无症状传播、睡眠知识
Increase in Deaths, Questions about Asymptomatic Spread, & More Sleep Tips (lecture 18)
Welcome to another MedCram coronavirus update. Let’s take a look at the numbers since the updated criteria for the diagnosis has gone to just a lung scan and a clinical history consistent with coronavirus. 64,436 total confirmed; total deaths 1,383; total recovered is 6886; about five times the total deaths is the total recovered.
欢迎来到另一个MedCram冠状病毒更新。让我们看一下这些数字,因为更新的诊断标准仅用于肺部扫描以及与冠状病毒一致的临床病史。确认总数64,436;总死亡1,383;回收的总数为6886;总死亡人数的五倍左右。
Let’s take a look at the WorldOmeter. And we can see here total cases outside of China have kind of remain constant because there hasn’t been that redefinition causing a slew of new cases. Let’s take a look and see what’s going on inside China, or total cases overall. If we look down here at new cases, there’s been a dramatic drop in the number of new cases, probably because there were a number of cases that were reclassified. We’ll have to watch this and see how things go.
让我们看一下WorldOmeter。我们可以看到,在xx境外的总案件数量一直保持不变,因为没有重新定义导致大量新案件。让我们看一看,看看中国境内发生了什么事,或总体而言是什么情况。如果我们在这里查看新案例,那么新案例的数量会急剧下降,这可能是因为有许多案例已被重新分类。我们将不得不观看此事,看看情况如何。
Now, remember we’re talking about these total cases is based on the number of people presenting to hospitals that can get work done on them. Based on some reports that we’ve been seeing, especially at New York Times, there’s been a crackdown and a rounding-up of people, and holding them in quarantine, and not getting the medical treatment that they need. Some people of course too scared to go, and not wanting to get treatment, and so it’s unclear exactly how many people are not being counted here, but it’s apparent that this is still being undercounted. In terms of total deaths, there has been a jump, and that doesn’t seem to be cooling off anytime soon, unfortunately. For the same reason why the total number of cases may be underestimated, the total deaths may be underestimated as well.
现在,请记住,我们所说的总病例数是根据向医院求助的人数来完成的。根据我们一直在观察的一些报道,特别是在《纽约时报》上,有人进行了xx和xx,将他们隔离起来,没有得到他们需要的医疗。当然,有些人太害怕了,不想去接受治疗,因此目前尚不清楚到底有多少人没有被计算在内,但显然这仍然被低估了。就总死亡人数而言,这是一个跳跃,不幸的是,这似乎并没有很快消失。出于相同的原因,为什么总病例数可能会被低估,因此总死亡人数也可能会被低估。
On the WorldOmeter, latest updates for February 14. We see that there’s a report from Hubei Province for yesterday that there were 4,823 new cases, including 3095 that were clinically diagnosed. We can see here that the testing was just kind of underestimated in those chronically. 160 new deaths and 8 clinically diagnosed. So we can see that the clinical diagnosis, addition to the count, is greatly influencing the number of new cases; whereas it’s not affecting the number of deaths as much.
在WorldOmeter上,2月14日的最新更新。我们昨天看到湖北省的报告,有4,823例新病例,其中3095例被临床诊断。我们可以在这里看到,对于那些长期以来的人来说,测试只是被低估了。 160例新死亡和8例临床诊断。因此,我们可以看到,除了计数之外,临床诊断还大大影响了新病例的数量。而对死亡人数的影响不大。
Total accumulative cases, we can see here that 15,384 clinically diagnosed we talked about that. What’s interesting here is that 36,000 are currently hospitalized. That’s an incredible amount of people that are hospitalized, and you can see here that 73%, so the vast majority of them are in mild condition whereas 8,000 are in serious condition, and about 4.6% are in critical condition. There’s a number of people that are undergoing medical observation because of either their contact or other symptoms that they may have.
