美国医学院讲师清晰讲解肝脏工作机理、内分泌与外分泌系统;毒细胞检测方法(ACT, SGOT, ALT, SGPT, Albumin, PK, PK/INR)及各自的局限性;急、慢性肝病检测值区别;酒精肝检测值;服用血液稀释药物对PK/INR值的影响等。
本文由‘中国推动’学者,华东政法大学Popoko同学与中山大学南方学院LZCHING同学翻译编辑。
通过高质量医学视频课程,了解肝病其治疗(treatment),肝功测试(liver function tests)和胆汁淤积性(cholestatic)疾病。
MedCramChina医学视频使您可以缩短学习时间,并通过专注于最重要的内容来最大程度地保留和理解相关医学知识。医学插图,图表,辅助记忆和测验将使学习和复习医学主题变得轻而易举。您会发现《肝脏解释》非常有用,易于理解且很有趣。
Welcome to another MedCram lecture! We’re going to talk about the liver. There have been some requests to go over the liver, and we are going to look over this. In terms of an overview, I first like to start with the anatomy. So if you can imagine the liver, it’s a pretty large organ, sits in the abdomen, and it has a number of functions, which we’re going to go over.
欢迎参加另一个MedCram讲座!我们将谈论肝脏。已经有一些要求讲解肝脏的要求,我们将对此进行研究。在概述方面,我首先想从解剖学入手。因此,如果您能想象到肝脏,它是一个相当大的器官,位于腹部,并且具有许多功能,我们将继续介绍。
The first thing you’ve got to look at is what goes into the liver and what comes out of it. The first thing that you’ll notice with the liver is that there are two inputs to it, which are called portal vein and hepatic artery. So this is the hepatic artery, and there are two of them. They split, and this is not drawn to anatomical scale; it’s kind of schematic, and this is coming from the heart. So this is oxygenated blood. The other input is the portal vein. And this is coming from the intestines.
您首先要了解的是肝脏中的成分以及肝脏中的成分。首先要注意的是,肝脏有两个输入,称为门静脉和肝动脉。所以这就是肝动脉。有两个。他们分开了,这并没有按照解剖学的比例绘制,只是一种示意图,而这是发自心脏的。所以这是含氧的血液。另一个输入是门静脉。这是从肠子来的。
This is important because a lot of medications that you ingest like pills, the first place that they go is to the liver. So the metabolism of these medications first occurs in the liver, which is called the first-pass metabolism. Then they go on to the heart, and that’s the next part of the drawing here. You get the hepatic vein.
这很重要,因为您摄取的许多药物首先要运到肝脏。因此,这些药物的新陈代谢首先发生在肝脏中。这被称为首过代谢,然后它们进入心脏,这就是这里的下一部分, 然后它们到了肝静脉。
So there are two inputs and one output, and so it’s gonna go through the liver. If it’s coming from the portal vein, from the intestines. Now in terms of output or exocrine; we know where happens to endocrine; it goes into the blood.
因此,有两个输入和一个输出,因此它将通过肝脏。如果它来自门静脉,则来自肠道。现在就外分泌而言;我们知道内分泌发生在哪里;它进入血液。
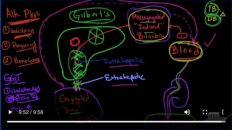
But in terms of exocrine, there are two major outputs, you’ve got a hepatic duct, a right hepatic duct, and a left hepatic duct, and they combine into the common hepatic duct. Then they meet up with the cystic duct, which is from the gallbladder, which stores bile and that forms the common bile duct, which then dumps into the intestines. And that’s how the body gets rid of it.
但就外分泌而言,有两个主要输出;有一个肝管,一个右肝管和一个左肝管,它们合并成肝总管,然后与来自胆囊的胆囊管储存胆汁并形成胆总管,然后胆囊管排入肠内。这就是身体如何排除它的方式。
So the liver really has two functions. It has endocrine functions and exocrine functions. The endocrine functions are that hormones produced in the cells regulate glucose, produce albumin., etc. There are a whole bunch of things that they do, and their output gets dumped into the hepatic vein, and that goes on to the heart, where it gets pumped for the whole body.
因此,肝脏确实具有两个功能。它具有内分泌功能和外分泌功能。内分泌的功能是细胞中产生的激素调节葡萄糖,产生白蛋白等。它们起着很多作用,其输出被倾倒入肝静脉,然后进入心脏或由心脏泵入整个身体。
The heart also pumps oxygenated blood to the liver because the liver just like any other organ needs oxygenated blood to survive, and that’s where it gets its supply. But the major source of blood supply to the liver is actually from the portal vein, and this includes the stomach, the duodenum, the jejunum, the ileum, the colon, all the way down to the rectum.
