或未经其他科学家评论。宣布华盛顿州有关该病毒的初步发现的副教授特雷弗·贝德福德(Trevor Bedford)周六晚在Twitter上表示,该州1月20日的第一例病例与周五宣布的病例之间的遗传相似性表明,较新的病例可能是早期病例的后继病例。一。
Now, this is going to be something that we’re going to talk about when we talk about molecular biology. It is this idea about descendants. So the thing that you’ve got to understand is that the virus, when it infects your cell, it takes over the cells machinery to create more viruses, but the genes that the virus brings in is kind of sloppy, and so because of that sloppiness, there’s a lot of mutations that are made, and some of those mutations may actually end up changing amino acids. Some of those mutations won’t translate into differences in amino acids, but you can still see those mutations. And as you track those mutations in time, you can see which virus strain descended from another.
现在,这将是我们谈论分子生物学时要谈论的问题。这是关于后代的想法。因此,您必须了解的是,这种病毒在感染细胞时会接管细胞机制以产生更多病毒,但是该病毒带来的基因有些草率,因此lop草,产生了许多突变,其中一些突变实际上可能最终会改变氨基酸。其中一些突变不会转化为氨基酸差异,但您仍然可以看到这些突变。当您及时跟踪这些突变时,您可以看到哪个病毒株是另一个病毒株。
Now, those mutations can occur randomly anywhere along the genetic thread, the RNA as it turns out in this case with coronavirus, but if those mutations affect a key component, for instance, the binding protein or the spike protein on the coronavirus, that allows it to infect human cells. Well, that virus is just not going to be able to infect the next human cell, but because there are millions and millions that are made. there’s always another one right behind it that’s going to happen.
现在,这些突变可以沿着遗传途径的任何地方随机发生,在这种情况下,冠状病毒就是RNA,但是如果这些突变影响了关键成分,例如冠状病毒上的结合蛋白或刺突蛋白,则可以它可以感染人体细胞。好吧,这种病毒只是无法感染下一个人类细胞,而是因为有成千上万的病毒在制造。总有另一种情况会发生。
The bottom line is you rarely are going to see viruses, copies of the virus, infecting human cells that have a mutation that is critical in the binding of that protein, and therefore the binding of that site now, in this case, the binding site in the human being is the H2 receptor in the cells, in the bronchi, or the lining of the lungs. So that’s a highly conserved area.
最重要的是,您很少会看到病毒,病毒的副本,感染具有突变的人细胞,该突变对于该蛋白的结合至关重要,因此现在对该位点的结合至关重要,在这种情况下,就是该结合位点人体内的H2受体是细胞,支气管或肺内膜中的H2受体。因此,这是一个高度保护的区域。
Why is that? It’s highly conserved because those are the only viruses that are going to infect the human being. But if you look at these, just like the human race has different families, different last names, because they’re related to each other. Different coronavirus, different SAS-COV-2, different covid-19 viruses, in other words, if you were to look at the ones in Wuhan vs the ones in Washington, they are not identical to each other, they have mutated in some way, and what you can do is actually come up with a family tree, and you can see where these things came from.
这是为什么?它是高度保守的,因为这些是唯一会感染人类的病毒。但是,如果您看这些,就像人类有不同的家族,不同的姓氏一样,因为它们彼此相关。不同的冠状病毒,不同的SAS-COV-2,不同的covid-19病毒,换句话说,如果您要看武汉的病毒与华盛顿的病毒,它们是彼此不相同的,它们以某种方式发生了突变,您实际上可以拿出一棵家谱,然后您可以看到这些东西的来源。
They say “I believe we’re facing an already substantial outbreak in Washington state that was not detected until now due to narrow case definition requiring direct travel to China. Scientists not affiliated with the research,” said the results did not necessarily surprise them and pointed out that for many people, especially the younger healthier ones, the symptoms are not much worse than the flu or a bad cold.
他们说:“我相信我们正面临华盛顿州已经爆发的大规模疫情,由于病例定义狭窄,需要直接前往中国,因此直到现在仍未被发现。与研究无关的科学家们,”研究结果并不一定会让他们感到惊讶,指出对于许多人,特别是较年轻的人,症状并不比流感或重感冒严重得多。
He says we think that this has been a pretty high rate of mild symptoms and can be asymptomatic. The symptoms are pretty nonspecific, and testing criteria that have been pretty strict, and this is really the key here. Up to this point, you could not get testing unless you had traveled to that specific portion of China where the virus was. So these combinations of factors mean that it easily could have been circulating for bit without knowing, suggesting Lesler. So people are saying that this is high-quality work.