在累计病例总数中,我们可以看到有15384例临床诊断病例。有趣的是,目前有36,000人住院。这是令人难以置信的住院人数,您可以在这里看到73%的人口,因此他们中的大多数处于轻度状态,而8,000人处于严重状况,约4.6%处于严重状况。由于接触或其他症状,很多人正在接受医学观察。
Two new cases in Japan. One of them being a surgeon at a hospital who developed a fever and still continue to work as usual and saw patients for three days. So that’s probably going to have to be followed up on as well. Okay. I want to discuss three things today. I want to talk about the New England Journal of Medicine article that actually we referenced back at the end of January. I want to talk about cell phones in China, and I also want to talk just briefly about sleep and circadian rhythms and some more reading.
日本有两个新案件。其中一名是医院的外科医生,发烧但仍继续照常工作,看了三天病人。因此,可能还必须跟进。好的。我今天要讨论三件事。我想谈一谈我们实际上在一月底引用的《新英格兰医学杂志》。我想谈谈中国的手机,我也想简单谈谈睡眠和昼夜节律以及更多阅读内容。
First of all, let’s talk about the New England Journal of Medicine. So there was this article that was published in the New England Journal, talking about a visitor from Wuhan, China who visited in Germany for business meeting, and it was reported in the New England Journal of Medicine that this woman who came over was asymptomatic, and then when she flew back to China she developed symptoms of fever and the symptoms of the coronavirus later tested positive.
首先,让我们谈谈《新英格兰医学杂志》。因此,有一篇文章发表在《新英格兰杂志》上,谈论的是来自中国武汉的来访者在德国进行商务会议访问,据《新英格兰医学杂志》报道,这位过来的妇女没有症状,然后她飞回中国时出现发烧症状,随后冠状病毒的症状呈阳性。
And when they tested her friends that were at the business meeting in Germany, they had already become sick and then got better, and they tested positive for Coronavirus, and it was touted at that time that this was evidence that coronavirus could be spread even though the patients were asymptomatic.
当他们在德国举行的商务会议上测试她的朋友时,他们已经病了,然后病情好转,他们的冠状病毒测试呈阳性,当时有人吹捧这是即使冠状病毒也可以传播的证据患者无症状。
Well, as it turns out there’s been a correction on this New England Journal of Medicine case, and will post the link in the description. What they found out was that before they printed, they had not actually reached out to this index case from China and discuss what if she actually had symptoms. They reported that she was asymptomatic, but in reality, she actually was symptomatic. In fact, she was taking medications to suppress a fever, and was having very mild symptoms, but was having them nevertheless.
好吧,事实证明,此新英格兰医学杂志的案子已得到更正,并将在说明中发布该链接。他们发现,在他们印刷之前,他们实际上并没有从中国接触到这个索引病例,也没有讨论过她是否确实有症状。他们报告说她没有症状,但实际上,她实际上是有症状的。实际上,她正在服用抑制发烧的药物,虽然症状很轻,但仍然有症状。
So what does this mean? Does this mean that coronavirus does not shed when the patient is asymptomatic? No, there are still people that believe that and they may be correct. All it means is that you can’t use this New England Journal of Medicine case to support that theory. So I think that’s an important distinction that needs to be made, and it tells us that we’ve got to be careful in this world of rapid information that we get it right before we spread the information because spreading false information can have consequences.
那么这是什么意思?这是否意味着患者无症状时冠状病毒不会脱落?不,仍然有人相信,他们可能是正确的。这意味着您不能使用《新英格兰医学杂志》的案例来支持该理论。因此,我认为这是需要区别的一个重要区别,它告诉我们,在当今快速信息的世界中,我们必须谨慎行事,在传播信息之前一定要正确处理,因为传播虚假信息可能会造成后果。
The other thing I wanted to mention was cell phones. We will link to an article also in the New York Times about what they are doing right now in China in terms of cell phone use. Of course in China, they have three cell phone providers that are run by the government, and wherever you go, of course, that phone has GPS, right? So if you go to any particular province, it’s going to keep track of that on the phone. Well, what they’ve currently worked out through these phone companies is if you text a particular number to them, it will show on the phone right in front of you exactly which provinces in China you have been in in the last two weeks, one month, however, they want to do it. And they’re just listing it. And so what’s going on now is people are coming into various places to various checkpoints, the customs agents, the military personnel who are enforcing these bans, are actually asking people as they come off to text on their phone exactly this number, and up there will pop where they have been in the last month or so, and of course if Wuhan is on there or specific province Wuhan is in, pops up.