心脏也将含氧的血液泵送到肝脏,因为肝脏就像其他器官一样需要含氧的血液才能生存,这就是它的来源。但是,肝脏的主要血液供应来源实际上是门静脉,包括胃,十二指肠,空肠,回肠,结肠,一直到直肠。
Basically, it is blood, all of the fatty acids, all of the nutrients that you get absorbed take the first pass, and they go to the liver, and that’s kind of the circulatory and the endocrine and the exocrine functions of the liver. Of course, the exocrine functions are: it produces bile; biles are these things that break down fats. It’s what’s makes your poo look brown, and 50% of it approximately is stored in the gallbladder at each meal. So it can be ejected into the cystic duct, into the common bile duct, and into the duodenum, so it can help in aiding indigestion.
但是,肝脏的主要血液供应来源实际上是门静脉,包括胃,十二指肠,空肠,髂骨,结肠,一直到直肠。基本上是血液,所有脂肪酸,所有被吸收的营养素都会经过肝脏,然后进入肝脏,这就是肝脏的循环,内分泌和外分泌功能。当然,外分泌功能是:产生胆汁。胆汁是分解脂肪的东西。这就是使您的便便看起来呈棕色的原因,每餐中大约有50%的便便存储在胆囊中。因此可以将其排出到胆囊管,胆总管和十二指肠,从而有助于消化不良。
The next I want to talk about are the blood tests that are associated with the liver, and these are sometimes confusing. Let’s go over those. The first one, or the first type of blood test, that I want to go over is what I call the cytotoxic blood tests. So what are the cytotoxic blood tests? Well, the first one is AST. This is also known as the SGOT. This enzyme is actually made in the liver. In fact, it’s not specific to the liver; it is in a number of cells. But you can see it in a number of cells but also in the liver.
接下来我要谈的是与肝脏相关的血液检查,这些检查有时会令人困惑。让我们来看看那些。我想进行的第一个或第一种血液测试是所谓的细胞毒性血液测试。那么什么是细胞毒性血液测试?好吧,第一个是AST。这也称为SGOT。这种酶实际上是在肝脏中产生的。实际上,它不是特定于肝脏的。它存在于许多细胞中,但是您可以在许多细胞中以及肝脏中看到它。
The other ones are the ALT, albumin, and PT. By the way, ALT is also known as the SGPT. AST and ALT are simply enzymes that are in the hepatocyte, and when the hepatocyte dies, these enzymes get released. So in essence, these are like cardiac enzymes, like when you have a heart attack, you release CK, CKMB, and troponin. When you have an injury of liver cells, that’s when the AST and ALT go up.
其他的是ALT,白蛋白和PT。顺便说一句,ALT也称为SGPT。 AST和ALT只是肝细胞中的酶,当肝细胞死亡时,这些酶被释放。因此,从本质上讲,它们就像心脏酶一样,当您心脏病发作时会释放CK,CKMB和肌钙蛋白。当肝细胞受损时,AST和ALT升高。
Now just like you can have congestive heart failure and a low ejection fraction, and your heart is not contracting very well, and you have heart failure, you might not have elevated CKCK and be in troponin, the same way that if you can be in liver failure. In other words, your hepatocyte is not producing the things that the liver should do. You could also have low AST and ALT.
现在,就像您可能会出现充血性心力衰竭和低射血分数,并且您的心脏无法很好地收缩,并且您患有心力衰竭,您可能没有CKCK升高和肌钙蛋白一样,就像您处于肝功能衰竭。换句话说,您的肝细胞没有产生肝脏应做的事情。您可能还具有较低的AST和ALT。
So what do we use AST and ALT for? These are basically markers for hepatic inflammation. So hepatic inflammation is tracked by and seen as elevations in the ALT and AST, and we’ll get into a little bit about that in just a second. So the AST specifically has low specificity. For the liver. Okay. It’s seen in the periportal hepatocyte.
那么我们将AST和ALT用于什么呢?这些基本上是肝炎的标志。因此,可以根据ALT和AST的升高来跟踪并观察到肝炎,我们将在短短一秒钟内对此进行一些了解。因此,AST特异性低。对于肝脏, 在门静脉肝细胞中可见。
Okay, whereas the ALT has a high specificity for the liver. Okay. So think of the L here in the ALT as being standing for liver whereas S is more for muscle, but they’re both seen in the liver. Now in terms of both of these, the AST and ALT, they both go up in all forms of liver injury. It’s only good for a recent injury. So if there’s an old injury, you won’t see these elevated. Okay, these tell you nothing about residual function.