他说,我们认为这是一种相当高的轻度症状,并且可能是无症状的。症状是非常特定的,并且测试标准非常严格,这才是真正的关键。到目前为止,除非您前往该病毒所在的中国特定地区,否则您将无法进行测试。因此,这些因素的组合意味着它很容易在不知不觉中流传了一下,莱斯勒建议。因此人们说这是高质量的工作。
So what I want to do is talk a little bit more about what is going on with this mutation, and I want to introduce you to a really cool site, and that website is called Nextstrain, and this actually does real-time tracking of pathogen evolution.
因此,我想做的是更多地谈论这种突变的发生情况,我想向您介绍一个非常酷的网站,该网站称为Nextstrain,它实际上对病原体进行实时跟踪演化。
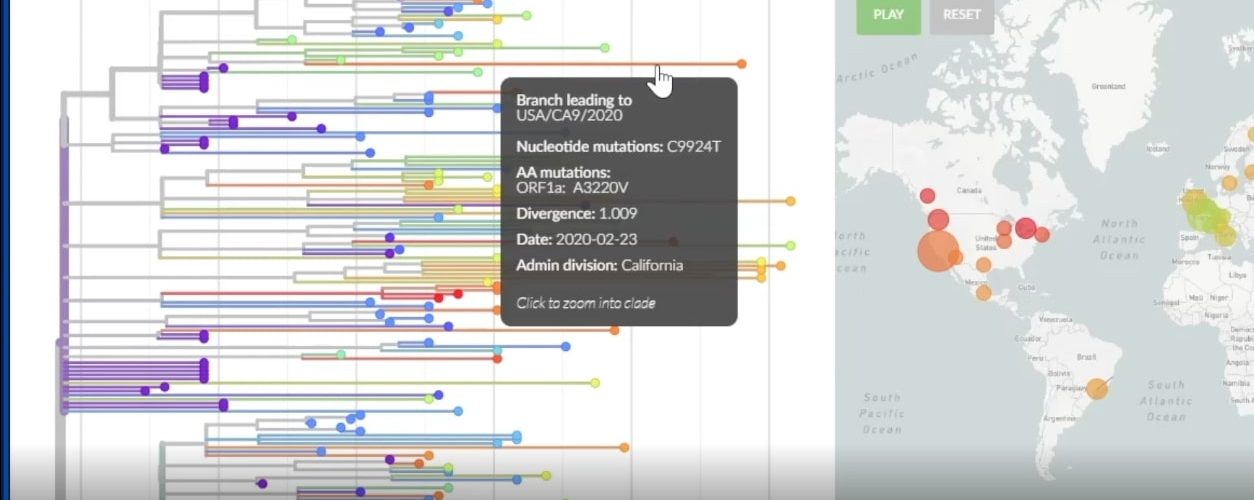
If we click on the latest data and analysis here, what we’ve got here is the SARS-COV02 genome, and I think this is really cool. What you can see here, we have the initial strain over here, and we can see how through time the different mutations have occurred in different family trees. So if we play this, you can see that things started out here in Wuhan. But as things have spread across the world, there have been mutations, and we can see what the descendants are as we track it.
如果单击此处的最新数据和分析,那么这里得到的就是SARS-COV02基因组,我认为这真的很酷。您在这里可以看到,我们在这里有了初始负担,并且可以看到随着时间的流逝,不同的家族树中发生了不同的突变。因此,如果我们玩这个游戏,您会发现武汉的事情从这里开始。但是随着事情在世界范围内的传播,已经发生了变异,我们可以在追踪过程中看到后代是什么。
So interestingly the one here in California, it shows that there are nucleotide mutations from the original. There are amino acid mutations in the ORF-1-A gene; we will talk more about that. That is the gene in the virus that codes for the protein that allows it to reproduce the RNA genome of the virus.
有趣的是,这是加利福尼亚的一个,它表明原始分子中存在核苷酸突变。 ORF-1-A基因中存在氨基酸突变。我们将进一步讨论。那是病毒中的基因,它编码允许其复制病毒RNA基因组的蛋白质。
And if we look down here, we can actually see the genome of the virus. This is the entire RNA of the coronavirus, specifically that we’re talking about here, the ORF-1-A gene and the ORF-1-b gene. For those of you who are molecular biology buffs, there’s actually an overlap in that gene right here that requires a frameshift on the ribosome to be able to translate both of these, and we’ll talk more about that in the coming sessions and updates.
如果我们在这里往下看,我们实际上可以看到病毒的基因组。这就是冠状病毒的整个RNA,特别是我们在这里所说的ORF-1-A基因和ORF-1-b基因。对于分子生物学爱好者来说,这里的基因实际上存在重叠,需要核糖体上的移码才能翻译两者,我们将在以后的会议和更新中详细讨论这一点。
What this here represents is where these mutations in the genome are occurring. We see that there are a lot of mutations occurring down here in these small genes, and not so much here. This S gene right here codes for the S protein. We can see that there are some mutations; some of these mutations may not be actually changing amino acids. However, this s protein is the spike protein on the very outside of the cell. This is the protein that is going to be binding to the ACE2 protein on the human lung cells that allows it to bind and infect them. Ostensibly, this is the portion of the RNA genome of the virus they would be injecting into your cells as a possible vaccine so that your cells could take this instruction, make the S protein inside your body, which would cause an antibody response, which would then give you the vaccine against the coronavirus.