我想提到的另一件事是手机。我们还将链接到《纽约时报》上的一篇文章,介绍他们目前在中国使用手机的情况。当然,在中国,他们有三家由政府运营的手机提供商,而无论您走到哪里,那部手机都具有GPS,对吗?因此,如果您去任何一个特定省份,它将通过电话xx。好吧,他们目前通过这些电话公司解决的问题是,如果您给他们发一个特定的电话号码,它将在您面前的电话上准确显示您最近两个星期在中国的哪个省份但是,他们想这样做。他们只是列出它。因此,现在发生的事情是人们进入不同的地方到各个检查站,执行这些禁令的海关人员,xx人员实际上是在问人们,当他们下车时正好在手机上发短信给这个号码,然后到那儿会弹出他们上个月左右去过的地方的消息,当然,如果武汉在那儿或武汉所在的特定省份,也会弹出。
They’re in some cases not letting them go, and they’re redirecting them. So I thought I’d make you aware of that. The last thing I want to talk about real quickly is circadian rhythms. Now, there’s been a lot of questions, and what I’m really trying to do is balance how much we talk about the virus and how much we talk about sleep, and this is the reason why I’m really gung-ho here about sleep.
在某些情况下,它们不让它们离开,而是对其进行重定向。所以我想我会让你意识到这一点。我想快速谈论的最后一件事是昼夜节律。现在,有很多问题,我真正想做的是平衡我们谈论该病毒和谈论睡眠的数量,这就是为什么我在这里真的很高兴的原因。睡觉。
Number One is according to the studies that we’ve talked about in our last updates, you can prevent getting the colds with sleeping appropriately up to five times. Imagine if I could tell you that if you took this pill, you could reduce the chances of you getting the coronavirus by 80%, that would be an amazing way of curtailing the R-O (naught), or the spread factor of coronavirus.
第一是根据我们在最近一次更新中谈到的研究,您可以适当地睡眠多达五次,以防感冒。试想一下,如果我能告诉您,如果您服用了这种药,可以将您获得冠状病毒的机会减少80%,那将是减少R-O(零)或冠状病毒传播因子的一种惊人方法。
That’s what we’re seeing, not necessarily the coronavirus but in rhinovirus, and so I think this is actually significant enough in a discussion of what we can do practically. So in that vein of things, there’s been a lot of comments specifically about some things that I wanted to talk about.
这就是我们所看到的,不一定是冠状病毒,而是在鼻病毒中,因此,我认为这在讨论我们可以实际做的事情时实际上意义重大。因此,就我想谈的某些事情而言,有很多评论。
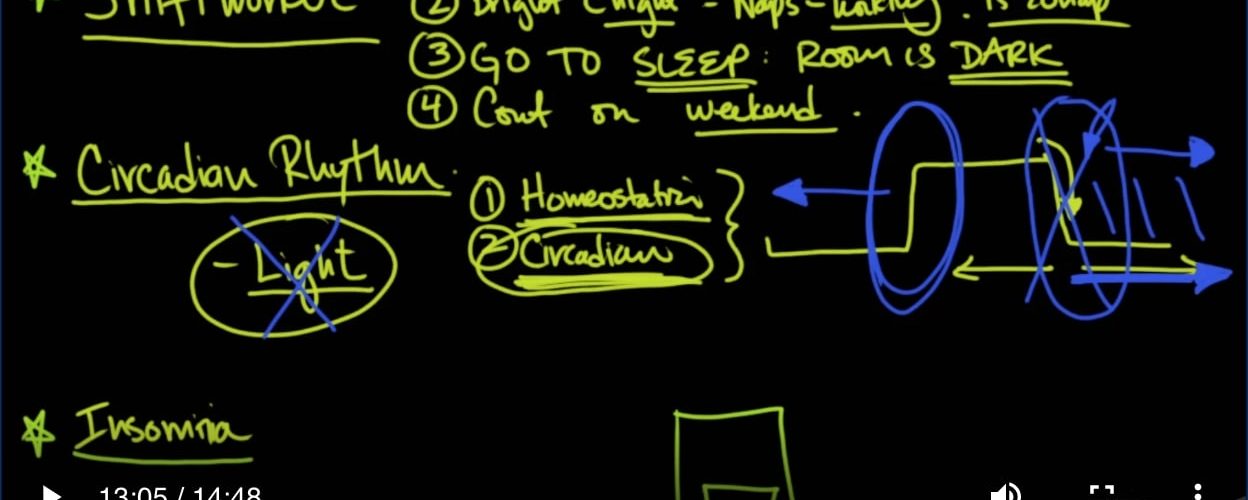
Shift workers, circadian rhythm, lights, and insomnia. First of all, shift workers. I know there’s a lot of health care workers that work night shift. So that’s like going in at 7 p.m. and getting home at 7:00 a.m. Or 6 p.m to 6 a.m., etc. Here’s the key about shift workers. If you’re going to do shift work, it’s better to always do shift work, and not go back between day and night. That’s number one. So stay at same shift. The reason why this is important is because of the second thing we’re going to talk about, and that is your circadian rhythm. If you don’t do that, you confuse your body’s circadian rhythm.