好的,而ALT对肝脏具有很高的特异性。因此,可以认为ALT中的L代表肝脏,而S代表肌肉,但是它们都在肝脏中可见。现在,就AST和ALT而言,它们都以各种形式的肝损伤而上升。这仅对最近的受伤成立。因此,如果有旧伤,您将看不到这些伤痕。好的,这些没有告诉您关于病后残存功能的任何信息。
Okay, so if these are low, it doesn’t mean that your liver function is low. It just means there’s no current inflammation going on in the liver. It doesn’t tell me if my liver is good and it is productive, or if my liver is damaged and not functioning well. And the damage is not dose-dependent. So if the AST and ALT are coming down, this doesn’t necessarily mean as a good thing or it’s a bad thing. In other words, a decrease could mean better or worse. So in other words, if the AST and ALT are coming down, it could be that the liver so damaged that there are no more cells to damage, or it could mean that the AST and ALT are coming down; therefore the damaged has ceased.
好吧,如果这些低,并不意味着您的肝功能低下。这只是意味着目前肝脏中没有炎症正在发生。它并没有告诉我我的肝脏是否健康,是否有生产力,或者我的肝脏是否受损且功能不正常。而且损害不是剂量依赖性的。因此,如果AST和ALT下降,这并不一定意味着好事或坏事。换句话说,减少可能意味着更好或更糟。换句话说,如果AST和ALT下降,则可能是肝脏受损导致不再有细胞受损,或者意味着AST和ALT下降。因此,损坏已停止。
Okay, it’s kind of like fire and smoke. This is kind of like smoke. Now you could see smoke go away for two reasons, either because there’s no more stuff to be burned or because the fire has been put out. Okay. I hope that makes sense. Okay, so I cleared the page so we can talk about albumin and PT. Let’s talk about albumin.
好吧,有点像火和烟。这有点像烟雾。现在您可能会看到烟雾消失的原因有两个,要么是因为没有更多的东西要燃烧,要么是因为火被扑灭了。好的。我希望这是有道理的。好的,现在我们讨论白蛋白和PT。让我们谈谈白蛋白。
We’ve talked about albumin before, specifically when we’re talking about anion gap. Albumin is a very complicated protein. It’s made in the liver. And it’s pretty reliable for looking at Chronic hepatocellular injury. So if the albumin is low, that usually equals chronic liver injury, so someone has an acute problem with the liver, their albumins usually stay up. The reason why that is the case is because it has about a 20-day half-lives, which means it takes a long time for the albumin levels to start to go. So I would say this is a good marker for chronic liver disease.
我们之前已经讨论过白蛋白,特别是当我们谈论阴离子间隙时。白蛋白是一种非常复杂的蛋白质。它是在肝脏中制成的。它对于检查慢性肝细胞损伤非常可靠。因此,如果白蛋白水平低(通常等于慢性肝损伤),那么某人的肝脏出现急性问题,他们的白蛋白通常会保持正常状态。之所以如此,是因为它具有约20天的半衰期,这意味着白蛋白水平需要很长时间才能开始下降。因此,我想这是慢性肝病的良好标志。
Finally, in the cytotoxic category, let’s talk about the PT. So what is the PT? PT is the prothrombin time, and it’s pretty reliable for both acute and chronic hepatocellular disease. So it’s acute and chronic. The other way of looking at the PT is also the INR. So, for instance, the PT might be 10. The INR is 1.0. Usually, the PT is about 10 times that of the INR but not always. And this is pretty important and I’ll tell you why; because the PT or the INR simply measures the time of prothrombin to do its work. In other words to have clotting. It’s a clotting time, and clotting times require many different enzymes that are made in the liver.
最后,在细胞毒性类别中,让我们谈谈PT。那么什么是PT? PT是凝血酶原时间,对于急性和慢性肝细胞疾病都非常可靠。所以这是急性的和慢性的。查看PT的另一种方法是INR。例如,PT可能为10。INR为1.0。通常,PT大约是INR的10倍,但并非总是如此。这非常重要,我会告诉你原因;因为PT或INR只是测量凝血酶原完成工作的时间。换句话说有凝块。这是凝血时间,凝血时间需要肝脏中产生许多不同的酶。
This is important because any enzyme that is not successfully made in the liver, it is going to interfere with the PT/INR. So it’s very sensitive. In fact, the PT/INR is the most sensitive liver function tests that can be done. In other words, this is the first thing that starts to get bad as the liver starts to fail because it requires so many proteins that are synthesized in the liver.