这表示基因组中这些突变发生的位置。我们看到这些小基因在这里发生了很多突变,而在这里没有那么多。这里的S基因编码S蛋白。我们可以看到其中有些突变;其中一些突变可能实际上并未改变氨基酸。但是,这种s蛋白是细胞最外层的刺突蛋白。该蛋白将与人肺细胞上的ACE2蛋白结合,从而使其结合并感染它们。表面上看,这是它们将作为可能的疫苗注射到您的细胞中的病毒RNA基因组的一部分,以便您的细胞可以按照此说明进行操作,在体内产生S蛋白,这会引起抗体反应,然后给您接种冠状病毒疫苗。
At this point, I’d like to talk to health care providers and people who are leaders in their community, people who are members of medical groups. This is the time now to start communicating with your patients, educate them.
在这一点上,我想与医疗保健提供者以及社区中的领导者,医疗团体的成员进行交谈。现在是时候开始与您的病人沟通,教育他们了。
What are they supposed to do? If they get sick, if they develop a fever, if they develop a sore throat, if they are otherwise healthy, they don’t have shortness of breath. They’re not hypotensive, the best thing to do is to self-quarantine and stay home. Do not overburden your health care delivery system. They’re going to be plenty busy with people who are worse off. If you are going to go to the hospital, make sure you call ahead, find out what the procedures are, because they’re going to want to make sure that you’re isolated. They’re going to probably give you a mask.
他们应该怎么办?如果他们生病了,发烧了,嗓子疼了,如果他们健康的话,他们没有呼吸急促。它们不是低血压的,最好的办法是自我隔离并待在家里。不要给您的医疗服务提供系统增加负担。他们将与处境较差的人一起忙碌。如果您要去医院,请确保提前致电,查明程序是什么,因为他们将要确保您与外界隔离。他们可能会给你口罩。
Things to think about as well is to make a plan on where to go. There are hotlines. People are going to be calling in. If you have a Nurse Advice Line, make sure you double it or triple it because the volume of calls are going to increase; people are going to be very concerned. If you have the ability to do telemedicine, that’s what you should do. The coronavirus cannot infect somebody over the phone.
还需要考虑的事情是要计划去哪里。有热线电话。人们会打来电话。如果您有护士咨询专线,请确保将其增加一倍或三倍,因为通话量将会增加。人们将非常关注。如果您有能力进行远程医疗,那就是您应该做的。冠状病毒不能通过电话感染某人。
Next thing we need to do is plan for a surge, so that means that people who are in the hospital may be overwhelmed, and they may need to get into resources that are normally in the outpatient setting, people who are doing, for instance, Well checks.
我们接下来要做的是计划一个大手术,这意味着医院的人们可能会不知所措,他们可能需要进入通常在门诊环境中的资源,例如正在做手术的人,好检查。
Hospitals themselves need to start thinking about hospitals within hospitals. So, in other words, a dedicated unit for people that you suspect as having coronavirus, a place that you would need to have negative pressure rooms so that you’re not blowing out the aerosolized coronavirus into other parts of the hospital.
医院本身需要开始考虑医院内部的医院。因此,换句话说,这是一个专门为您怀疑患有冠状病毒的人提供的病房,在这个地方您将需要有负压室,以免将雾化的冠状病毒吹到医院的其他地方。
Something as practical as understanding that most operating rooms are under positive pressure. Some of the more modern ones can switch to negative pressure. But if you take a coronavirus patient into a positive pressure operating room, that’s not going to be a good thing. It could also be very expensive to have the ability to have coronavirus treatment all throughout the hospital, you need to have a dedicated place where contact is minimized, and the people working in that area are going to have maximal PPE (or personal protective equipment), and not have to burn through a lot of these materials because they’re going to be limited. So the time is now to start putting these procedures in place.
了解大多数手术室处于正压力下的实际操作。一些更现代的产品可能会转换为负压。但是,如果您将冠状病毒患者带入正压手术室,那将不是一件好事。拥有在整个医院进行冠状病毒治疗的能力也可能非常昂贵,您需要有一个专门的场所以尽量减少接触,并且该地区的工作人员将拥有最大的PPE(或个人防护设备) ,并且不必烧掉很多这些材料,因为它们将受到限制。因此,现在该开始着手执行这些程序了。
Now, of course, this situation is very fluid right now. Thanks for joining us.
当然,现在这种情况现在非常不稳定。感谢您加入我们。




Add comment