轮班工人,昼夜节律,灯光和失眠。首先,要轮班。我知道有很多医护人员夜班。这就像晚上7点进去一样。并在早上7:00或从下午6点到早上6点等回家,这是轮班工人的关键。如果您要进行轮班工作,最好总是进行轮班工作,而不要在白天和黑夜之间回去。那是第一位。因此,保持不变。之所以如此重要,是因为我们要谈的第二件事,那就是您的昼夜节律。如果您不这样做,则会混淆身体的昼夜节律。
Number two is make sure that your nights are days and that your days are nights. In other words, if you’re going to be up at night, make sure that it is bright where you work at night. It’s also very helpful sometimes to take naps when you’re working if your job allows for that, even if 15 to 20-minute nap can be very restful.
第二个要确保您的夜晚是白天,而您的日子是夜晚。换句话说,如果您要在晚上起床,请确保晚上工作的地方光线明亮。如果您的工作允许,有时在工作时小睡片刻也很有帮助,即使小睡15至20分钟也很轻松。
Number three: if you are a shift worker, and you get home, make sure you go to sleep right away, as soon as you get home. Don’t go out shopping. Don’t do the kids laundry. Don’t go work outside. Go to sleep and make sure that the room is dark. Make sure that the curtains are sealed. Make sure the window is sealed. You are working different shift from what the rest of the world is doing, but you still need your sleep. And so what you need to do is get your circadian rhythm on a completely different cycle, and that way you’re going to get your sleep. The problem occurs is when you want to be one way on the weekends and the other way during the week, that doesn’t work.
第三点:如果您是轮班工人,并且回家了,请确保回家后立即入睡。不要出去逛街不要给孩子洗衣服。不要在外面上班入睡,并确保房间是黑暗的。确保窗帘是密封的。确保窗户是密封的。您的工作与世界其他地方的工作有所不同,但您仍然需要睡眠。因此,您需要做的是在完全不同的周期中获得昼夜节律,这样您就可以入睡。发生问题是,当您想在周末成为一种方式而在一周中成为另一种方式时,这种方式不起作用。
So number four: continue your routine on the weekend. I’m going to put a link into the American Academy of Sleep Medicine website that gives very, very good tips on not only shift workers, but people who have other issues with their sleep.
因此,第四点:在周末继续您的例行工作。我将链接到美国睡眠医学研究院网站,该站点不仅为轮班工作人员提供了非常非常好的技巧,还为睡眠方面有其他问题的人提供了非常好的提示。
So the other thing I want to talk about that affects all of us is circadian rhythm and lights, so there are two cycles that have to be in perfect harmony in your body for you to get the great night sleep. Number one is the homeostatic, and this is just a funny word that tells you basically as you are awake more and more and more, you start to become increasingly more and more and more sleepy; as you sleep more and more, you start to become more and more and more rested. It’s just like eating and hunger, the more you eat the less hungry you are; the longer you go without eating, the more hungry you are.