这很重要,因为任何无法在肝脏中成功制造的酶都将干扰PT / INR。因此非常敏感。实际上,PT / INR是可以完成的最敏感的肝功能检查。换句话说,这是由于肝脏开始衰竭而开始变坏的第一件事,因为它需要在肝脏中合成的大量蛋白质。
And so what are the things that are associated with the PT? Well, it’s factors. You may remember this from the clotting cascade but factors related to vitamin K, which are 2, 7, 9, 10, also (1 and 5) are related to the PT. So what are some causes that could do this? Well, if the liver is not synthesizing these factors, it’s going to take longer for coagulation to occur, and therefore your PT and your INR will go up. So in liver disease instead of it being a nice 1.0 you start to see it to go to 1.5, 2.0 Etc. This is usually a good sign of chronic liver disease or acute liver disease, and it tells you just how bad their livers are.
那么,与PT相关的是什么?好吧,是因子。您可能在凝血级联中还记得这一点,但与维生素K有关的因子也包括PT,2、7、9、10及1和5。那么,什么原因可以做到这一点呢?好吧,如果肝脏不合成这些因子,那么凝血时间将更长,因此您的PT和INR会上升。因此,在肝脏疾病中,它不是好于1.0,而是开始升至1.5、2.0等,这通常是慢性肝病或急性肝病的好兆头,它告诉您他们的肝病有多严重。
Now, what are some other things other than the liver disease that could cause it? Obviously, if the patient has low vitamin K, that’s going to be a confounder. if the patient obviously is on coumadin, which is a blood thinner, that’s going to confound it. So if they have low vitamin K, just given vitamin K. If they have cumin, and obviously you’re not going to use this test to see if they have liver disease because you’re trying to get their INR up anyway, because that’s why they’re on a blood thinner in the first place.
现在,除了肝脏疾病以外,还有哪些其他原因可能导致它呢?显然,如果患者维生素K含量较低,那将是一个混杂因素。如果患者显然正在服用coumadin(一种血液稀释剂),那将会使它感到困惑。因此,如果他们的维生素K低,就给他们维生素K。如果他们服用coumadin,很明显,您将不会使用此测试来查看他们是否患有肝病,因为您无论如何都试图提高其INR,因为为什么他们首先要稀释血液。
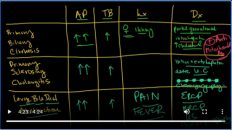
Okay. So let’s review. The AST is a blood test that will tell you if there is acute damage. It has a lower specificity for the liver than those Alt. It’s increased in all types of liver injury. It’s only good for a recent injury. There’s no indication of residual liver functional capacity. The damage is not dose-dependent. All of those go for the ALT except the ALT is a little bit more specific. So I would expect the ALT to be higher if it’s specific to liver disease. The one exception to this is if you have alcoholic liver disease, in which case the AST and ALT may be very similar, sometimes that you even hear of a 2 to 1 or 3 to 1 ratio of AST to ALT in alcoholic liver disease.
让我们回顾一下。 AST是一项血液检查,可以告诉您是否存在急性损伤。它对肝脏的特异性低于那些Alt。它在所有类型的肝损伤中均增加。这仅对最近的受伤成立。没有剩余肝功能的迹象。损害不是剂量依赖性的。ALT对肝脏更为具体。因此,我希望ALT如果针对肝脏疾病则更高。一个例外是如果您患有酒精性肝病,在这种情况下AST和ALT可能非常相似,有时您甚至听说酒精性肝病中AST与ALT的比例为2:1或3:1。
Albumin is reliable for chronic hepatocellular injury. It is synthesized in the liver. It’s a marker for chronic liver disease, and it’s half-life, remember, is about 20 days. The PT is probably the most sensitive blood test for liver disease. And as a result, you will see these elevations in chronic liver disease. Remember it’s obviously going to be elevated if you’re given the patient warfarin or coumadin or things of that nature. Great. So that concludes this. Join us for our next lecture, which is going to talk about cholestatic liver function tests. Thanks very much!
白蛋白对显示慢性肝细胞损伤是可靠的。它在肝脏中合成。它是慢性肝病的标志,记住,它的半衰期约为20天。 PT可能是对肝脏疾病最敏感的血液检查。您将在慢性肝病中看到这些升高。请记住,如果您给患者服用warfarin 或 coumadin或具有这种性质的东西,显然会升高。好了,这样就可以得出结论。加入我们的下一个讲座,下次讲座将讨论胆汁淤积性肝功能检查。非常感谢!


Add comment