因此,我想说的另一件事影响着我们所有人的昼夜节律和灯光,因此,为了获得良好的夜间睡眠,必须使体内的两个周期完全和谐。第一个是体内平衡剂,这只是一个有趣的词,它基本上告诉您,随着您越来越清醒,您开始变得越来越困倦。随着您睡眠的增加,您开始变得越来越休息。就像吃饭和饥饿一样,吃得越多,饥饿就越少。您不吃东西的时间越长,您就越饿。
And that’s pretty easy to understand, but there is a bedtime that we have and there’s a wake time that we have, and so the other one is circadian. And this is what happens when you go on a jet plane, and go to different time zone, and you get off, there’s a certain circadian rhythm that occurs. And when both of these are combined together, the perfect thing happens is you are asleep until the morning, and then you wake up, and then you are awake until the evening and then you go to sleep, and what makes you go to sleep all of a sudden, which makes you get tired around 10 o’clock normally or 11 o’clock normally, is the combination of the drive to go to sleep and the drive to stay awake, finally goes away, and both of those combined for you to go to sleep.
这很容易理解,但是我们有一个上床时间,也有一个唤醒时间,所以另一个是昼夜节律。这就是当您乘坐喷气式飞机前往不同的时区并下车时会发生的事情,这会产生某种昼夜节律。当这两种方式结合在一起时,完美的事情发生了:您一直睡到早晨,然后醒来,然后您一直醒着直到晚上,然后才去睡觉,而这使您全部入睡突然之间,这会导致您通常在10点左右或11点左右感到疲倦,是开车进入睡眠状态和开车保持清醒状态的结合,最后消失了,而这两种情况都适合您去睡觉。
The problem is that the circadian rhythm can be shifted either to the left, Advanced, or to the right, Delayed. And what is it that can shift circadian rhythm? It’s light, and this is the thing that is the bane of our existence as people who look at electronic equipment, whether it’s coming from a TV screen, a cell phone, whether it’s coming from the lights in our house. All of those things at that time of the night, when we should be going to bed, especially blue light, is going to delay your circadian rhythm so that you become tired later and later and later. And so what happens is you stay up later and later and later, and you don’t feel tired until later and later and later, but you still have to get up in the morning to beat the traffic, to get into work, which starts at eight, or nine, or whenever it starts.
问题在于,昼夜节律可以向左(高级)或向右(延迟)移动。什么可以改变昼夜节律?它很轻,这就是我们作为查看电子设备的人而生存的祸根,无论它是来自电视屏幕,手机还是来自我们家的灯光。在晚上的那个时候,我们应该上床睡觉时,尤其是在蓝光下,所有这些事情都会延迟您的昼夜节律,使您越来越晚变得疲倦。因此,发生的事情是您迟晚要熬夜,直到以后再迟一点都不会感到疲倦,但是您仍然必须早上起床才能打败交通,开始工作,然后开始八点或九点,或开始时。
So that squeezes the amount of time that you have to go to bed and to get the sleep. So by eliminating light at night, the light that causes this delay in your circadian rhythm, is particularly from blue light, but bright light exposure at the beginning of your day when you’re starting to get up in the morning has the opposite effect, and it can actually advance your circadian rhythm
这样可以减少您上床睡觉所需的时间。因此,通过在夜间消除光线,导致这种昼夜节律延迟的光特别是来自蓝光,但是从早晨开始起床的早晨开始,明亮的光线却产生了相反的效果,它实际上可以提高您的昼夜节律。
So what I tell my patients is that if they have a situation where they’re going to bed very, very late because they don’t feel sleepy until they go to bed very late. And they love to sleep in till 8:00, or 9:00 or 10:00, kind of like my teenager. What they need to do is to advance their circadian rhythm. So what I tell them to do: make sure that they’re exposing their eyes to nice bright light around 7:00 or 8:00 in the morning, and to avoid light exposure late in the evening.
因此,我告诉我的患者,如果他们的情况下他们睡得非常非常晚,因为直到睡到很晚才感到困倦。他们喜欢睡到8:00、9:00或10:00,就像我的少年一样。他们需要做的是提高他们的昼夜节律。因此,我告诉他们要做的事情:请确保他们在早上7:00或8:00左右将眼睛暴露在明亮的光线下,并避免在深夜曝光。
Let’s talk really briefly about insomnia. So some people have an issue with going to bed. And for those of you who have a separate room where your bed is as compared to other parts of your house, this works. But many, many people have the situation where they feel tired. They’re in the kitchen, and as soon as they go into the bedroom now, they are wide awake. They can’t go to sleep, and they become very concerned about their insomnia.
让我们真正简短地谈谈失眠。所以有些人上床睡觉有问题。对于那些与您的房屋其他部分相比拥有单独床铺的房间的人来说,这很有用。但是很多人会感到疲倦。他们在厨房里,现在一进卧室,他们就醒了。他们无法入睡,他们非常担心自己的失眠。
And there’s a number of issues going on here. It has to do with classical conditioning and things like Pavlov’s Dog that you may have heard of an experiment. And the situation is that you’ve got your bedroom, and there are things in your bedroom that you have associated with insomnia, and so that comes to your mind as soon as you go into the bedroom, and you can’t sleep because you see these things that you’ve associated with yourself in your brain for many, many times that you can’t sleep when you’re in this bedroom.
这里有很多问题。它与经典调理以及您可能听说过的实验有关,例如巴甫洛夫的狗。情况是您有卧室,并且卧室中有些东西与失眠有关,因此,一旦进入卧室,您就会想到,而您无法入睡,因为看到这些与您自己的大脑相关的东西很多次,即使您在这个卧室里也无法入睡。
And it’s sort of like a performance anxiety, and it’s because you’ve associated that bedroom with your inability to perform, and the performance that you need to do in that bedroom is sleep. So what do you do? If you cannot sleep in your bed, you should leave your bedroom and go to another part of the house and associate that other part of the house with inability to sleep. We want your bedroom to be associated with you sleeping. So in the same vein, if it’s possible, and you have insomnia, you need to toss out other things in that bedroom that aren’t there for sleep. So in other words, if you have a TV in your bedroom, you should get rid of it; if you read in your bedroom, if you work in your bedroom, you should get rid of it.
这有点像对表现的焦虑,这是因为您已经将那个卧室与您的无力表现联系在一起,而您在那间卧室需要做的表现就是睡眠。所以你会怎么做?如果您无法在床上睡觉,则应离开卧室,转到房屋的另一部分,并将房屋的另一部分与无法入睡联系起来。我们希望您的卧室与您的睡眠联系在一起。因此,如果可能的话,同样,如果您失眠,您需要扔掉卧室中其他不睡觉的东西。因此,换句话说,如果您的卧室里有一台电视,则应该将其删除。如果您在卧室里读书,或者在卧室里工作,就应该摆脱它。
Essentially, there are only two things you should be doing in that bedroom. And one of them is sleeping so that when you go into that bedroom, you are going to associate that very, very strongly with sleep, and you’re going to eliminate the feeling of performance anxiety because you’re not going to be associating that bedroom with inability to sleep, because you will be getting out of bed and going to another part of the house until you are ready to go back to sleep.
本质上,在该卧室中您应该只做两件事。其中一个正在睡觉,所以当您进入卧室时,您将非常非常强烈地将其与睡眠相关联,并且您将消除表现焦虑的感觉,因为您不会与之相关联卧室无法入睡,因为您将起床并进入房屋的另一部分,直到准备好入睡为止。
The reason why people get this is because they watch videos like mine, and they get the wrong impression. They say I must go to sleep earlier. I must get more sleep, so they go to bed earlier when the circadian rhythm is not ready for them to go to sleep, or they say I’m going to sleep in this morning, even though it’s 9,10 o’clock, and it’s time for them to get up, and their circadian rhythm is saying get up, but they stay in bed, and they can’t sleep, and when they can’t sleep, they become more anxious, and when they become more anxious, they associate that with the bedroom, and that causes the issues. So thanks for joining us.
人们之所以会这样做,是因为他们像我一样观看视频,并且得到了错误的印象。他们说我必须早点睡觉。我必须多睡一会,所以当昼夜节律还没准备好让他们入睡时他们会早点睡觉,或者他们说我今天早上要入睡,即使现在是晚上9点10分,并且他们该起床了,他们的昼夜节律说起床了,但是他们躺在床上,无法入睡,当他们无法入睡时,他们变得更加焦虑,当他们变得更加焦虑时,他们将其与卧室相关联,从而导致了问题。感谢您加入我们。

Add comment